
Trying to lose weight? Be careful not to lose muscle
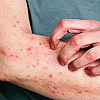
Is your skin problem actually an autoimmune condition?

People with diabetes face higher risk of hearing loss

Antibiotic-free fixes for recurrent UTIs

Musculoskeletal syndrome of menopause: When menopause makes you ache all over
When can older women stop getting mammograms?

To lose weight, especially harmful belly fat, combine diet and exercise

Can men hold off on treating recurring prostate cancer?

The 7 types of rest and why we need them all

What are the early warning signs of cervical cancer?
Medical Devices & Technology Archive
Articles
Can a smart watch diagnose a heart attack?
ECG readings taken with a smart watch may be just as accurate as a traditional ECG done in a medical setting. But the notion of using a smart watch to diagnose a heart attack is still years away. One main reason: obtaining an ECG with a smart watch requires carefully holding the back of the watch on the wrist and at eight specific locations on the chest and abdomen. Quality control and regulatory issues are other important hurdles that need to be addressed. But experts believe improved smart watches with enhanced diagnostic ability may be on the market within a decade.
All about your heart rate
Maximum heart rate refers to the upper limit of what a person's cardiovascular system can handle during exercise. It can be estimated by subtracting the person's age from 220. Target heart rates (which range from 64% to 93% of the maximum) can help people know if they are doing moderate or vigorous exercise. Physical activity guidelines recommend that people get at least 150 minutes of moderate-intensity exercise or 75 minutes of vigorous-intensity exercise, or a combination of both, per week.
A device to prevent strokes in afib
The Watchman, a tiny, basket-like device placed in the heart's left atrial appendage, is designed to prevent blood clots traveling from the heart to the brain and causing stroke. People with atrial fibrillation who face a high risk of bleeding from anti-clotting drugs may be good candidates for the device.
Gene editing: A one-time fix for dangerously high cholesterol?
A gene editing technique that permanently shuts down a cholesterol-raising protein called PCSK9 is being tested in heart attack survivors with an inherited form of high cholesterol. The one-time infusion contains tiny particles that contain the editing tools, which travel through the blood to the liver and changes the cells that produce the protein. If early data show the treatment to be safe and effective, the therapy potentially could be used in people who have "garden variety" high cholesterol.
Simple home medical gadgets to protect your health
The modernization of standard home medical devices has made monitoring health easier than ever. These gadgets include thermometers, scales, blood pressure monitors, and pulse oximeters. Gadget features that are especially helpful for older adults are easy operation and large, lighted readouts. It’s important that some home medical devices, such as blood pressure monitors and pulse oximeters, have a seal of approval from an accredited agency, such as the FDA for pulse oximeters or the Association for the Advancement of Medical Instrumentation for blood pressure monitors.
Over-the-counter hearing aids: What we know so far
Over-the-counter hearing aids are now available in stores and online. They're regulated by the FDA, they don't require a prescription from a doctor, and they're cheaper than prescription hearing aids. But over-the-counter devices are not right for everyone. They're meant only for adults with perceived mild to moderate hearing loss. Before buying a pair, a person should do some homework to find devices with the right fit and features, including a trial period that allows the buyer to return them if they aren't working out.
Most Americans need a large or extra-large blood pressure cuff
A majority of people in the United States need a large or extra-large blood pressure cuff. To ensure an accurate reading, people should check their arm circumference to make sure they're using the correct cuff size.
The inside story on pacemakers
The likelihood of someone needing a pacemaker increases with age. This tiny battery-powered device, implanted into the chest, improves abnormal heart rhythms and improves blood flow if the heart does not pump effectively. By helping the heart maintain more normal function, pacemakers enable many individuals with certain heart conditions to resume their normal lifestyle and stay active longer.
What's the future of remote patient monitoring?
The miniaturization of electronics is leading to the development of next-generation devices to monitor health. People today are using various devices (typically smart watches) to measure their heart rate, the regularity of their heart rhythm, the quality of their sleep, their body temperature, and the levels of oxygen and sugar in their blood. And scientists are working on other devices—such as a thin strip of material that is pasted onto the skin—to constantly measure blood pressure, organ function, or certain body chemicals.
Over-the-counter hearing aids are finally available
In August 2022, the FDA approved a new category of safe, regulated hearing aids to be sold over the counter. The devices are meant only for people with perceived mild-to-moderate hearing loss who need to amplify the volume of sounds around them.

Trying to lose weight? Be careful not to lose muscle

Is your skin problem actually an autoimmune condition?

People with diabetes face higher risk of hearing loss

Antibiotic-free fixes for recurrent UTIs

Musculoskeletal syndrome of menopause: When menopause makes you ache all over

When can older women stop getting mammograms?

To lose weight, especially harmful belly fat, combine diet and exercise

Can men hold off on treating recurring prostate cancer?

The 7 types of rest and why we need them all

What are the early warning signs of cervical cancer?
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up











