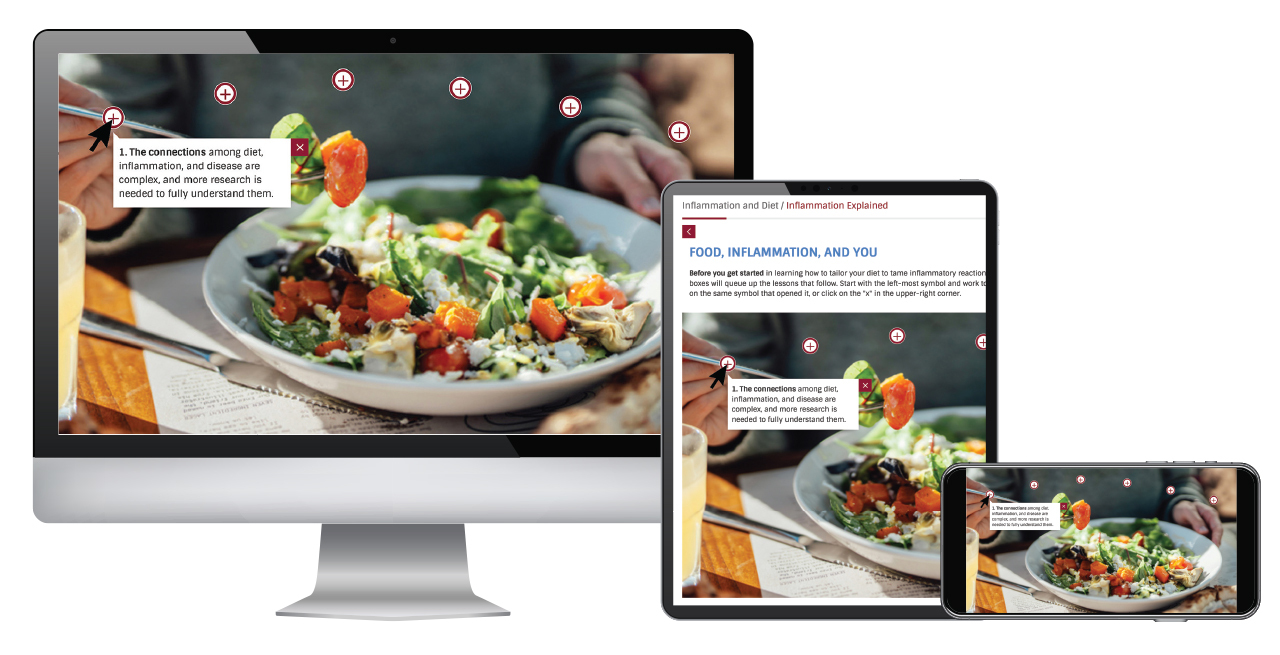
Understanding food noise - and how to turn down the volume

Remedies for motion sickness: What works?

4 keys to a heart-healthy diet

Understanding exercise heart rate zones

Resistant starch: Can you make the carbs you eat a little healthier?

Harvard study: A couple of daily cups of coffee or tea linked to lower dementia risk

Does everyone benefit from cutting saturated fat in their diet?

How to treat shoulder impingement

Beyond protein: 6 other nutrients that help prevent muscle loss
Advancements in knee replacement: More precise and personalized
Heart Attack Archive
Articles

Understanding food noise - and how to turn down the volume

Remedies for motion sickness: What works?

4 keys to a heart-healthy diet

Understanding exercise heart rate zones

Resistant starch: Can you make the carbs you eat a little healthier?

Harvard study: A couple of daily cups of coffee or tea linked to lower dementia risk

Does everyone benefit from cutting saturated fat in their diet?

How to treat shoulder impingement

Beyond protein: 6 other nutrients that help prevent muscle loss

Advancements in knee replacement: More precise and personalized
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up