The inside story on pacemakers
These devices can help people with heart rhythm issues live long and productive lives.
- Reviewed by Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
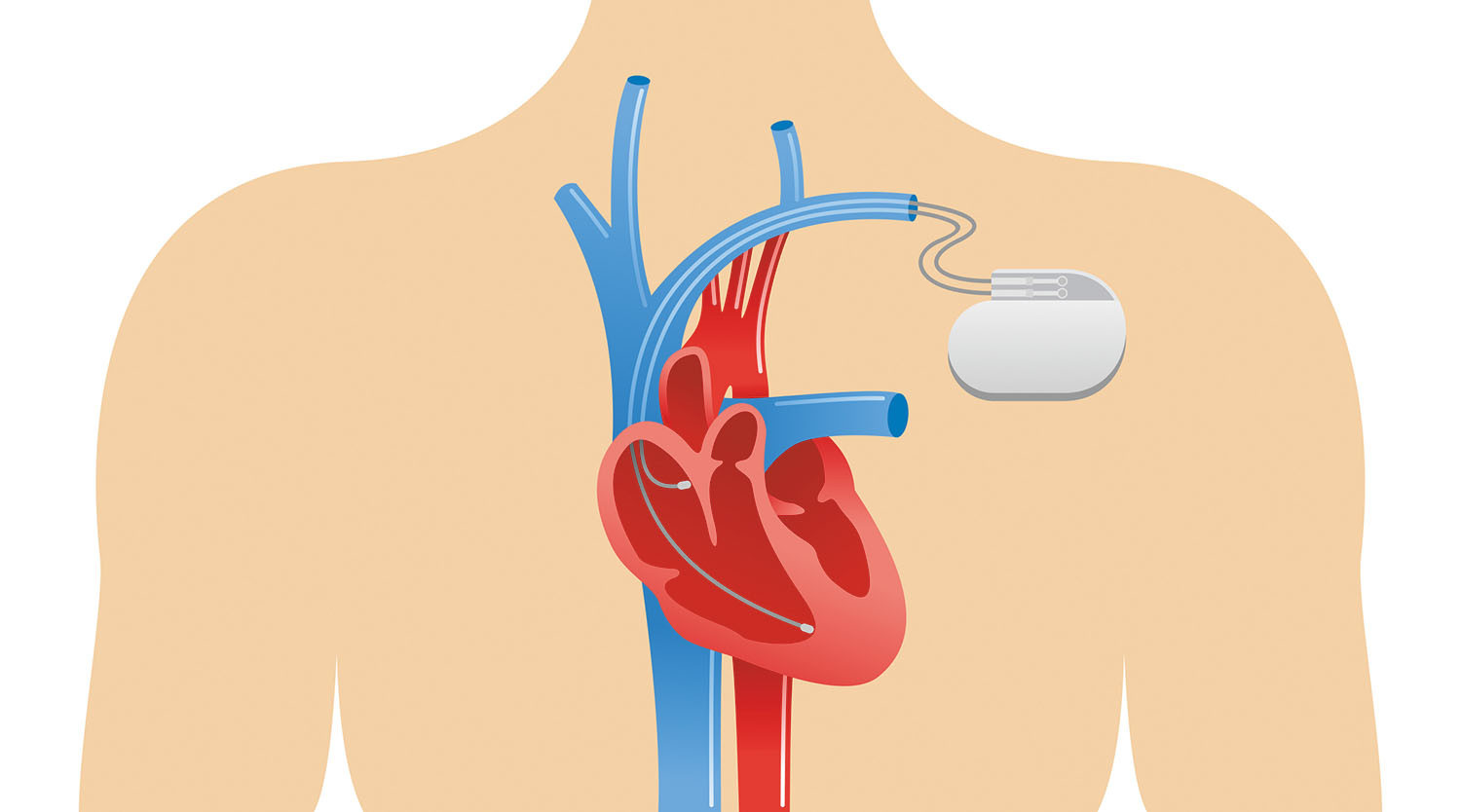
Pacemakers may be seen as a sign of frailty, yet these tiny battery-powered devices help many men maintain a robust lifestyle.
"The likelihood of needing a pacemaker increases with age," says Dr. Sunil Kapur, a cardiologist at the Heart and Vascular Center at Harvard-affiliated Brigham and Women's Hospital. "The good news is that today's pacemakers have evolved from fixing irregular heartbeats to helping the heart maintain its normal function, which allows many men with certain heart conditions to stay active longer."
Who needs one?
A pacemaker monitors the heart's rhythm and, when necessary, generates a painless electrical impulse that triggers a heartbeat.
The most common use for a pacemaker is when the heart beats too slowly or pauses, which triggers dizziness, shortness of breath, or fainting. (You should see your doctor immediately if you have any of these symptoms.) A pacemaker also can help your heart chambers beat in sync and improve blood flow if your heart isn't pumping enough blood. In some cases, a pacemaker may be needed to treat a heartbeat that is too fast or irregular.
These issues can stem from problems with the heart's electrical signaling, a heart defect, an enlarged or thick heart muscle, heart failure, or a heart attack.
Several tests can help your doctor determine if you need a pacemaker: an electrocardiogram, which measures the heart's electrical activity; Holter monitoring, in which you wear a small device to track your heart's rhythm; or an echocardiogram, which uses sound waves to produce images showing your heart's size, structure, and motion.
Can anything disrupt a pacemaker?A constant concern about having a pacemaker is that other electronic devices can disrupt their function. But in most cases, you need not worry, according to Dr. Sunil Kapur, a cardiologist at Brigham and Women's Hospital. For example, cellphones and microwave ovens don't affect most pacemakers. "Even MRI scans are now safe for some people with pacemakers," he says. The American Heart Association has more information about other devices and situations that can interfere with pacemakers; see /pacemaker. |
An inside look
Pacemakers are typically made of titanium and weigh as little as one ounce. They have two working parts: a pulse generator with a lithium-ion battery and one or more flexible wires called leads (pronounced "leeds").
Pacemaker surgery lasts one to two hours. You are awake during the procedure and given a mild sedative. Your upper chest is numbed, and the surgeon makes an incision of two to three inches near your collarbone to access a large vein. The surgeon then creates a small pocket in the skin between the shoulder and chest and inserts the pulse generator.
The leads are connected to the pulse generator, threaded through the large vein, and attached to the heart's surface with electrodes. These electrodes pick up the heart's natural electric signals. When the heartbeat is abnormal, the pulse generator sends a programmed pulse along the leads to the heart muscle to make the necessary correction.
"The surgery is relatively minor and has become much more routine in the past 10 years," says Dr. Kapur. "It's usually a same-day procedure, where you arrive in the morning and are home by that afternoon." A small bulge remains where the pulse generator was inserted. Although pacemakers are generally safe, rare complications can occur. These include infection, excessive bleeding, a tear in the heart, a punctured lung, or a blood clot.
After a few weeks of healing, you'll have a post-op check-up. From there, you have scheduled check-ins every three to six months and eventually only once a year. "Check-ups are to make sure the pacemaker and your heart are functioning well, and the battery has a good charge," says Dr. Kapur.
But technology now exists where patients can transmit the pacemaker's performance information remotely for their doctor's review, eliminating many routine office visits.
A pacemaker's battery lasts from five to 12 years depending on how frequently the pacemaker is in use. When a new battery is needed, the entire pulse generator is replaced through the same procedure, but the leads are often not changed.
Lifestyle approaches
You often don't have to adjust your lifestyle with a pacemaker. "We encourage people to return to their normal routine as soon as possible after the healing phase," says Dr. Kapur.
One caveat is to be mindful of repetitive motions in the upper body. For instance, regularly using arm-strengthening machines, rowing or kayaking, and other similar arm movements can cause a lead to bend and relax repeatedly at the same spot. Over time, this can damage the lead.
"Still, it's fine to exercise your upper arms as long as you don't overdo it," says Dr. Kapur. Ask a trainer about exercises suitable for someone with a pacemaker. If you practice yoga, stick to gentle classes or chair yoga and tell the instructor you have a pacemaker.
In general, moderate-intensity aerobic exercise such as brisk walking or cycling is acceptable for people with pacemakers. In fact, you may notice your overall fitness improve since the pacemaker will correct a previously slow heart rate. But check with your doctor about any concerns over how much and how intensely you can exercise.
Image: © Dmitry Kovalchuk/Getty Images
About the Author

Matthew Solan, Former Executive Editor, Harvard Men's Health Watch
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.
















