GLP-1 drugs versus bariatric surgery for treating obesity
How do the new weight-loss drugs stack up against surgery? And when might a combined approach help?
- Reviewed by Eric G. Sheu, MD, PhD, Contributor

Prescriptions for the weight-loss drugs known as GLP-1s - especially semaglutide (Wegovy) and tirzepatide (Zepbound) - have surged in recent years. Meanwhile, the number of weight-loss surgeries has declined. Known as bariatric surgery, these procedures remove or bypass part of the stomach.
Many people in America meet the criteria for these proven obesity treatments (see "Who qualifies for weight-loss therapies?"). "But obesity is a chronic, complex disease, so it may not be an either-or situation, as some people may benefit from a combined approach," says Dr. Eric Sheu, associate professor of surgery at Harvard Medical School and chief of bariatric and foregut surgery at Brigham and Women's Hospital. Here's what you should know about how (and how well) both options work - not just for weight loss but also for reducing your risk for serious health conditions linked to excess weight.
Who qualifies for weight-loss therapies?GLP-1s usually are prescribed only for people with a body mass index (BMI) of at least 30 - or at least 27 for people with one or more of these weight-related medical conditions:
For bariatric surgery, the BMI cutoff used to be at least 40 (or at least 35 with a weight-related condition). In recent years, obesity and diabetes organizations have advocated for lowering the cutoffs to 35 and 30, respectively. Some (but not all) insurers are now covering bariatric surgery for people at those lower thresholds. You can calculate your BMI at the website of the National Institutes of Health. |
GLP-1s versus surgery: How do they work?
GLP-1 stands for glucagon-like peptide-1, a naturally occurring gut hormone that helps control blood sugar and appetite. GLP-1 receptor agonist drugs (called GLP-1s for short) like semaglutide work by mimicking this hormone, increasing insulin release (which helps control diabetes), signaling your brain that you're full, and slowing digestion. Tirzepatide mimics GLP-1 and another hormone with similar effects called gastric inhibitory polypeptide (GIP).
Most of the GLP-1s for weight loss are injected once weekly under the skin of your abdomen, thigh, or upper arm, using a penlike device with a needle the width of a human hair. In studies, people lost 15% to 20% of their body weight, on average.
The two most common types of bariatric surgery are sleeve gastrectomy and gastric bypass (see illustrations). Both approaches are minimally invasive, meaning they involve very small incisions and usually require just one night in the hospital. Both surgeries reduce the size of the stomach, but more importantly alter your body's secretion of gut hormones that regulate hunger and metabolism, Dr. Sheu explains. "For example, the surgeries increase GLP-1 and GIP levels in the body, which is a key reason they trigger weight loss," he says. In addition, diabetic control improves within days of the surgery. Weight-loss drugs under development aim to mimic other gut hormones that change after bariatric surgery, he adds.
Gastric bypass leads to the greatest weight loss (about 33%) and shows the greatest success for resolving diabetes. But sleeve gastrectomy is a simpler, shorter procedure. It accounts for about 70% of all bariatric surgeries and leads to an average weight loss of about 25%.
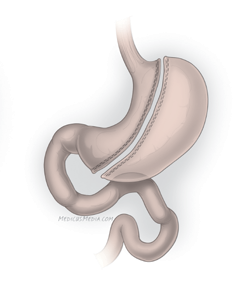
Gastric sleeve
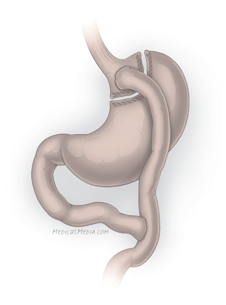
This surgery removes about 80% of the stomach, leaving a banana-shaped tube. It's less invasive than gastric bypass because the small intestine is not cut. Gastric bypass
Gastric bypass converts the upper stomach into an egg-sized pouch and reroutes the small intestine to the pouch. Illustrations by Scott Leighton |
GLP-1s: Promise and problems
"GLP-1 medications are great, and there are similar promising drugs in the pipeline," says Dr. Sheu. Future drugs may be easier to take and have fewer side effects. For example, a pill form of semaglutide for weight loss (called the Wegovy pill) became available in early January 2026.
GLP-1s can produce side effects such as nausea, vomiting, and diarrhea. "And their real-world effectiveness is about half of what's been reported in the clinical trials, probably because most people stop taking them, often for a combination of reasons including side effects, cost, and access," say Dr. Sheu. To maintain your weight loss, you have to take the drugs for the rest of your life, which many people don't realize, he adds. Initially, the average cost ranged around $1,000 per month, but prices are in flux and have dropped recently. Insurance coverage varies widely but is less common for people without related health conditions.
Pros and cons of bariatric surgery
A 2025 study in Nature Medicine that compared GLP-1 drugs to bariatric surgery found that people who had surgery lost more weight and had far fewer serious health problems - including heart attacks, strokes, kidney disease, and diabetes-related eye damage - during the follow-up period, which lasted a median of nearly six years. However, more than half of the people using GLP-1s were taking earlier, less effective versions.
For people with both obesity and diabetes, surgery is clearly more effective than GLP-1s for preventing deaths from cardiovascular disease, Dr. Sheu says. That benefit far outweighs the small risk associated with surgery, which has a complication rate lower than hip replacement surgery. And studies show that most people maintain their weight loss for up to a decade.
Surgery costs between $17,000 and $26,000 and is typically covered by insurance. But the procedures require several weeks of recovery, are irreversible (with rare exceptions), and require lifelong dietary changes.
A combination approach?
These days, most people who consider bariatric surgery have already tried GLP-1 drugs without success, says Dr. Sheu. After bariatric surgery, the resulting hormone changes persist to different degrees. "A year or two after surgery, some people regain their hunger response and put on weight," says Dr. Sheu. For them, GLP-1s can be a good option to help maintain their weight loss. "The two therapies may work best in combination, but we're still trying to figure out the best sequence and timing," he adds.
Image: © IPGGutenbergUKLtd/Getty Images
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
About the Reviewer

Eric G. Sheu, MD, PhD, Contributor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.