When walking makes your legs hurt
These four conditions may cause leg pain when walking.
- Reviewed by Mallika Marshall, MD, Contributing Editor
Walking is supposed to be good for you, so why do you have to suffer leg pain? And what causes the pain in your legs when walking?
Walking usually tops the moderate-intensity exercise list because it's easy, convenient, and free, and it requires minimal equipment: just a comfortable pair of shoes.
The trouble is that walking isn't easy for everyone. Walking-related leg pain is agony for many. And forget the brisk pace of three to four miles per hour advised for health and fitness.
With age - and occasionally without it - several conditions can result in leg pain during or after walking. Some may be very familiar, such as arthritis that makes knees and hips creaky; others, such as peripheral artery disease, may not be.
This article looks at four nonarthritic conditions that cause leg pain and may affect walking, as well as some ways to treat and manage them - no need to limp and bear it!
Why do my legs hurt? Leg pain causes and conditions
We discuss these conditions separately, but you may have two or more of them at the same time, which complicates diagnosis and treatment.
1. Peripheral artery disease
Peripheral artery disease (PAD) is a form of atherosclerosis, the same condition that leads to most strokes and heart attacks. Fat- and cholesterol-filled plaques narrow the arteries, and blood clots can collect on the plaques, narrowing them further. In peripheral artery disease, the arteries affected by atherosclerosis tend to be the ones that supply the leg muscles. The risk factors are like those for heart disease and stroke: smoking, high cholesterol levels, high blood pressure, and especially diabetes.
The classic symptom is lower extremity cramping, tight pain that's felt in muscles "downstream" from the narrowed artery. Pain can occur in the buttocks, thigh, calf, or foot, but occurs most often in the calf. The pain tends to come on with walking, get worse until you stop walking, and go away with rest.
Similar to angina, the pain caused by peripheral artery disease comes from working muscle cells that are starved for oxygen because of obstructed blood flow. The medical jargon for this kind of pain is intermittent claudication, from the Latin claudicatio for "limping". Many people with peripheral artery disease have other sorts of pain, too. Sometimes their legs feel heavy, or they tire easily. And it's common for people to cut back on their activity level without realizing it, which can mask the problem.
Signs of peripheral artery disease include a diminished pulse below the narrowed artery, and scratches and bruises on the lower leg that won't heal. The skin in the affected area is cool to the touch and can be pale or discolored. The diagnosis usually depends on the ankle-brachial index, which compares the blood pressure at the ankle to the blood pressure at the arm. They're normally about the same, but if there's a blockage in the leg vessels, blood pressure will be lower in the ankle because of low blood flow.
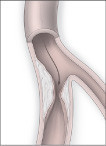
|
Arteries narrowed by atherosclerosis leave leg muscles starved for oxygen. |
Peripheral artery disease by itself can be serious and debilitating, but it may also serve as an important warning of even more serious trouble. Atherosclerosis in the legs often means there's atherosclerosis elsewhere, and people with peripheral artery disease are six to seven times more likely to have a heart attack, stroke, or transient ischemic attack (TIA) than people without it. A peripheral artery disease diagnosis should prompt a concerted effort to rein in cardiovascular disease risk factors: for example, current guidelines recommend a high-dose statin to reduce cholesterol levels.
For people who can take blood-thinning medication, a combination of rivaroxaban (Xarelto) and low-dose aspirin is recommended to reduce the risk of heart attack and stroke. Clopidogrel (Plavix), another drug that makes blood clots less likely by making platelets less sticky, is an alternative for people allergic to aspirin. The antiplatelet medication cilostazol (Pletal) may help some people walk longer distances without pain.
With PAD, walking hurts, so a "just do it" attitude about exercise isn't helpful. But researchers have found that tightly structured, supervised exercise programs can help people increase the amount they can walk before their leg pain kicks in. These programs usually involve walking until it hurts (which may be only for a few minutes), resting until the pain goes away, and then walking again. These walk-rest-walk sessions are most effective if people do them for about 30 minutes at least several days a week.
Serious cases of peripheral artery disease can cause leg pain even when the person isn't walking. This "rest pain" most often occurs in the feet. In even more serious cases, the condition can lead to tissue death and gangrene.
If peripheral artery disease is serious, or isn't improving with exercise and medication, doctors can reopen the blocked artery with angioplasty or use part of a blood vessel from elsewhere in the body to reroute circulation around the blockage. But the track record of these revascularization procedures is mixed, and some studies suggest that the results from a structured exercise program can be as good, or even better.
2. Chronic venous insufficiency
Like peripheral artery disease, chronic venous insufficiency is a condition of poor circulation, but it involves the veins and the blood's return trip back to the heart and lungs.
Our arteries are springy and help push blood along, but our veins are relatively passive participants in circulation. Particularly in the legs, the muscles surrounding the veins provide the pumping power that drains the vessels near the surface of the skin and then pushes the blood up through the deeper vessels that travel toward the heart. Tiny valves inside the veins even out the pressure and keep blood from flowing backward.
These valves are damaged in people with chronic venous insufficiency, so blood tends to pool in the legs and feet instead of traveling "north" to the heart. It's often a vicious cycle: if the valves aren't working well, pressure increases in the veins from collected blood, so the veins stretch out. As a result, the valves don't close properly, so even more blood flows backward, adding pressure. This can lead to varicose veins: bulging, swollen blood vessels in the legs and feet.
The most common symptom of chronic venous insufficiency is swollen feet and ankles. Persistent fluid accumulation in the legs can also lead to inflammation of the skin (dermatitis), skin ulcers, and an increased risk of skin infection (cellulitis). Legs may feel achy or heavy. And when people walk, they may feel an uncomfortable tightness in their legs.
|
Damaged valves in veins happens commonly with chronic venous insufficiency. |
The symptoms from chronic venous insufficiency can be helped by lying on your back and using a pillow to elevate your legs so blood flows downhill to the heart. If you're sitting for long periods, pointing your toes up and down several times can flex the vein-pumping leg muscles.
Compression stockings that squeeze harder at the ankle than at the knee can be very effective at reducing swelling and discomfort. For the stockings to work, they must be much tighter than the "antiembolism" stockings people routinely wear in the hospital. But because they are so tight, people often have a hard time getting them on. Washing a new pair can help. Some people coat their skin with talcum powder or wear thin, regular stockings underneath.
There are no specific medicines to treat venous insufficiency. Surgical procedures have improved significantly over the years. Today, physicians usually close a varicose vein permanently, rather than remove it. They use minimally invasive techniques, which are performed through catheters inserted into the veins under ultrasound guidance. These treatments are performed in outpatient settings under local anesthesia, and the patient can walk immediately after treatment.
3. Lumbar spinal stenosis
Stenosis (pronounced ste-NO-sis) is a medical term for any kind of narrowing. Spinal stenosis can occur anywhere along the spine when the vertebrae, the disks between vertebrae, or supporting structures impinge on the tubelike spinal canal that holds the spinal cord and the roots of the nerves that branch off it. Pain comes from the mechanical pressure, and perhaps also from a reduction in blood flow to nerves.
The lumbar region of the spine consists of the five large vertebrae that form the small of the back. When spinal stenosis occurs in the lumbar region, lower back pain can be a symptom - but often, the legs are affected. The pain can resemble the pain caused by peripheral artery disease: cramping tightness that increases with walking, although it's often felt in the thigh rather than the calf. The legs may also feel weak or numb.
The leg pain caused by lumbar stenosis is called neurogenic claudication.
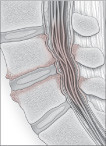
|
Vertebrae, disks, and other parts of the spine impinge on the spinal cord and nerves branching off it. |
The diagnosis starts with discussion of symptoms and medical history. One important clue is that the pain usually eases when the back is curved forward. That posture tends to take pressure off the lumbar region, and it's the reason some people with lumbar spinal stenosis find it easier to walk when leaning on a grocery cart or a walker.
An MRI or CT scan will often be ordered to confirm a diagnosis if someone has other symptoms. However, many people have spinal stenosis that shows up on imaging but doesn't cause symptoms.
Treatment usually begins with physical therapy and exercises aimed at strengthening the back and abdominal muscles. Pain relievers may help. Corticosteroid injections into the spine may provide a temporary reduction in pain, but they are not a long-term solution.
If the pain persists, surgery is an option. The most common procedure is a laminectomy, which involves cutting away part of a vertebra to create more space for the spinal cord and nerves. Bone spurs and portions of the disks and facet joints can also be removed to relieve pressure.
4. Diabetic neuropathy
People with diabetes are prone to nerve damage, or neuropathy. Exactly why is unknown. High blood sugar levels may damage the tiny blood vessels that supply nerves with oxygen and nutrients. Diabetes may also deplete the body's store of neurotrophic peptides, chemicals that normally repair and regenerate nervous tissue.
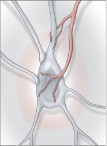
|
Blood vessels (shown in red) that supply nerve cells can be damaged by high blood sugar. |
Diabetic neuropathy affects the upper and lower legs in different ways. In the upper leg, the pain from a damaged nerve can come on suddenly and be felt in just one leg. In the lower legs and feet, where it is more common, the symptoms are typically numbness or tingling and are usually felt equally in both legs. The numbness often dulls painful sensations, so sores on the feet go unnoticed and get worse. Diabetic neuropathy can make walking difficult, but leg pain may improve with exercise.
People with diabetes can reduce their chances of developing neuropathy by keeping their blood sugar down. Once nerves have been damaged, it's less certain that tight blood sugar control is helpful. Still, blood sugar control is an important goal for many other reasons.
Medications to control burning and tingling from diabetic neuropathy include:
- tricyclic antidepressants (amitriptyline, nortriptyline, desipramine)
- serotonin and norepinephrine reuptake inhibitors (SNRIs): duloxetine (Cymbalta) is FDA-approved for diabetic neuropathy; other SNRIs also can be used.
- gabapentin or pregabalin: these are anticonvulsants but can be used if the other options are not effective.
Some people may need to take more than one type of medication at the same time. Topical pain relievers, such as capsaicin or lidocaine, also may be prescribed. Opioid pain relievers are not recommended for diabetic neuropathy.
Image: lzf/Getty Images
About the Reviewer

Mallika Marshall, MD, Contributing Editor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.