What to do if you have - or suspect you have - shingles
Don't wait to get help for shingles. Early treatment can bring quicker relief.
- Reviewed by Sharon G. Curhan, MD, ScM, Contributor
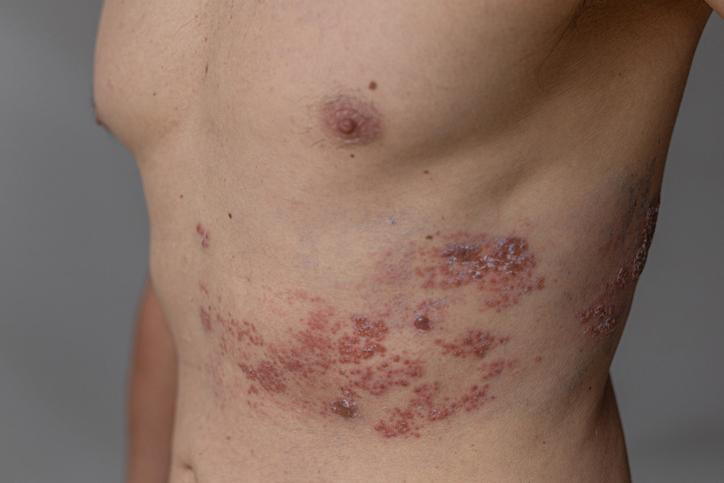
Tingling, itching, or burning in one area on one side of the body. A day or two later, a blistering rash. That telltale sequence suggests you have herpes zoster, better known as shingles.
About one in three people in the United States will suffer from shingles at some point. It can occur at any age but is most common after 50.
Who gets shingles?
Anyone who's had chickenpox (often as a child) can develop shingles. This is because the varicella-zoster virus, which causes chickenpox, doesn't go away once you've recovered from the illness; it lies dormant in the body. Later in life it can reactivate, causing shingles.
"Almost all Americans born before 1980 had chickenpox, even if they don't know or remember that they did," says Dr. Sharon Curhan, an epidemiologist at Harvard-affiliated Brigham and Women's Hospital.
Shingles can develop in otherwise healthy adults, but some people are at higher risk. These include people with certain medical conditions, such as some cancers and infections, and people who take medications that may weaken the immune system (such as chemotherapy for cancer); medications to prevent organ rejection after a transplant; and drugs used to treat autoimmune conditions (such as rheumatoid arthritis or inflammatory bowel disease). Chronic mental stress may also increase the risk for developing shingles.
What to expect when you have shingles
The tingling, itching, and burning that signal the beginning of shingles sometimes come along with a headache, a fever, or a feeling of being unwell.
Once the rash appears, it's often blistering and painful. "It may look like a band or strip," says Dr. Curhan. The rash typically affects one side and can occur anywhere on the body. It's often on the back, chest, or abdomen. It can also appear on an arm, a leg, or the face or head.
Pain in the area of the rash is common and can be severe. "It's often described as a sharp, deep burning, throbbing, or stabbing pain," says Dr. Curhan. Pain can interfere with sleep and the ability to go about daily activities.
In three to four days, the blisters, called vesicles, can become open sores. "In people with a healthy immune system, the sores crust over in seven to 10 days," says Dr. Curhan. The rash usually goes away in three to four weeks. Scarring and skin color changes can last longer.
Possible complications
Most people recover completely from shingles. But there may be complications, some of which can be severe and long-lasting.
- Post-herpetic neuralgia, which affects up to 20% of people with shingles, is shingles pain that lasts for three months or longer, even after the rash has healed.
- Allodynia is a sensitivity to stimuli that wouldn't normally be painful, such as a light touch or a temperature change. A person with allodynia may feel intense shooting pain, stinging, burning, or numbness and tingling. It usually improves over time, but some people experience it for months or even years after their episode of shingles.
- Vision or hearing damage, possibly permanent, may develop from untreated shingles near the eye or ear.
- Inflammation of the brain, called encephalitis, or of the spinal cord, called myelitis, are two possible serious consequences when shingles develops near the brain or spinal cord.
- Bacterial infections may develop in the area of the rash.
Studies have also shown that people who develop shingles are nearly 30% more likely to have a stroke or heart disease. They may be 20% more likely to experience a decline in cognitive function.
What to do if you have shingles
"If you think you might have shingles, contact a health care provider right away," says Dr. Curhan. The earlier you can get a diagnosis and treatment, the more effective the treatment is likely to be.
A clinician can usually diagnose shingles based on your symptoms and the appearance of the rash. If the diagnosis is less certain, he or she may test a sample of the fluid from the rash for the presence of the varicella-zoster virus.
Treatment typically involves an antiviral medication such as acyclovir (Zovirax), famciclovir, or valacyclovir (Valtrex). It's most effective when you start taking it within three days of the rash appearing.
Antiviral medications can shorten the duration and reduce the severity of shingles. "It's less clear whether they reduce the risk of complications," says Dr. Curhan.
Because shingles pain can be intense, you may also need pain medication. Nonprescription nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen (Tylenol) are often sufficient. Some people need prescription pain medications. If the rash becomes infected, you may need antibiotic treatment as well.
Managing shingles symptoms at home
Keep the area clean and dry. "Don't apply creams or gels to the rash unless your provider tells you to," says Dr. Curhan. Try not to scratch your skin. "Covering the rash with a lightweight, clean dressing and wearing loose-fitting clothing might help," she says.
It's also important to avoid transmitting the virus to others. "Although shingles is not contagious, a person who has never had chickenpox or gotten the vaccine can develop chickenpox after exposure to someone who has shingles," says Dr. Curhan.
The virus can be transmitted through direct contact with the rash. The virus can also become airborne and be inhaled, which is another reason to keep the rash covered. Avoid exposing people who might be at high risk for chickenpox, such as pregnant women, babies, and people with weakened immune systems.
"People usually are not infectious before the rash appears, and they're no longer infectious once the vesicles have crusted over completely," says Dr. Curhan.
Preventing shingles
The best way to prevent shingles and its complications is to get the shingles vaccine (Shingrix). Even if you've already had shingles, you should still get the vaccine, because it can reduce the risk you'll develop shingles again.
The shingles vaccine is safe and highly effective. It's recommended for adults ages 50 and over, and anyone 18 and over has a weakened immune system.
Image: © Leonardo Moreno/Getty Images
About the Author

Lynne Christensen, Staff Writer
About the Reviewer

Sharon G. Curhan, MD, ScM, Contributor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.













