Can you stop blood thinners after an ablation for atrial fibrillation?
Some people with this common heart rhythm disorder may safely stop taking certain anti-clotting medications after a successful catheter ablation.
- Reviewed by Sunil Kapur, MD, Contributor
In recent years, catheter ablation has become a routine, first-line procedure for treating the fast, chaotic heart rhythm that characterizes atrial fibrillation. When successful, this minimally invasive therapy may allow some people to stop taking certain anti-clotting medications, according to a study in the Nov. 8, 2025, issue of The New England Journal of Medicine.
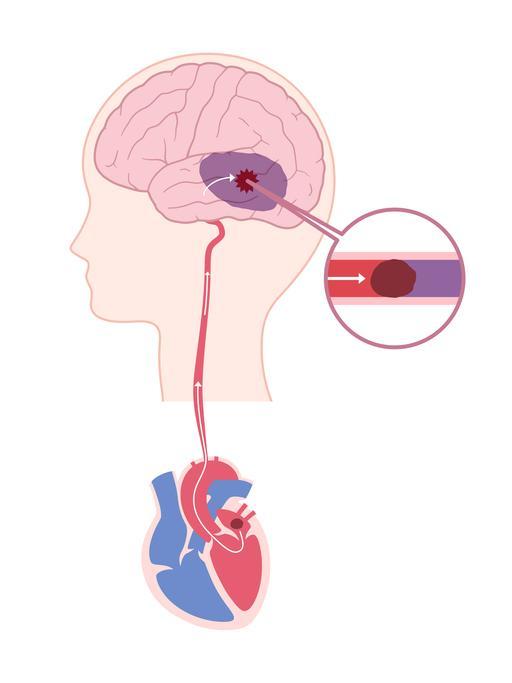
Atrial fibrillation (called afib for short) can cause blood to stagnate and form clots in the heart's upper chambers (atria). Because a clot may travel to the brain and trigger a stroke (see illustration), many people with afib take anti-clotting medications, commonly known as blood thinners (see "Clot prevention for afib").
Afib can also cause symptoms such as palpitations, fatigue, shortness of breath, dizziness, and fainting. Originally, catheter ablation was reserved for people experiencing symptoms. But improvements have spurred wider use of the technique, including in people without symptoms. And growing evidence suggests that earlier ablation treatment may prevent afib from worsening.
After a successful ablation, people often ask if they can stop taking their anti-clotting drug. "From a patient's perspective, ablation can feel like a 'fix,' so it's natural to ask whether that medication is still necessary," says Dr. Sunil Kapur, a cardiologist at Harvard-affiliated Brigham and Women's Hospital. However, the answer depends much more on their underlying risk of stroke than whether the ablation seems successful, he adds.
|
Image: © float/Getty Images |
Who might consider forgoing blood thinners?
People who might be good candidates for stopping anti-clotting drugs after a catheter ablation are typically those who have a low risk of stroke to begin with. In general, that means people who are younger than 65 who've never had a stroke and who have no major risk factors like heart failure, high blood pressure, or diabetes. But the decision should be made cautiously, in consultation with your doctor after a period of careful follow-up after the procedure. Don't stop taking your anti-clotting medication unless your doctor agrees that would be a safe choice for you, says Dr. Kapur.
People at high risk of stroke should definitely not stop taking their pills - especially anyone who's already had a stroke or transient ischemic attack, people 65 and older, and people with multiple risk factors for cardiovascular disease. In these people, ablation does not reliably eliminate the risk of stroke, even if their afib episodes are less frequent or no longer noticeable. "For them, continuing anti-clotting medication remains strongly recommended," says Dr. Kapur.
Clot prevention for afibPeople with afib often take anti-clotting medications, which usually means a direct oral anticoagulant, or DOAC. This drug class includes
DOACs are easier to use than an older anti-clotting drug, warfarin, which requires frequent monitoring and interacts with many foods and medications. But warfarin is a better choice for certain people, including those with mechanical heart valves or moderate to severe mitral stenosis. |
Common concerns and misconceptions
People worry about the cost, inconvenience, and potential side effects of taking of anti-clotting medications indefinitely. The drugs interfere with the body's normal reaction to suppress bleeding. This leaves people vulnerable to minor or more dangerous bleeding. But, for those with atrial fibrillation who are prescribed blood thinners, the potentially catastrophic effects of a stroke generally outweigh those bleeding risks, especially for people already at risk for stroke.
Others are surprised to learn that afib can recur silently, without symptoms, after an ablation. "A big part of the conversations I have with my patients is helping them understand that blood thinners are prescribed to prevent stroke - not to treat symptoms. Feeling better doesn't always mean the underlying risk is gone," says Dr. Kapur.
A device to prevent strokes caused by afib?
What about people who should not take (or cannot tolerate) anti-clotting drugs indefinitely, such as those who have already experienced serious bleeding or face a high risk of bleeding or falling (which raises the risk of bleeding)? A nondrug alternative called a left atrial appendage closure device might be a good option. (Most blood clots form in the left atrial appendage, a tiny pouch that hangs off the upper left side of the heart.) One of these devices - a tiny filter that traps clots, called Watchman - may enable people to stop taking anti-clotting drugs. It is sometimes implanted at the same time as the ablation procedure.
Image: © Nadzeya Haroshka/Getty Images
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
About the Reviewer

Sunil Kapur, MD, Contributor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.