
Driving with arthritis pain: Stay comfortable — and safe — behind the wheel

Daily cup of coffee may prevent afib recurrence
Gene-editing therapy lowers harmful blood fats in early study

What is EMDR therapy, and who can it help?
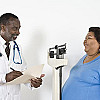
GLP-1 drugs versus bariatric surgery for treating obesity

Two dumbbells, three exercises, and 10 minutes

Easing the emotional burden of IBS

Modify your push-ups to meet your fitness level
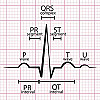
What is long QT syndrome?

Stroke survivors may benefit from very low LDL levels
Hearing loss
- Reviewed by James Naples, MD, Contributor; Editorial Advisory Board Member, Harvard Health Publishing
A person’s hearing naturally declines with age. The National Institute on Deafness and Other Communication Disorders estimates that about one in three adults between the ages of 65 and 74 has some hearing loss, and almost 50% of people age 75 or older have difficulty hearing.
However, people of all ages can experience hearing loss from other causes, such as infections, medication side effects, exposure to loud noises, and genetic causes.
While most people can function with some degree of hearing loss, ignoring hearing decline can profoundly affect one’s health. Hearing loss is associated with cognitive decline, memory loss, depression, and social isolation.
The good news is that there are many types of hearing aids and surgical options available to help with all types and severities of hearing loss.

Driving with arthritis pain: Stay comfortable — and safe — behind the wheel

Daily cup of coffee may prevent afib recurrence

Gene-editing therapy lowers harmful blood fats in early study

What is EMDR therapy, and who can it help?

GLP-1 drugs versus bariatric surgery for treating obesity

Two dumbbells, three exercises, and 10 minutes

Easing the emotional burden of IBS

Modify your push-ups to meet your fitness level

What is long QT syndrome?

Stroke survivors may benefit from very low LDL levels
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up

