That nagging cough
- Reviewed by Mallika Marshall, MD, Contributing Editor
What's that nagging cough, and what can you do to cure it? Cough for a minute or two, and you may think something has "gone down the wrong pipe." Cough for a day or two, and you may think you've picked up a cold or the flu. After a week, bronchitis or allergies may come to mind. But after three or four weeks, your mind starts to race, and the worry begins to mount.
For many people, chronic coughing raises the specter of cancer. But is cancer really a common cause of a cough that lingers? If not, what is? And what can you do to quiet a nagging cough?
What is a cough?
Cough is a vital player in the body's defense against disease. Coughing expels mucus, microbes, and foreign particles from the respiratory tract, protecting the lungs from infection and inflammation.
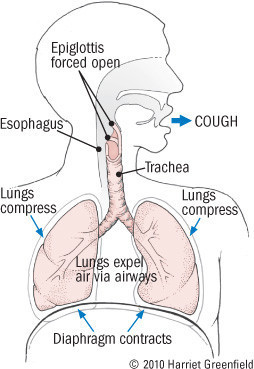
Cough begins with an initial gasp that draws air deep into the lungs. Next, the glottis snaps shut, blocking the trachea, or windpipe. The third step is the forceful contraction of the muscles of the chest cage, abdomen, and diaphragm (see figure). In normal breathing, these muscles push air gently from the lungs up through the nose and mouth. When the glottis is closed, the air can't move out, so tremendous pressure builds up in the air passages. Finally, the glottis is forced open and the air rushes out. And it is quite a rush; with a vigorous cough, air travels out at nearly the speed of sound.
Anatomy of a cough
|
A cough can be a conscious, voluntary act or an uncontrollable, involuntary reflex. In the latter case, stimulation of nerves in the larynx ("voice box") and respiratory tract initiates the process. These nerves can be irritated by infections, allergies, cold air, tumors, chemicals such as smoke, particles or foreign bodies, and normal body fluids such as nasal mucus or stomach acid. It's no wonder, then, that so many different things can trigger a cough.
The chronic cough
Everyone coughs, and nobody worries about an occasional cough. Many acute illnesses and allergies - ranging from hay fever and the common cold to bronchitis and pneumonia - produce recurrent coughs. But the cough that accompanies acute illnesses resolves in a few days or weeks. In contrast, a chronic cough lingers for more than three to eight weeks, sometimes lasting for months or even years.
Chronic coughing is one of the most common reasons for seeing a doctor. In addition to worry about the cause of the cough, patients experience frustration and anxiety, especially if diagnosis and treatment stretch out over weeks. Coughing interrupts sleep, causing fatigue, poor concentration, and impaired work performance. Coughing also can have physical consequences ranging from urinary incontinence to fainting and, more rarely, broken ribs. Considering medical tests, lost productivity at work, remedies that don't help, and treatments that do, coughing can become expensive.
Persistent cough: Major causesCommon causes of a nagging cough
Less common causes of a nagging cough
Common in smokers
|
What causes chronic coughing?
Smoking is a leading cause of chronic coughing. Sooner or later, most cigarette smokers develop a chronic "smoker's cough." Chemical irritation is responsible - but the same noxious chemicals that cause a smoker's cough can lead to far more serious conditions such as bronchitis, emphysema, pneumonia, and lung cancer. A chronic cough is always a cause of concern for smokers.
A lingering cough also is a worry for nonsmokers. Dozens of conditions can cause a recurrent cough, but the lion's share of coughs are caused by just five: postnasal drip, asthma, gastroesophageal reflux disease, chronic bronchitis, and treatment with angiotensin-converting enzyme (ACE) inhibitors used for high blood pressure and heart failure. Many people have several of these conditions, but in nonsmokers, the first three, singly or in combination, account for nearly all chronic coughs. The major causes of long-term coughing are listed below.
In nonsmokers, more than nine of every 10 lingering coughs are caused by one of these five conditions:
1. Postnasal drip (also called the upper airway cough syndrome)
This is the leading cause of a lingering cough.
The human nose is more than the organ of smell: It is also the gateway to the lower respiratory tract. As such, its job is to condition the air passing through to the lungs. The nose warms air that is cool, adds moisture to air that is dry, and removes particles from air that is dirty. The nasal membranes accomplish all three tasks by producing mucus that is warm, moist, and sticky.
Although the nose is a guardian of the more delicate lungs, it is subject to problems of its own. Viruses, allergies, sinusitis, dust particles, and airborne chemicals can all irritate the nasal membranes. The membranes respond to injury by producing mucus that is thin and runny.
All that mucus must go somewhere. When it drips out of the nose, it's a nuisance. But when it drips down the throat, it tickles the nerves of the nasopharynx, triggering a cough. In some cases, the nose itself is to blame (rhinitis), but in others, a prolonged postnasal drip lingers after a viral upper respiratory infection; some call this variety a post-infectious cough.
In typical cases, people with postnasal drip cough more at night, and they are often aware of a tickling feeling at the back of their throats. But they also may cough during the day, and their throats may be irritated and sore, or perfectly fine.
The best way to find out if a chronic cough is the result of postnasal drip is to try treatment. Nonprescription decongestant or antihistamine tablets are a first step. Most contain a decongestant, an antihistamine, or a combination of the two. In one form or another, these medications are generally effective and safe, but some people complain of a racing heart and jitteriness (due to the decongestant), while others feel sleepy (due to the antihistamine). Men with benign prostatic hyperplasia (BPH) may have difficulty passing urine while they're taking decongestants, and antihistamines occasionally can trigger acute glaucoma. As with all medications, read the directions carefully.
Home remedies can help as well. Inhaling steam from a hot shower or kettle is the simplest. Nasal irrigation may clean out irritating secretions. You can purchase saline nose sprays at your drugstore, or you can do it yourself using a homemade solution (1/8 teaspoon of table salt per 1 cup of water) and a neti pot, squeeze bottle, or bulb syringe. If saline irrigations seem to help, repeat them one to three times per day.
2. Asthma
Asthma results from bronchospasm, a temporary, reversible narrowing of the medium-size tubes that carry air into the lungs. In most cases, that air makes a whistling or wheezing sound as it moves through narrowed passages. Excessive mucus production, shortness of breath, and cough are the other classic symptoms of asthma. Some people have cough-variant asthma, in which coughing is the only symptom.
In most cases, cough-variant asthma produces a persistent, dry cough that occurs around the clock but may begin at night. Exposure to allergens, dust, or cold air often triggers coughing, as does exercise.
If your medical team suspects that asthma is responsible for a chronic cough, they can order pulmonary function tests to confirm the diagnosis. If the tests are inconclusive, you may be asked to inhale small doses of methacholine, a drug that often triggers wheezing in people with asthma.
Cough-variant asthma also is likely to respond to treatment. Care providers often suggest a short-acting bronchodilator spray such as albuterol (Proventil, Ventolin). For longer-term relief, your provider may prescribe an inhaled corticosteroid such as fluticasone (Flovent), triamcinolone (Azmacort), or budesonide (Pulmicort).
If you have a chronic cough that may be due to asthma, ask your provider to consider testing or treatment. But if asthma is not the answer, consider another leading cause of the cough that lingers.
3. Gastroesophageal reflux disease (GERD)
Just as people are surprised to learn that asthma can cause coughing without wheezing, many people are shocked to learn that GERD can cause coughing without heartburn.
GERD occurs when stomach contents travel backward, making their way up into the esophagus instead of down into the intestines. Heartburn is the typical symptom; other common symptoms include belching, a sour taste in the mouth, and bad breath. But acid also irritates nerves in the esophagus, and these nerves can trigger the cough reflex even without the distress signal of pain. In fact, up to one-third of patients with GERD are pain-free, and they might only complain of cough, a hoarse voice from recurrent laryngitis, or unexplained sore throats.
GERD can be tricky to diagnose when there's no pain. Esophageal pH monitoring, in which the patient swallows a probe that remains in the lower esophagus for 24 hours, can detect the presence of acid from reflux. It's not as uncomfortable as it sounds, but it is expensive and inconvenient.
As with the other causes of chronic cough, a simpler approach to diagnosis is to try treatment. You can begin on your own. Avoid alcohol and foods that often trigger GERD, including those that contain chocolate, peppermint, caffeine, garlic, onions, citrus fruits, tomato sauce, or lots of fat. Eat small meals and never lie down until two hours after you've eaten. Take over-the-counter antacids, particularly at bedtime, and consider elevating the head of your bed or sleeping on a wedge-shaped pillow to keep your stomach's contents flowing down at night.
If you're constantly coughing after a week or so, you can add an over-the-counter acid suppressor. Today there are many to choose from, such as cimetidine (Tagamet), famotidine (Pepcid), omeprazole (Prilosec), omeprazole plus sodium bicarbonate (Zegerid), and lansoprazole (Prevacid). Less expensive generic versions work just as well. Stronger acid blockers are available by prescription.
It may take three or four weeks of gradually escalating therapy to control GERD. If you continue coughing, there's likely another cause.
4. Chronic bronchitis and bronchiectasis
Chronic bronchitis is persistent inflammation of the bronchial tubes causing airway narrowing and production of excess mucus. It usually happens from tobacco use or long-term exposure to high levels of industrial air pollutants. Bronchiectasis is also a result of chronic inflammation that damages the walls of the bronchial tubes. In either variant, the inflammation leads to a chronic cough. The most effective treatment is to quit smoking and avoid air pollutants. In addition, your doctor can prescribe a corticosteroid inhaler, usually with a long-acting bronchodilator. People with chronic bronchitis are prone to flare-ups. Doctors call them chronic obstructive pulmonary disease (COPD) exacerbations. The main symptoms are increased coughing, thick dark mucus production, shortness of breath, and fatigue. The treatment includes antibiotics and an oral corticosteroid, usually prednisone.
5. Therapy with angiotensin-converting–enzyme (ACE) inhibitors
ACE inhibitors - such as enalapril (Vasotec, generic), lisinopril (Prinivil, Zestril, generic), and benazepril (Lotensin, generic), as well as many others - have assumed a prominent role in the treatment of high blood pressure and heart failure.
ACE inhibitors are favored by many doctors because they produce good results and have few side effects, with one exception - a persistent cough. It occurs in up to 10% of people taking an ACE inhibitor. The first symptom is often just a throat tickle, followed by a dry cough that can begin as soon as three weeks or as late as one year after the medication is started.
If the cough is mild, people may choose to continue their medication, or they may cough less if they change to a different ACE inhibitor. But the only way to eliminate a severe cough induced by an ACE inhibitor is to switch to another type of antihypertensive medication. Fortunately, many are available, including angiotensin-receptor blockers (ARBs) like losartan (Cozaar, generic) and valsartan (Diovan, generic) - drugs that have been shown to be just as effective as ACE inhibitors without causing a cough.
When to worry about a constant coughAlthough a chronic cough is usually not serious, warning symptoms call for prompt medical care. The symptoms include:
|
Finding chronic cough causes and treatments
Don't ignore a chronic cough - but don't panic just because your cough lingers for more than three or four weeks. Most often, the puzzle can be solved without elaborate tests, and the problem can be corrected with simple treatments. But if your cough is accompanied by mucus production, bloody mucus, fever, weight loss, night sweats, breathlessness, undue fatigue, or chest pain, consult your doctor without delay.
Cough medicineAt the drugstore, you'll find a bewildering array of syrups, sprays, tablets, and lozenges designed to control coughing. You'll also see a steady stream of customers coughing up lots of money to purchase products that may be ineffective. Many cough remedies contain expectorants, compounds intended to thin and loosen mucus in the airways, making it easier to clear. Guaifenesin is the most popular expectorant, and the only one found in over-the-counter products. Unfortunately, there is little scientific evidence that expectorants are effective. You'll probably do just as well by using a humidifier and drinking lots of water. Cough suppressants are also very popular. Nonprescription agents such as dextromethorphan can partially suppress the cough reflex, helping make you more comfortable. However, prescription-only cough syrups with codeine tend to be more effective. When used appropriately, cough suppressants can reduce discomfort; remember, though, that because coughing can serve a useful function, it should not always be suppressed. Medicated lozenges and cough drops are among the most widely sold cough remedies. These products contain various combinations of menthol, camphor, eucalyptus oil, honey, and other ingredients. Some also contain topical anesthetics. Despite their popularity, there is no evidence that medicated cough drops are more effective than simple hard candies. |
Image: © Sebarnes/Getty Images
About the Reviewer

Mallika Marshall, MD, Contributing Editor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.