Insulin resistance in women and why it rises after 50
The condition, which can lead to diabetes, shows up with an array of easy-to-miss signs.
- Reviewed by Nancy Oliveira, MS, RD, LDN, CDCES, Contributor; Editorial Advisory Board Member, Harvard Health Publishing
Many middle-aged women who consult dietitian Nancy Oliveira point to their bellies, dismayed. Since menopause, they've noticed that extra pounds seem to go straight to their middle.
Cosmetic matters aside, these women may have another reason for concern: the weight shift could signal they're developing insulin resistance, when the pancreas makes insulin but the body's cells don't use it efficiently.
Insulin helps cells take in sugar from the blood to use for energy. But insulin resistance disrupts this process, causing sugar to build up in the bloodstream. Unchecked, the cycle can be a slippery slope to prediabetes and type 2 diabetes as well as a variety of other serious health problems, says Oliveira, manager of the Nutrition and Wellness Service at Harvard-affiliated Brigham and Women's Hospital.
"When your body can't use insulin, your blood sugar will continue to rise higher and higher," explains Oliveira, who is also a certified diabetes care and education specialist. "Then your pancreas continues to secrete even more insulin. Chronically high insulin levels really stress the pancreas, causing it to work overtime. Eventually, this can permanently damage cells in the pancreas."
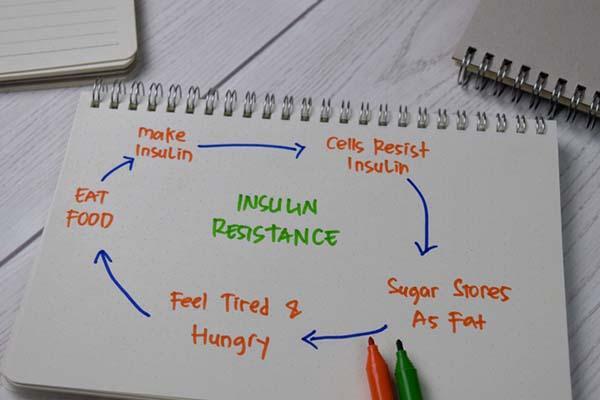
Chain reaction
With nearly four in 10 Americans classified as obese, insulin resistance is highly common in both sexes. That's because excess body fat interferes with how insulin is supposed to work.
Insulin resistance can be a precursor to prediabetes (in which blood sugar levels are elevated, but not high enough to be diagnosed as diabetes) or diabetes itself, which affects nearly 12% of Americans and more than 29% of people 65 and older. But women seem to hit an inflection point in their risk for insulin resistance after 50. Why?
The transition to menopause brings diminished estrogen and progesterone levels, a shift that leads the body to store fat in the belly - a location associated with insulin resistance. The resulting chronically high insulin levels promote additional fat storage, again concentrated in the abdomen. "It's sort of a vicious cycle," Oliveira says.
Moreover, when those additional fat cells break down, they release what are called free fatty acids - fat molecules that flow freely in the bloodstream - as well as inflammatory chemicals called cytokines. "This triggers changes in how cells use energy, possibly leading to insulin resistance," Oliveira says.
Insulin resistance symptoms
Aside from extra belly fat, if you're developing insulin resistance, you might notice signs such as
- "crashing" after meals
- brain fog or difficulty concentrating
- increased hunger
- fatigue
- mood swings
- gradually rising blood pressure, cholesterol, or blood sugar levels, even if still within normal ranges
- skin tags in the armpits or groin.
Beyond prediabetes and diabetes, insulin resistance can cascade into many other health issues, including
- chronic, low-grade inflammation
- high blood pressure
- cardiovascular disease
- fatty liver disease, in which extra fat builds up in the liver and hinders its function.
Your doctor can use a variety of blood tests to determine if you're developing insulin resistance. Regardless of risk factors, the American Diabetes Association recommends all adults 35 and older be screened at least once every three years for prediabetes and diabetes. This typically involves a simple blood test for hemoglobin A1c, which offers a picture of your average blood sugar levels over the prior two to three months.
"If you're at higher risk for insulin resistance because family members have diabetes or cardiovascular disease, you can request an A1c test at an earlier age," she says.
Steps to combat insulin resistanceInsulin resistance is increasingly common as we get older, but not inevitable. Nancy Oliveira, a dietitian at Brigham and Women's Hospital, suggests these strategies to hinder it: Practice time-restricted eating. A form of intermittent fasting, this is an eating pattern where you eat all meals within a set window of time each day. "I suggest 12 to 14 hours overnight without eating. It supports a metabolic cleanout, and the body also uses free fatty acids more effectively when there's no food we're still trying to digest," she says. Eat healthfully. Prioritize eating fruits, vegetables, and lean proteins such as poultry and fish, she says. Cut down on highly processed carbohydrate foods, which tend to spike blood sugar levels. Seek sound sleep. Experts recommend getting a minimum of seven hours each night. Poor sleep tends to drive up blood sugar levels, partly by making the body less responsive to insulin. Move your body. Aim for a minimum of 150 minutes per week of moderate-to-vigorous exercise, as well as two to three days a week of strength training. Oliveira recommends engaging in longer stretches of walking, biking, and other moderate-intensity movement and not just shorter high-exertion activities like running, since this approach may be more effective at burning free fatty acids stemming from extra belly fat. "I recommend that people do a variety of exercise types," she says. "Don't stop running if you love it, but consider a longer walk or hike outdoors at lower intensity as well." |
Image: © syahrir maulana/Getty Images
About the Author

Maureen Salamon, Executive Editor, Harvard Women's Health Watch
About the Reviewer

Nancy Oliveira, MS, RD, LDN, CDCES, Contributor; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.












