Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Scoliosis treatment: Can it help as you get older?

Physical therapy provides modest improvement for chronic low back pain
Prostate Cancer Archive
Articles
Who needs hormone therapy for prostate cancer?
Level of health literacy affects treatment choice for slow-growing prostate cancer
A genetic test that provides an assessment of how aggressive a man's prostate cancer is and how likely it is to spread within his body. A new study has investigated for the first time how results of this test are impacting treatment decisions — with surprising results.
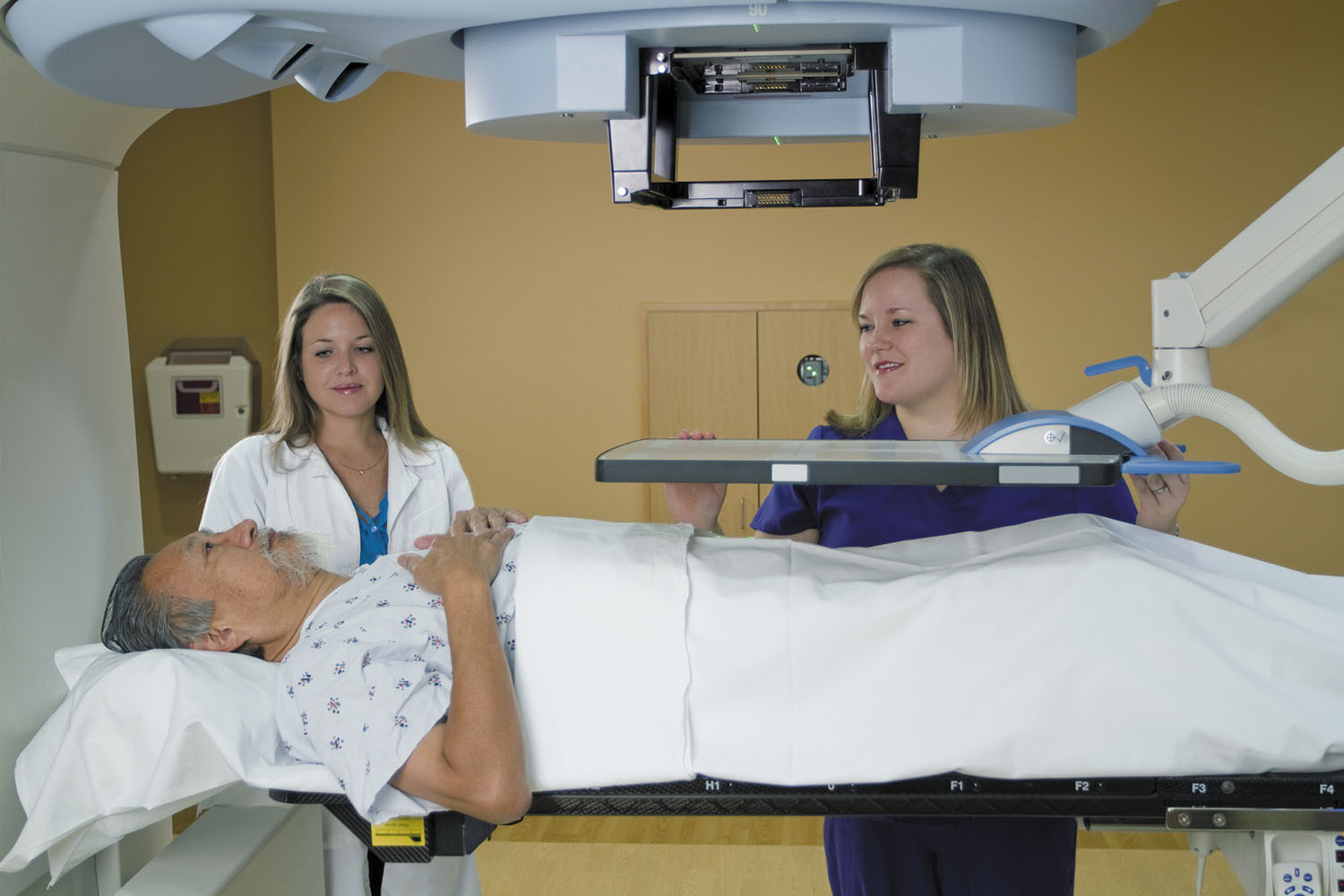
A new treatment for advanced prostate cancer improves survival in phase 3 clinical trial
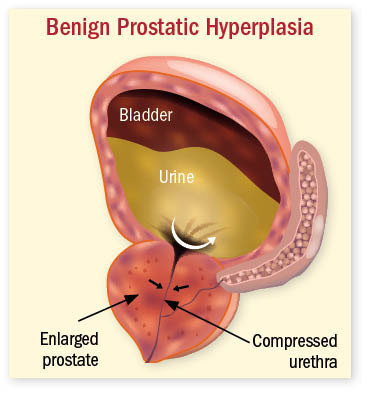
Steps to treating an enlarged prostate
Large review study finds low risk of erectile dysfunction after prostate biopsy
MRI looking better for detecting prostate cancer
American Heart Association issues statement on cardiovascular side effects from hormonal therapy for prostate cancer
New ways to test for prostate cancer
Recent advances can help men with a worrisome PSA result avoid immediate biopsy.
Prostate-specific antigen (PSA) blood testing receives high marks as an effective way to monitor disease activity in men diagnosed with prostate cancer. Yet, as a screening tool for prostate cancer, PSA testing is problematic.
PSA naturally tends to increase as men get older, but levels that get too high may suggest prostate cancer. A PSA level of less than 4 nanograms per milliliter (ng/mL) is often reassuring, unless there has been a sudden jump from a much lower number. Many doctors consider a total PSA level higher than 10 ng/mL as the threshold for getting a biopsy to check for cancer.
Predicting low-risk prostate cancer
New calculators can estimate the chance your cancer might — or might not — become more aggressive.
Active surveillance is a popular option for men with low-risk prostate cancer, defined as a tumor that is confined to the prostate gland and unlikely to grow or spread. It involves monitoring prostate-specific antigen (PSA) levels in the blood for changes and having regular digital rectal exams to look for abnormal areas on your prostate.
During active surveillance, you have a PSA test and a digital rectal exam every six months and prostate biopsies approximately every other year. If your PSA level rises, your doctor will likely recommend a prostate MRI or an immediate prostate biopsy to see if the cancer has become more aggressive. If so, you and your doctor can decide whether to continue with active surveillance and have another biopsy six months or a year later, or move ahead to treatment, such as radiation, hormonal therapy, or surgery.

Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Scoliosis treatment: Can it help as you get older?

Physical therapy provides modest improvement for chronic low back pain
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up