Hantavirus explained: What to know after the cruise ship outbreak

Stay strong at any age with 4 basic exercises

Why testosterone levels drop and when to consider treatment

Don't count on daily aspirin to prevent colon cancer

Night owls' habits linked to worse heart health

After ablation, exercise may lower atrial fibrillation recurrence

What can cause an enlarged heart?

Women's unique risks for heart disease

Chronic kidney disease: A hidden threat to your heart

Navigating your online patient portal: Best practices
Digestive Health Archive
Articles
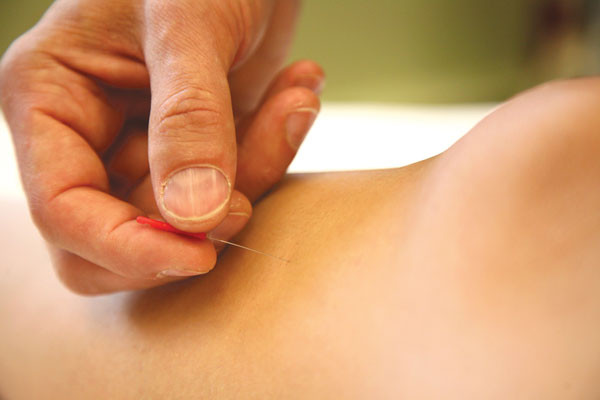
Modern acupuncture linked to constipation relief
It appears that electroacupuncture may be a treatment option for people with chronic severe functional constipation.
Is a heartburn drug hurting your health?
Long-term risks are associated with proton-pump inhibitors, but there are other options for treating acid reflux.
Image: Eranicle/ Thinkstock
Proton-pump inhibitors (PPIs), which reduce the amount of acid produced in the stomach, are so effective at treating heartburn and ulcers that they've been among the world's top-selling drugs for 25 years. Initially available only by prescription, PPIs, which include omeprazole (Prilosec), lansoprazole (Prevacid), and esomeprazole (Nexium), have been sold over the counter for several years. However, now that millions of people are taking PPIs, the drugs have been linked to an increasing number of health risks, such as fractures, kidney problems, vitamin B12 deficiency, low magnesium, and—most recently—dementia and heart attack.
"These studies—especially those suggesting a relationship to dementia and heart attack—are concerning," says Dr. Jacqueline Wolf, a gastroenterologist and associate professor of medicine at Harvard Medical School and author of A Woman's Guide to a Healthy Stomach: Taking Control of Your Digestive Health.
A warning about heartburn medications that contain aspirin
The FDA is warning that over-the-counter antacids with aspirin in them can cause stomach bleeding in rare cases.
Attack of the gallstones
They affect more women, but men still are at risk.
Image: iStock
Most people never think about gallstones—that is until they experience the severe, gut-piercing pain of a gallstone attack. "These often strike after eating, especially a high-fat or high-cholesterol meal, and can last about 30 minutes to two or more hours," says Dr. William Brugge, past director of gastrointestinal endoscopy at Harvard-affiliated Massachusetts General Hospital.
The attacks often begin in the upper-right side of the abdomen and may spread to the back, between the shoulder blades, and under the right shoulder. Nausea or vomiting may also occur.
Concern about recurring hiccups
Hiccups are often caused by many everyday situations, including distention of the stomach (which can be the result of overeating), swallowing air, or drinking carbonated beverages. They usually go away on their own, but episodes that last longer than 48 hours could be a sign of certain medical problems.
Too much of a good thing?
Proton-pump inhibitors are among the most-prescribed medications, but is long-term use safe?
Proton-pump inhibitors reduce stomach acid, which helps to treat symptoms of acid reflux.
Image: kamontad123/Thinkstock
Proton-pump inhibitors (PPIs), which are used to treat a variety of gastrointestinal problems, are among the most popular drugs in the United States. In fact, the FDA estimates about one in 14 Americans has used a PPI.
Should you keep taking that heartburn medication?
It may be time to re-evaluate if it's been a while since you started using proton-pump inhibitors.
Long-term use of some heartburn medications appears to be associated with an increated risk of dementia, heart attack, and chronic kidney disease.
Image: Thinkstock
You may think you're reaching for heartburn relief when you take a proton-pump inhibitor (PPI), a type of medication that helps block the production of stomach acid. PPIs are effective, and some—such as lansoprazole (Prevacid) and omeprazole (Prilosec)—are readily available over the counter. Others, such as pantoprazole (Protonix), are frequently prescribed for long-term use. But PPIs may have risks when taken over a long period.
8 ways to quell the fire of heartburn
Heartburn is a common problem. It's caused by the backwash of stomach acid into the esophagus, the tube connecting the mouth and stomach. This is formally called gastroesophageal reflux disease (GERD). More than just a minor discomfort, heartburn can significantly reduce quality of life. "Heartburn can cause damage to the esophagus and even increase the risk of cancer if ignored and untreated," says Dr. William Kormos, editor in chief of Harvard Men's Health Watch and a primary care physician at Massachusetts General Hospital.
These eight steps can help ease heartburn.
- Eat in a heartburn-smart way. Large meals put pressure on the muscle that normally helps keep stomach contents from backing up into the esophagus. The more you eat, the longer it takes for the stomach to empty, which contributes to reflux. Try smaller, more frequent meals — and don't wolf down your food.
- Avoid late-night eating. Having a meal or snack within three hours of lying down to sleep can worsen reflux, causing heartburn. Leave enough time for the stomach to clear out.
- Don't exercise right after meals. Give your stomach time to empty; wait a couple of hours. But don't just lie down either, which will worsen reflux.
- Sleep on an incline. Raising your torso up a bit with a wedge-shaped cushion may ease nighttime heartburn. Wedges are available from medical supply companies and some home goods stores. Don't just prop your head and shoulders up with regular pillows — doing so can actually increase pressure on the stomach by curling you up at the waist.
- Identify and avoid foods associated with heartburn. Common offenders include fatty foods, spicy foods, tomatoes, garlic, milk, coffee, tea, cola, peppermint, and chocolate. Carbonated beverages cause belching, which also causes reflux.
- Chew sugarless gum after a meal. Chewing gum promotes salivation, which helps neutralize acid, soothes the esophagus, and washes acid back down to the stomach. But avoid peppermint-flavored gum, which may trigger heartburn more than other flavors.
- Rule out medication side effects. Ask your doctor or pharmacist whether any of the medications you take might cause pain resembling heartburn or contribute to reflux.
- Lose weight if you need to. Being overweight puts more pressure on the stomach and pushes stomach contents into the esophagus. The tight-fitting clothing and belts that come with weight gain may also be a factor.
For more on relieving heartburn and treating a sensitive gut, purchase The Sensitive Gut by Harvard Medical School.

Hantavirus explained: What to know after the cruise ship outbreak

Stay strong at any age with 4 basic exercises

Why testosterone levels drop and when to consider treatment

Don't count on daily aspirin to prevent colon cancer

Night owls' habits linked to worse heart health

After ablation, exercise may lower atrial fibrillation recurrence

What can cause an enlarged heart?

Women's unique risks for heart disease

Chronic kidney disease: A hidden threat to your heart

Navigating your online patient portal: Best practices
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up