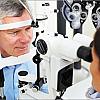
Risk factors for MCI and dementia
Certain factors can affect your risk of developing MCI, such as genetics, health conditions, and lifestyle.
- Reviewed by Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing

© Hispanolistic | Getty Images
Because MCI is very often a harbinger of coming dementia, many of the risk factors that have been identified are the same as those for vascular dementia or neurodegenerative conditions such as Alzheimer's disease. Your risk for these conditions also plays a large role in determining whether or not MCI will progress to a more serious form of dementia.
Personal and family medical history
The roots of MCI may lie in factors you can't control, such as your age and genetic makeup. However, knowing these risks can help prompt you to make lifestyle and health choices that promote cognitive health.
Age. By far, the strongest risk factor for dementia, particularly Alzheimer's disease, is age. Aging is also the key predictor in the progression of MCI to dementia resulting from Alzheimer's disease. In people younger than age 50, MCI is unlikely to be from a degenerative brain disease, unless the person has a strong family history of early-onset dementia.
Race and ethnicity. Rates of Alzheimer's disease and related dementias among older adults of African American and Latino descent are higher than they are among non-Hispanic whites of similar ages. In addition, the number of new dementia cases among these ethnic groups is increasing at a faster pace than the national average.
While there is some evidence that genetic differences may contribute to higher Alzheimer's disease rates among Black Americans, researchers do not believe that this accounts for the bulk of the discrepancy. Instead, they point to factors such as higher prevalences of cardiovascular (heart and blood vessel) risk factors among these groups, including high blood pressure and diabetes, as well as socioeconomic considerations such as poor access to health care.
Genetics. Scientists have identified a cluster of rare variations in three genes - APP, PSEN1, and PSEN2 - that determine whether a person will develop Alzheimer's disease, especially in midlife. People who inherit one of these genes from their parents have a nearly 100% chance of developing Alzheimer's disease.

© Jian Fan | Getty Images
The APOE4 gene variant is associated with an increased risk of developing Alzheimer's disease, including in people with MCI.
A particular common variant of a different gene, known as APOE4, has been associated with increased risk of later-life Alzheimer's disease. Unlike the rare genes mentioned above, APOE4 does not determine whether or not you will develop Alzheimer's disease. Rather, it tells you if you have a greater or lower risk. About 25% of the general healthy population have the APOE4 gene, while about 65% of individuals with Alzheimer's disease have it. Studies have also suggested that people with MCI who carry this gene variant may be more likely to progress to dementia due to Alzheimer's disease.
Several studies have turned up additional genes and gene mutations that may increase susceptibility for Alzheimer's disease. Compared with APOE4, these genes are rare or increase risk only modestly. Some of the newly discovered genes are linked to cholesterol and inflammation, which have been implicated as potential contributing factors in Alzheimer's disease.
In addition, frontotemporal dementia is closely linked to a family history of dementia, as well as to certain genetic variations.
Stroke. Roughly one in 10 of those who have been diagnosed with a stroke will go on to develop dementia. That number jumps to one in three among people who have had multiple strokes. Cardiovascular risk factors such as high blood pressure, high cholesterol, diabetes, and obesity contribute to vascular damage in the brain, which can lead to MCI and vascular dementia, as well as to an increase in stroke risk.
Head injury. Repeated mild head trauma, such as the type likely to be encountered in some sports, can lead to cognitive impairment, mood and personality changes, and speech and movement problems that often occur in people with Parkinson's disease. Moderate or severe traumatic brain injuries caused by a blow or jolt to the head that results in a temporary loss of consciousness or memory can lead to a two- to fourfold increase in the risk of Alzheimer's disease.
COVID-19 infection. Emerging evidence is suggesting that people who survive a COVID-19 infection, particularly those who have been hospitalized, may be subject to long-term cognitive deficits, especially in the area of sustained attention. Scientists speculate that the virus may cause brain injury through direct damage caused by infection, overactive immune response, stroke, or lack of oxygen. Strokes due to COVID are common, particularly in people over 70. It is, however, still unknown what the long-term outcomes of COVID-related cognitive impairment are - specifically, whether it leads to dementia. To answer this question, studies are needed to follow people who have cognitive impairment linked with COVID-19 over time.
Cardiovascular risks
Many studies show that the same conditions that harm the heart and blood vessels also increase the risk of vascular dementia, Alzheimer's disease, and MCI.
High cholesterol. People with high total cholesterol or LDL cholesterol face increased odds of experiencing cognitive decline later in life. The connection may be even stronger in people who have Alzheimer's-related genes.
Diabetes. People with either type 1 or type 2 diabetes face a greater risk of Alzheimer's disease and vascular dementia. In fact, type 2 diabetes, which is often linked to obesity and lack of activity, appears to double or triple the odds of developing Alzheimer's disease. Not surprisingly, diabetes is also linked to a significantly higher chance of developing MCI, especially the amnestic form (aMCI). Research indicates that this increase in risk may reflect a shared mechanism: a deficiency or dysfunction of insulin, the hormone that enables cells in the body to use blood sugar (glucose). Brain cells need glucose to function, and in particular to execute a high-energy task such as learning a skill or forming a memory.

© Mayur Kakade | Getty Images
High blood pressure increases the risk of Alzheimer's and vascular dementia, and research suggests that intensive blood pressure control may slow development of MCI in older adults.
High blood pressure. People with high blood pressure are at increased risk of both Alzheimer's disease and vascular dementia, which frequently coexist. Controlling blood pressure is key to stroke prevention, which is instrumental in staving off cognitive decline. Intensive blood pressure control versus standard therapy has also been shown to slow the development of MCI in older adults.
Metabolic syndrome. A growing body of evidence suggests that a complex problem called metabolic syndrome also raises risk for MCI and the progression to dementia. Metabolic syndrome is characterized by the presence of three or more of the following factors: a large waistline, high blood pressure, high triglycerides, low HDL (good) cholesterol, and difficulty regulating blood sugar. Metabolic syndrome also significantly raises the risks for stroke, heart disease, and diabetes, all of which can contribute to cognitive decline.
Obesity. Research points to excess weight in midlife as a risk factor for Alzheimer's disease and other forms of dementia. (Overweight is defined as having a body mass index, or BMI, of 25 to 29. Obesity is a BMI of 30 or more. To determine your BMI, visit /BMI.) Paradoxically, unintended weight loss in later life has been linked to a higher risk of developing MCI. Researchers hypothesize that this disparity might indicate that weight loss in older people signals the beginnings of another underlying health condition.

© SimpleImages | Getty Images
People who smoke are more likely to develop MCI, Alzheimer's disease, and vascular dementia.
Smoking. Smoking is a risk factor for heart disease, and it also makes you vulnerable to MCI, Alzheimer's disease, and vascular dementia. A scientific review pooling results from 19 different studies estimated that current smokers faced a nearly 70% higher risk of dementia than those who had never smoked. Other research has revealed a connection between secondhand smoke and dementia.
Atrial fibrillation. Atrial fibrillation (afib) is the most common type of heart arrhythmia. Some people with this heart condition may notice dizziness, shortness of breath, and fluttering, but the vast majority experience no symptoms at all. Complications from afib are a major cause of stroke. However, poor blood flow to the brain due to afib also can lead to inflammation, tissue damage, hemorrhage, and brain shrinkage - all of which raise dementia risk. A 2023 population-based study that analyzed data from more than 400,000 participants in the United Kingdom found that people who were diagnosed with afib at a younger age had a higher risk of dementia from all causes than people who developed the arrhythmia later in life.
Other health conditions
Researchers have identified certain health conditions that often occur along with the development of MCI and its progression to dementia. Doctors will screen for these disorders as part of the evaluation for MCI.
Depression. Studies have found that depression in midlife appears to increase risk for dementia later on. Several hypotheses have been offered to explain this link, including the possibility that depression raises levels of stress hormones that injure the brain. More research is required to establish the mechanisms with greater certainty. Also, severe depression symptoms often mimic behavior changes that occur with dementia. In these cases, MCI will often disappear if depression is successfully treated.
That said, mild depressive symptoms often occur along with cognitive impairment as part of the MCI syndrome. Mild depressive symptoms may even precede MCI, and the development of late-life depression may signal an impending neurodegenerative disorder like Alzheimer's disease.

© HUIZENG HU | Getty Images
Problems with hearing increase the risk of developing dementia in later years.
Hearing loss. Hearing deficits in older adults have been linked to lower measures of cognitive skills such as executive function, memory, and processing speed as well as overall cognitive function. Research has shown that a decline in hearing in people with normal cognition increases the risk for developing Alzheimer's disease or another dementia years later. Furthermore, a 2023 study published in The Lancet found that treating hearing impairment with hearing aids reduced the chance of developing cognitive impairment in older adults at increased risk of cardiovascular disease.
Obstructive sleep apnea (OSA). With this type of sleep disorder, a person's upper airways collapse during sleep, which obstructs airflow to the lungs. The lack of oxygen causes the person to partially wake, which restores normal breathing. These episodes, called apneas, often occur repeatedly. People with this condition are at higher risk for developing MCI. Treating OSA with a continuous positive airway pressure (CPAP) machine may delay the onset of MCI.
Walking abnormalities. Walking requires the complex coordination of several functions, including movement, sensory perception, balance, and muscle strength. Because of this, many nervous system disorders will often show up in the way a person walks, and a gait test is a routine part of a neurological exam. Research has shown that a person's gait may slow down many years before an MCI diagnosis. Gait changes can also occur well before cognitive testing shows declines in other domains.
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.