Vitamin D and your health: Breaking old rules, raising new hopes

Vitamin D was discovered in 1920, culminating the long search for a way to cure rickets, a painful childhood bone disease. Within a decade, the fortification of foods with vitamin D was under way, and rickets became rare in the United States. But solving the problem of rickets was only the beginning of research into vitamin D. Research results suggest that vitamin D may have a role in other aspects of human health.
Breaking the old rules
Vitamin D is one of the 13 vitamins discovered in the early 20th century by doctors studying nutritional deficiency diseases. Ever since, scientists have defined vitamins as organic (carbon-containing) chemicals that must be obtained from dietary sources because they are not produced by the body's tissues. Vitamins play a crucial role in our body's metabolism, but only tiny amounts are needed to fill that role.
Although vitamin D is firmly enshrined as one of the four fat-soluble vitamins, it is not technically a vitamin. True, it's essential for health, and only minuscule amounts are required. But it breaks the other rules for vitamins because it's produced in the human body, it's absent from all natural foods except fish and egg yolks, and even when it's obtained from foods, it must be transformed by the body before it can do any good.
As our habits change, most of us cannot rely on our bodies to produce vitamin D the old-fashioned way. Instead, we increasingly depend on artificially fortified foods and pills to provide this vital nutrient. Coming full circle in the modern world, this substance may actually come to fit the technical definition of a vitamin.
What is vitamin D?
Vitamin D is not one chemical but many. The natural type is produced in the skin from a universally present form of cholesterol, 7-dehydrocholesterol. Sunlight is the key: Its ultraviolet B (UVB) energy converts the precursor to vitamin D3. In contrast, most dietary supplements are manufactured by exposing a plant sterol to ultraviolet energy, thus producing vitamin D2. Because their function is almost identical, D2 and D3 are lumped together under the name vitamin D — but neither will function until the body works its magic (see figure).
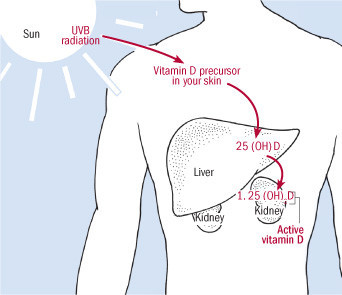
How your body makes vitamin D
The sun's energy turns a chemical in your skin into vitamin D3, which is carried to your liver and then your kidneys to transform it to active vitamin D. |
The first stop is in the liver, where vitamin D picks up extra oxygen and hydrogen molecules to become 25-hydroxyvitamin D, or 25(OH)D. This is the chemical that doctors usually measure to diagnose vitamin D deficiencies. But although 25(OH)D is used for diagnosis, it can't function until it travels to the kidney. There it acquires a final pair of oxygen and hydrogen molecules to become 1,25 dihydroxy vitamin D; scientists know this active form of the vitamin as 1,25(OH)2D, or calcitriol, but for ordinary folks the name vitamin D is accurate enough.
How it works
Vitamin D's best-known role is to keep bones healthy by increasing the intestinal absorption of calcium. Without enough vitamin D, the body can only absorb 10% to 15% of dietary calcium, but 30% to 40% absorption is the rule when vitamin reserves are normal. A lack of vitamin D in children causes rickets; in adults, it causes osteomalacia. Both bone diseases are now rare in the United States, but another is on the rise — osteoporosis, the "thin bone" disease that leads to fractures and spinal deformities.
Low levels of vitamin D lead to low bone calcium stores, increasing the risk of fractures. If vitamin D did nothing more than protect bones, it would still be essential. But researchers have begun to accumulate evidence that it may do much more. In fact, many of the body's tissues contain vitamin D receptors, proteins that bind to vitamin D. In the intestines, the receptors capture vitamin D, enabling efficient calcium absorption. But similar receptors are also present in many other organs, from the prostate to the heart, blood vessels, muscles, and endocrine glands. And work in progress suggests that good things happen when vitamin D binds to these receptors. The main requirement is to have enough vitamin D, but many Americans don't.
Vitamin D deficiencies
Vitamin D deficiencies were rare when most men rolled up their sleeves to work in sunny fields. But as work shifted from farms to offices, that changed. Because pigmentation can reduce vitamin D production in the skin by over 90%, nonwhite populations are at particular risk. Deficiencies are also common in patients with intestinal disorders that limit absorption of fat and those with kidney or liver diseases that reduce the conversion of vitamin D to its active form, calcitriol (1,25(OH)2D). In addition, certain medications reduce the availability or activity of vitamin D. And even in healthy people, advancing age is linked to an increased risk of vitamin D deficiency.
Although standards vary, most experts agree that levels of 25(OH)D below 20 ng/ml (nanograms per milliliter) reflect clear-cut vitamin D inadequacy, while levels between 20 and 30 ng/ml are borderline.
A number of factors can play a role. Limited exposure to sunlight heads the list. Except during the short summer months, people who live at latitudes above 37 degrees north or below 37 degrees south of the equator don't get enough UVB energy from the sun to make all the vitamin D they need. The same is true for people who spend most of their time indoors and for those of us who avoid sunshine and use sunscreens to protect our skin from the harmful effects of ultraviolet radiation (see box below). It's an example of an unforeseen consequence of wise behavior, but you can enjoy sun protection and strong bones, too, by taking vitamin supplements.
SunscreensLike politicians, doctors often have to compromise; when it comes to sunshine, most pols promise blue skies, while most docs turn out to be the shady guys — or, at least, sunscreen advocates. Sunlight contains two forms of radiant energy, ultraviolet A (UVA) and ultraviolet B (UVB). UVB provides the energy your skin needs to make vitamin D, but that energy can burn the skin and increase the cell damage that leads to cancer. UVA also contributes to skin damage and premature aging. To protect yourself, avoid the summer sunshine, especially between 10 a.m. and 2 p.m. Whenever possible, wear a large-brimmed hat and a tightly woven, dark-colored long-sleeve shirt and long pants when you go out in the sun. But summer garb is usually lightweight and exposes a lot of skin. That's where a sunscreen comes in. Look for a product with an SPF of 30 or higher. Look for a "broad spectrum" sunscreen that also protects against both UVA and UVB. Apply your sunscreen early, often, and liberally. |
These many factors explain why vitamin D deficiencies are shockingly common in the United States. Although standards vary, most experts agree that levels of 25(OH)D below 20 ng/ml (nanograms per milliliter) reflect clear-cut vitamin D inadequacy, while levels between 20 and 30 ng/ml are borderline. Using similar criteria, American researchers have reported deficiencies in 42% of African American women aged 15 to 49, in 41% of non-hospitalized patients aged 49 to 83, and in up to 57% of hospitalized patients. And low levels of vitamin D are common even in apparently healthy young adults; in one study, more than a third of people between the ages of 18 and 29 were deficient.
Numbers can never tell the whole story, but in this case, "D-ficiencies" add up to a wide range of health concerns.
Osteoporosis and fractures
It's a paradox: Skeletal health is the best-known contribution of vitamin D, but it has also become the most controversial. Although doctors agree that vitamin D deficiency increases the risk of osteoporosis and fractures, they disagree about the benefits and optimal dosage of supplements.
Without enough vitamin D, the intestines cannot efficiently absorb calcium. But because blood calcium is critical for neuromuscular and cardiac function, the body does not allow levels to fall. Instead, it pours out parathyroid hormone, which mobilizes calcium from bone. Blood calcium levels remain normal, so your heart and nerves keep working nicely. But your bones bear the brunt: As bone calcium density falls, bones become weak and fracture-prone.
Most studies show that a lack of vitamin D increases the risk of osteoporosis and the likelihood of hip and other non-spinal fractures. But there is considerable disagreement about how much supplements reduce the risk of fractures. Some studies include only women, others both men and women; some include only frail, elderly, or institutionalized subjects, others physically active people; some use vitamin D alone, others a combination of D and varying doses of calcium; and some administer 400 international units (IU) of vitamin D a day, others up to 800 IU a day.
Prostate cancer
Some men mistakenly dismiss osteoporosis as a women's worry, but none fail to recognize the importance of prostate cancer.
Vitamin D has an important role in regulating cell growth. Laboratory experiments suggest that it helps prevent the unrestrained cell multiplication that characterizes cancer by reducing cell division, restricting tumor blood supply (angiogenesis), increasing the death of cancer cells (apoptosis), and limiting the spread of cancer cells (metastasis). Like many human tissues, the prostate has an abundant supply of vitamin D receptors. And, like some other tissues, it also contains enzymes that convert biologically inactive 25(OH)D into the active form of the vitamin, 1,25(OH)2D. These enzymes are much more active in normal prostate cells than in prostate cancer cells.
Do the results from these experiments translate into clinically important effects? Possibly.
In 1998, Harvard's Health Professionals Follow-up Study of 47,781 men reported that a high consumption of calcium supplements was associated with an increased risk of advanced prostate cancer. The risk was greatest in men getting more than 2,000 mg of calcium a day from a combination of supplements and food. Since then, other studies have confirmed a link between very high levels of calcium intake and increased risk, but they have exonerated dietary calcium consumption. The Harvard scientists speculate that the problem is not calcium itself but a relative lack of active vitamin D.
Other malignancies
The risk of colon cancer, breast cancer, and other malignancies appears to rise in populations at latitudes far from the equator. Sun exposure and vitamin D levels may be part of the explanation. A recent clinical trial looking at a daily 1,000 IU vitamin D supplement did not show a decreased risk of cancer, but it was associated with a decreased risk of cancer death.
"D" right amount
The most widely used recommended dietary allowance (RDA) for vitamin D is 600 IU daily for adults up to age 69 and 800 IU daily for people older than 70.
Is more better? We don’t know yet, but you definitely can get too much of a good thing. Like the other fat-soluble vitamins, vitamin D is stored in the body's adipose (fat) tissue. That means your body can mobilize its own reserves if your daily intake falters temporarily — but it also means that excessive doses of vitamin D can build up to toxic levels. At those extremes, vitamin D can raise blood calcium to levels that can cause grogginess, constipation, and even death. But it takes massive overdosing to produce toxicity.
How to get vitamin D
You can make your vitamin D the old-fashioned way, by exposing your skin to UVB radiation in sunlight. It doesn't take much, but people living north of the 37-degree-latitude line — roughly the imaginary line between Philadelphia and San Francisco — can't get enough UVB in winter to do the trick. And many others will find it all too easy to overdose on UVB, increasing their risk of malignant melanomas and other skin cancers, as well as wrinkles and premature skin aging. All in all, most doctors recommend avoiding sunlight (see box) and getting vitamin D by mouth.
Diet can help, but it's very hard to approach the new goals with food alone. Fish and shellfish provide natural vitamin D (oily fish are best), but you'll have to eat about 5 ounces of salmon, 7 ounces of halibut, 30 ounces of cod, or nearly two 8-ounce cans of tuna to get just 400 IU. An egg yolk will provide about 20 IU, but since it also contains nearly a day's quota of cholesterol, you can't very well use eggs to fill your tank with D. Other foods have even less D, which is why manufacturers fortify milk, some yogurt, some orange juice, and many cereals with vitamin D. In general, a serving will provide about 100 IU; that means drinking a quart of fortified milk to get 400 IU.
Most people require supplements to get the vitamin D they need. It's the main benefit of a daily multivitamin; most provide 400 IU. Remember to read the labels carefully so you won't get too little or too much. And although cod liver oil is rich in vitamin D, it has too much vitamin A for regular use.
New light on the sunshine vitamin
It used to be simple: just get a "healthy" tan and your body will make all the vitamin D it needs. Desk jobs and sunscreen have changed all that, just as research is underlining the importance of vitamin D and suggesting its possible role in preventing many health problems. That makes vitamin D a dilemma of modern life that has a modern solution: eating fish and drinking some low-fat fortified milk, along with judicious doses of vitamin D supplements.
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.