Coping with chronic pain, depression, and high blood pressure
Can you prevent the hunched back of kyphosis?

What is ventricular bigeminy?

How gum disease may raise heart disease risk

Smart watch may improve detection of atrial fibrillation

Doing different types of exercise linked to a longer life

Emojis in electronic health records could be confusing

FDA approves nasal spray to treat rapid heart rhythm

CPR on TV may be misleading

4 keys to a heart-healthy diet
Harvard Health Blog
Read posts from experts at Harvard Health Publishing covering a variety of health topics and perspectives on medical news.
Articles
Environmentally friendly inhalers double the cost for people with asthma
Environmentally friendly asthma inhalers may be good for the atmosphere, but they have nearly doubled what people with asthma are paying out of pocket for their inhalers. That’s the take-home message from a study led by Dr. Anupam Jena, an assistant professor of health care policy and medicine at Harvard Medical School and an internist at Massachusetts General Hospital. The findings were published online today in JAMA Internal Medicine. In 2008, the FDA banned a class of asthma inhalers that contained ozone-depleting propellants called chlorofluorocarbons (CFCs). The switch to CFC-free inhalers has led to an average increase of $10 per inhaler prescription, which has effectively doubled their cost.
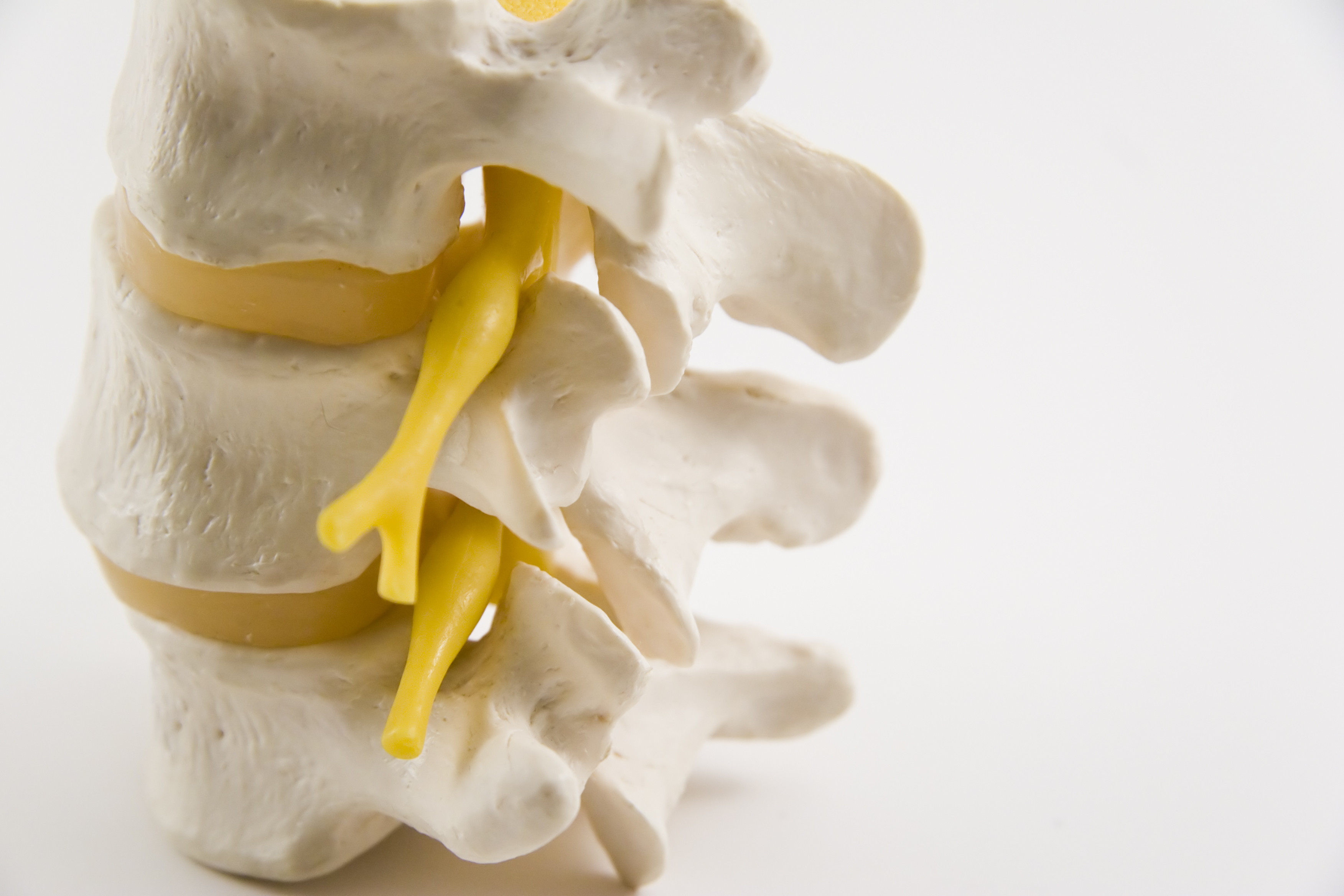
New recommendations aim to improve safety of pain-relieving spinal steroid injections
Each year, several million people with neck or back pain get injections of anti-inflammatory steroid medications. When they work (they don’t always), such injections can bring profound relief. But injecting these medications into the spine can cause partial or total paralysis, brain damage, stroke, and even death. Case reports beginning in 2002 highlighted serious problems linked to spinal steroid injections. In 2014, the FDA started requiring a warning on the labels of injectable steroids. A Viewpoint article in this week’s Journal of the American Medical Association spotlights new safety recommendations to help prevent these rare but real problems. The new recommendations are part of the FDA’s Safe Use Initiative.
Pets can help their humans create friendships, find social support
Pets can provide their owners with more than companionship. A new study, published online in the journal PLoS One, shows that pets can also help create human-to-human friendships and social support, both of which are good for long-term health. The effect isn’t limited to dogs. Other kinds of pets, including cats, rabbits, and snakes, can also be catalysts for making friends and finding social support. In a survey of residents of four cities, being a pet owner was the third most common way that respondents said they met people in their neighborhoods. Pet owners were 60% more likely than non–pet owners to get to know people in their neighborhoods they hadn’t known before. They were also more likely to have reported befriending someone they met through a pet-related connection or getting social support from them. As described in Get Healthy, Get a Dog, a Special Health Report from Harvard Medical School, pet ownership has many direct physical and mental health benefits.
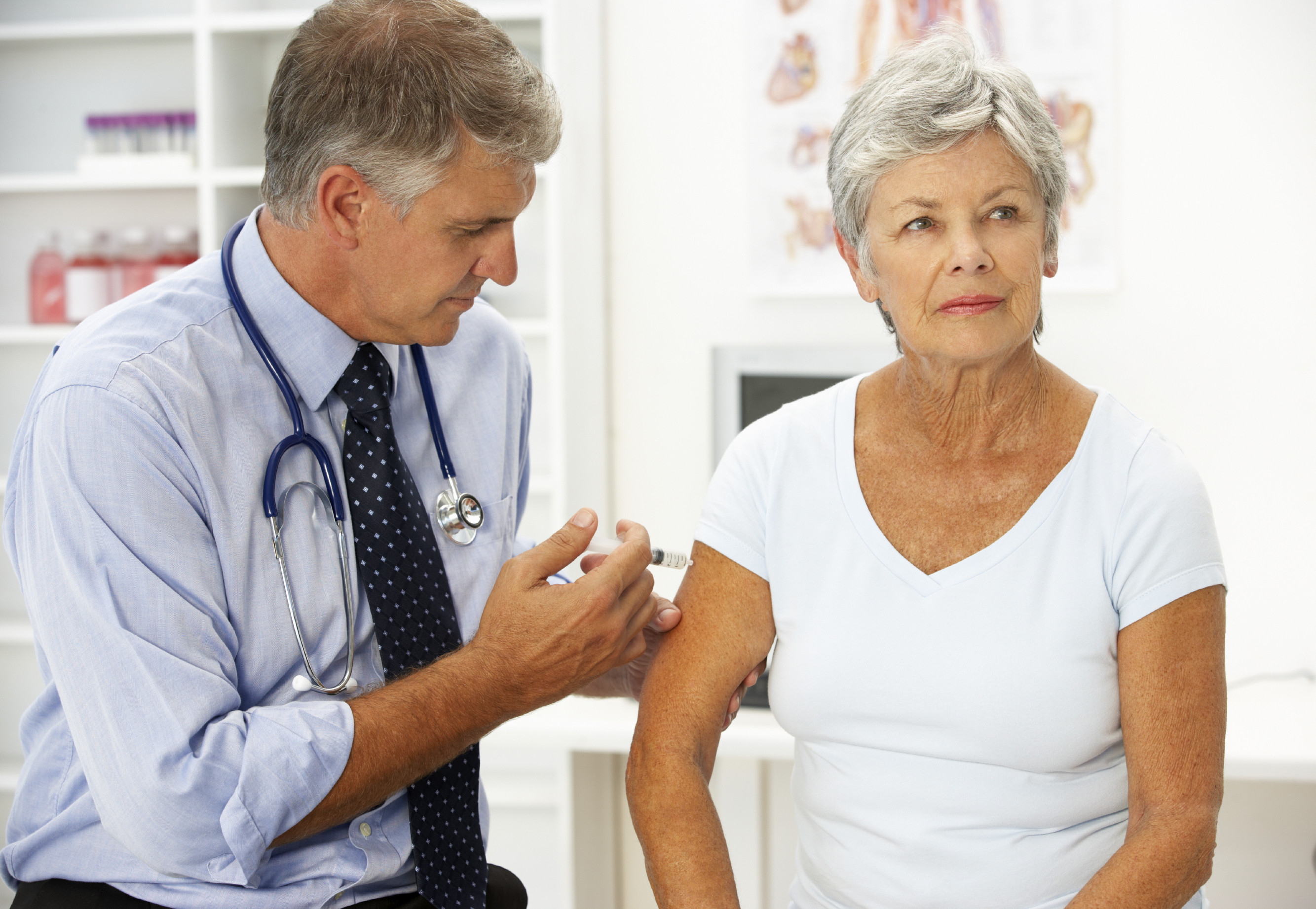
Experimental new vaccine may help in the fight against shingles
If you had chickenpox as a child, the virus that caused it can re-emerge later in life —to cause shingles. This condition, also known as herpes zoster, consists of a rash on one side of the body, often accompanied by excruciating pain. The rash typically goes away in about a month, but in some people, the pain lingers for weeks, months, or even years. This chronic pain is called post-herpetic neuralgia. A vaccine called Zostavax can help prevent shingles. It is recommended for people ages 60 and older. The vaccine is produced by treating live varicella-zoster virus in ways that weaken it but don’t kill it. Though Zostavax works reasonably well to prevent shingles, it tends to be less effective in older people. And because it contains live virus, it should not be given to people with weak immune systems. An experimental new vaccine which goes by the name HZ/su, just described in The New England Journal of Medicine, seems to get around these problems. In the international Zoster Efficacy Study in Adults 50 Years of Age or Older (ZOE-50), the new vaccine appeared to be effective even in older people. It may, however, cause more pain at the injection site and also more frequent muscle pain and headache than the current vaccine. Even if the new vaccine performs well in future tests, FDA approval would still be a few years away.
Should alcoholic drinks come with calorie labels?
Calorie counts adorn the exterior of cans and bottles of sodas, juices, sports drinks, and many other beverages. Should alcoholic beverages and drinks also come with calorie counts? Yes, argues Dr. Fiona Sim, chair of the United Kingdom’s Royal Society for Public Health, in an editorial in The BMJ. She explores well-supported links between alcohol drinking and obesity. Beginning in December 2015, alcohol-related calorie counts will be available in the United States to some people who dine out. The Food and Drug Administration is requiring restaurant chains with 20 or more outlets to provide calorie information for food and some alcoholic drinks. The calorie counts may come as a wake-up call for drinkers who are accustomed to thinking of an average drink as containing 100 to 150 calories. That figure may be true for the standard 1.5-ounce shot of distilled spirits, 12-ounce bottle of beer, or 5-ounce glass of wine, but the “generous pour” at many bars and restaurants often doubles the amount. Moreover, concoctions containing syrups, liqueurs, juices, cream, and other ingredients can send the calories soaring.
Switching to a fiber-rich diet may lower colon cancer risk in blacks
Switching from a “Western” diet with lots of fat and meat to a fiber-rich diet for just two weeks makes conditions in the large intestine less favorable to the development of colon cancer. The opposite switch may promote the formation of cancer. That’s the conclusion from a small but elegant study done in urban Pittsburgh and rural KwaZulu-Natal, South Africa. In the study, 20 volunteers from each area switched diets. For two weeks, the Americans ate a traditional high-fiber African diet rich in fruits, vegetables, nuts, and beans, while the Africans ate a Western diet with more fat, protein, and meat. In just two weeks, significant changes occurred in the lining of the colon and in its chemical and bacterial make-up in both groups, but in different directions. Those following the African diet showed improvements in colon health likely to protect against colon cancer, while those following the Western diet showed changes that could lead to colon cancer.
Special MRI scan could identify stroke risk in people with atrial fibrillation
Atrial fibrillation is a heart rhythm disorder that affects millions of people. It can lead to potentially disabling or deadly strokes. Researchers from Johns Hopkins University School of Medicine adding motion-tracking software to standard MRI heart scans of 149 men and women with atrial fibrillation. The scans revealed specific changes in the muscles of the left atrium that increased stroke risk in some of the volunteers. These changes were not associated with age or other risk factors for stroke. This could help many people with this condition to avoid taking warfarin or other clot-preventing medications for life. But it is much too early to include MRI as part of the standard evaluation of people with atrial fibrillation — not to mention that such scans would significantly increase the cost of these evaluations. For now, doctors will continue to use standard tools to help determine stroke risk.
Hormone therapy works best when combined with radiation for locally advanced prostate cancer
Men with locally advanced prostate cancer who combine hormone therapy with a course of radiation therapy tend to live longer than men who only take hormone therapy.
Number of babies born in withdrawal from prescription painkillers is on the rise
Each year, an alarming number of babies born in the United States spend their first few days withdrawing from drugs, often prescription painkillers their mothers took during their pregnancies. This problem, called neonatal abstinence syndrome (NAS), has increased fourfold since 2004, according to a report published online yesterday in The New England Journal of Medicine. NAS occurs in many babies whose mothers took a type of medication called an opioid during pregnancy. (Two commonly used opioids are OxyContin and Vicodin.) These drugs easily pass from the mother’s bloodstream to the baby’s. In effect, NAS is a baby’s withdrawal from opioids. With medication and time, babies with NAS get better, but they have to spend time in the hospital. In short, they get a rough start on life that can set them back and possibly have long-term repercussions. With so many safe options for pain control, women who are pregnant should use opioids only if these medications are absolutely necessary.
No “best” treatment for common uterine fibroids
Fibroids are noncancerous tumors that grow in the uterus. They may be smaller than a seed or bigger than a grapefruit. Depending on their size, number, and location, fibroids can cause heavy bleeding and long menstrual periods (which can, in turn, cause anemia), pelvic pain, frequent urination, or constipation. Fibroids can also cause infertility and repeated miscarriages. About 7 in 10 women will develop this condition at some point. Given how common uterine fibroids are, it’s surprising how few randomized trials have been done to compare treatment options. A clinical practice article in today’s New England Journal of Medicine lays out the options for treating uterine fibroids and discusses the factors women and their doctors should consider when making treatment decisions.
Hospitalization after fainting can do more harm than good
Fainting can be alarming. Sometimes it’s a signal of a heart or other problem that needs to be fixed. But sometimes it is nothing to worry about, caused by not eating, having blood drawn, or even laughing too hard. Up to one-third of people at low risk for serious short-term problems after fainting end up being hospitalized. A research letter in this week’s JAMA Internal Medicine points out that hospitalization for low-risk fainting can do more harm than good. Just because you’re in the emergency department after fainting doesn’t mean you need to be admitted to the hospital. Ask your physician if you’re at risk for a worse event if you go home, and make sure that if you’re admitted it’s because there’s a potential serious cause for your fainting that can’t be fully assessed in the emergency department.
5 tips to make the Boston Marathon your marathon
On Marathon Monday, thousands of runners will start in Hopkinton, Mass., and finish in Copley Square. Some will glide along, some will lope, and others will shuffle. No matter how they run, or how fast they run, running the Boston Marathon is something special. Here are a few tips to make the Boston Marathon your marathon. 1) Never wear something on marathon day you haven’t worn for a distance run before. 2) If family or friends will be watching you along the route, try to know in advance where they will be. 3. “The wall” is real so have a plan. 4. Try to take in the atmosphere. 5. Enjoy the camaraderie.
Targeted prostate biopsies better at detecting dangerous cancers
Standard biopsies of the prostate gland often miss potentially aggressive prostate cancer. Adding MRI images to standard biopsies improves the detection of prostate cancer.
More than a stretch: Yoga’s benefits may extend to the heart
Yoga is good for the muscles and the mind. New research suggests that it may also be good for the heart. A review of yoga and cardiovascular disease published in the European Journal of Preventive Cardiology indicates that yoga may help lower heart disease risk as much as conventional exercise, such as brisk walking. It can help people lose weight, lower blood pressure and cholesterol, and ease stress. Each of those changes works to prevent heart disease, and can help people who already have cardiovascular problems.
Germanwings Flight 9525 shows the limits of predicting human violence
The tragic story of copilot Andreas Lubitz, the man who apparently crashed Germanwings flight 9525 into the Alps in an act of suicide and murder, demonstrates the opaqueness of mental illness. It is difficult to know when a person is struggling with private psychological and emotional pain that might lead to dangerous or destructive behavior. All of us tend to keep our thoughts, especially our most disturbing ones, to ourselves. Even when encouraged to speak those thoughts aloud — to a mental health professional, for example — it is very difficult to do so. This tragedy will likely spark calls for increased scrutiny of pilots. That’s not necessarily a bad thing, but it could lead to the unintended and undesirable consequence that pilots will become even more wary of seeking help. To honor the lives lost will require policies that protect the public while not being punitive to pilots.
An apple a day may not keep the doctor away, but it’s a healthy choice anyway
This week’s inaugural April Fool’s Day edition of JAMA Internal Medicine carried a report entitled “Association Between Apple Consumption and Physician Visits: Appealing the Conventional Wisdom That an Apple a Day Keeps the Doctor Away.” Based on actual national nutrition data collected from nearly 8,400 men and women it concludes, “Evidence does not support that an apple a day keeps the doctor away; however, the small fraction of US adults who eat an apple a day do appear to use fewer prescription medications.” Apples may have failed this critical scientific test, but they are still an excellent choice as a snack, pick-me-up, or dessert.
Everywhere, hospitals are merging — but why should you care?
Hospitals across America are merging. In 2014 alone, there were 95 mergers, acquisitions, and joint ventures among U.S. hospitals, down only slightly from 98 in 2013. What is fueling this trend toward hospital consolidation — and why should you, as a consumer of health care, be concerned about it? Hospital administrators who create the mergers believe that hospital consolidation improves efficiency, access to care, and quality of care, and may lower costs. In contrast to hospital administrators, many health economists are wary about the growing number of these mergers. When individual hospitals merge into larger systems, they gain a larger share of the consumer health market. That puts them in a position to ask health insurance companies to pay more for medical care and procedures. These higher prices are not borne by the insurers, but by consumers in the form of greater premiums. Thus, some economists argue, mergers drive up health care costs and place added financial pressure on consumers.
Precision medicine is coming, but not anytime soon
President Obama’s announcement of a Precision Medicine Initiative was one of the few items in this year’s State of the Union address to garner bipartisan support. And for good reason. Precision medicine, also known as personalized medicine, offers the promise of health care based on your unique DNA profile and the profiles of a million other individuals. Getting to precision care will require new diagnostic tests. It will also need a new regulatory framework to make sure that technologies aren’t launched before they’ve been proven to be safe and effective, according to a Perspective article in The New England Journal of Medicine. It may take a few years to design this new vetting system and put it in place. In other words, precision medicine is on the horizon, but it isn’t around the corner.
Editorial calls for more research on link between football and brain damage
Is brain damage an inevitable consequence of American football, an avoidable risk of it, or neither? An editorial published yesterday in the medical journal BMJ poses those provocative questions. Chad Asplund, director of sports medicine at Georgia Regents University, and Thomas Best, professor and chair of sports medicine at Ohio State University, offer an overview of the unresolved connection between playing football and chronic traumatic encephalopathy, a type of gradually worsening brain damage caused by repeated mild brain injuries or concussions. The big question is whether playing football causes chronic traumatic encephalopathy or whether some people who play football already at higher risk for developing it. The Football Players Health Study at Harvard University hopes to provide a solid answer to that and other health issues that affect professional football players.
Early scans for back pain add cost but offer little benefit for seniors
Older adults with new back pain usually end up getting a CT scan or MRI. That’s often a waste of time and money and has little or no effect on the outcome, according to a new study from the University of Washington. The results of the study contradict current guidelines from the American College of Radiology. The guidelines say that it’s “appropriate” for doctors to order early MRIs for people ages 70 and older with new-onset back pain, and many doctors do just that. The study, which followed more than 5,200 men and women over the age of 65 who saw a primary care physician for a new bout of back pain, found that people who got early back scans did no better than those who didn’t have scans. The scans added about $1,400 per person to the overall cost of back pain care — with no measurable benefit.
Are you 65 or older? Get two vaccinations against pneumonia
If you or a loved one is age 65 or older, getting vaccinated against pneumonia is a good idea — so good that the Centers for Disease Control (CDC) now recommends that everyone in this age group get vaccinated against pneumonia twice. For the past 30 years or so, the CDC has recommended that everyone ages 65 and older get a single-dose pneumonia vaccine called pneumococcal polysaccharide vaccine 23 (PPSV23). This vaccine is also recommended for those between the ages of two and 64 who are at high risk of getting pneumonia. Findings from a large clinical trial called CAPiTA, published today in The New England Journal of Medicine, show that a second vaccine, called pneumococcal conjugate vaccine 13 (PCV13), provides further protection against pneumonia and related infections. When it comes to preventing pneumonia, the bottom line for older individuals is clear: Get vaccinated twice.
Folic acid, a B vitamin, lowers stroke risk in people with high blood pressure
If you’re among the one in three American adults with high blood pressure, be sure you’re getting plenty of the B vitamin known as folate. Doing so may lower your odds of having a stroke, an often disabling or deadly event linked to high blood pressure. That’s the conclusion of a large trial conducted in China, where many people don’t get enough folate. Most Americans get plenty of folate or its synthetic version, folic acid. That’s largely because grain folic acid is added to most grain products, including wheat flour, cornmeal, pasta, and rice. It’s a good idea for everyone to do a diet check to make sure it delivers enough folate. Good sources include green leafy vegetables, beans, and citrus fruits.

Coping with chronic pain, depression, and high blood pressure

Can you prevent the hunched back of kyphosis?

What is ventricular bigeminy?

How gum disease may raise heart disease risk

Smart watch may improve detection of atrial fibrillation

Doing different types of exercise linked to a longer life

Emojis in electronic health records could be confusing

FDA approves nasal spray to treat rapid heart rhythm

CPR on TV may be misleading

4 keys to a heart-healthy diet
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up