Why testosterone levels drop and when to consider treatment

Don't count on daily aspirin to prevent colon cancer

Night owls' habits linked to worse heart health

After ablation, exercise may lower atrial fibrillation recurrence

What can cause an enlarged heart?

Women's unique risks for heart disease

Chronic kidney disease: A hidden threat to your heart

Navigating your online patient portal: Best practices

Treating hair loss in men: What works?

Virtual cardiac rehab: Heal your heart from home
Heart Attack Archive
Articles
Heartburn medications and the heart
| Image: ThinkStock |
Ask the doctor
Q. I've read news reports that the heartburn drug I take may cause heart attacks. Should I worry about this?
A. Several studies have reported an association between proton-pump inhibitors (PPIs) and heart attacks. PPIs are medications for heartburn, such as omeprazole (Prilosec) and pantoprazole (Protonix). Overall, however, the evidence suggests these medications are not risky for your heart.
New recommendation narrows heart benefit from low-dose aspirin
Image: Bigstock
In the journals
The influential U.S. Preventive Services Task Force (USPSTF) has endorsed low-dose daily aspirin to prevent cardiovascular disease in people ages 50 to 59 who have a 10% or greater chance of heart attack or stroke in the next 10 years. Unless a person already has cardiovascular disease, the actual number of heart attacks and strokes prevented with daily aspirin is relatively small. This draft recommendation did not recommend aspirin for those younger than 50 or 60 or older, citing insufficient evidence to make a recommendation.
The USPSTF statement is at odds with a statement in 2014 by the FDA that evidence does not support general use of aspirin to prevent a first heart attack or stroke in otherwise healthy adults. However, daily aspirin is often recommended for those with a history of cardiovascular disease, since the potential benefit (preventing heart attacks and strokes) outweighs the risk of bleeding that comes with regular aspirin use.
Cardiac rehab is often the best medication for recovery
One advantage of attending cardiac rehab is the power of the group support, which can provide added motivation. |
Participation in a cardiac rehabilitation program following a heart attack helps people live longer and better.
Research we're watching: A better way to predict fatal heart events
In emergency departments, doctors routinely test blood levels of a protein called troponin to diagnose people with suspected heart attacks. That's because damaged heart muscle releases troponin into the bloodstream. Now, new research suggests that a high-sensitivity troponin test may help identify people with heart disease who face a high risk of fatal heart events.
For the study, published in the August 13 issue of The New England Journal of Medicine, researchers measured troponin levels with the high-sensitivity test in nearly 2,300 people with type 2 diabetes and stable heart disease (meaning they had narrowed heart arteries and chest pain but not a heart attack). Within five years, nearly one in three people with elevated troponin levels had a heart-related problem or died from one.
Low-dose aspirin for people with heart disease
If you have heart disease, national guidelines recommend that you take a low-dose (81-mg) aspirin every day. It's an inexpensive and effective way to lower your risk of a heart attack or stroke. According to a report in the July 17 Morbidity and Mortality Weekly Report, about seven in 10 adults with heart disease follow this advice.
The study relied on telephone surveys done by the CDC about health behaviors. It included data from more than 17,900 adults from 20 states and the District of Columbia.
Ask the doctor: Clot prevention drugs after a stent: How long?
Guidelines about how long to take clopidogrel after receiving a stent are in flux. Image: Thinkstock |
Q. My cardiologist told me to take clopidogrel for a year after I received a stent. Now the year is up. I haven't had any bleeding problems. Should I keep taking it?
A. In addition to aspirin, doctors routinely prescribe clopidogrel (Plavix) for people who receive stents, the tiny metal mesh tubes placed in clogged blood vessels to improve blood flow. This medication stops blood components called platelets from clumping together and forming clots. The current guidelines generally recommend that people take the drug for a year. This advice assumes they don't have any side effects such as unusual bleeding, which can show up as severe nosebleeds or blood in the urine or stools. However, these guidelines are still evolving. Experts are currently reviewing new findings from large studies on the benefits and risks of taking clopidogrel and similar drugs for extended periods of time.
Don't worry about sudden cardiac arrest during exercise
Getting regular exercise is the best way to prevent most types of heart disease—including sudden cardiac arrest. Images: Thinkstock |
New findings may help allay fears about sports-related heart death.
Too darn hot for your heart?
Dress for summer's heat, and don't stay outside too long. Image: Thinkstock |
Summer's heat, humidity, and smog may be tough for people at risk of heart disease.
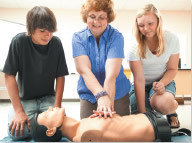
Bystander CPR may help cardiac arrest survivors return to work
Cardiopulmonary resuscitation (CPR) not only saves lives, it may also help survivors of cardiac arrest recover well enough to return to work, according to a study in the May 12, 2015, issue of Circulation.
Researchers studied more than 4,300 people in Denmark who were employed before they suffered a cardiac arrest. In cardiac arrest, the heart suddenly stops working. More than 75% of survivors who had a cardiac arrest outside a hospital were able to return to work in a median time of four months. Those who received CPR from a bystander were nearly 40% more likely go back to work compared with those who didn't get CPR. The chest compressions given during CPR keep blood circulating to the brain, minimizing brain damage caused by a lack of oxygen.
When the blood supply to the kidneys suffers
The renal arteries, which supply blood to the kidneys, can become narrowed or blocked—a condition known as renal artery stenosis. Image: Thinkstock |
Fatty plaque in the arteries that feed the kidneys poses a danger to the heart and brain.

Why testosterone levels drop and when to consider treatment

Don't count on daily aspirin to prevent colon cancer

Night owls' habits linked to worse heart health

After ablation, exercise may lower atrial fibrillation recurrence

What can cause an enlarged heart?

Women's unique risks for heart disease

Chronic kidney disease: A hidden threat to your heart

Navigating your online patient portal: Best practices

Treating hair loss in men: What works?

Virtual cardiac rehab: Heal your heart from home
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up