How to determine— and achieve—your target blood pressure
Take an active role by checking your blood pressure with a home monitor.
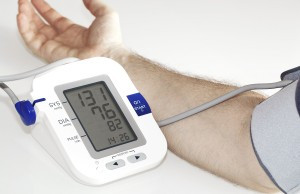
Most appointments with a health care provider begin with a gentle squeeze—the sensation of a blood pressure cuff inflating around your upper arm. But that single blood pressure reading offers only a glimpse of the health of your cardiovascular system.
"When you have your blood pressure checked in the doctor's office, you're in an artificial environment that is not reflective of the vast majority of the time when your blood pressure is going through its daily excursions," says cardiologist Dr. Elliott Antman, professor of medicine at Harvard Medical School. Throughout the course of a day, the average person's systolic b-lood pressure (the first number in the reading) may fluctuate considerably.
In medical settings, some people get very anxious, which can cause their blood pressure to rise—a phenomenon known as white-coat hypertension. Others may feel like they're in a protected, safe place where they can sit back and relax, which may cause their blood pressure to be lower. If their blood pressure is high at other times, however, they may have a condition called masked hypertension.
The diagnosis challenge
The U.S. Preventive Services Task Force, a group that draws up medical guidelines, recommends that people measure their blood pressure outside of the medical setting to confirm a diagnosis of high blood pressure before starting treatment. In November 2015, the group endorsed ambulatory blood pressure monitoring as the best method. For 24 hours, you wear a small portable machine on a belt or a pouch connected to a blood pressure cuff on your arm. The device records your blood pressure every 15 to 30 minutes. You go about your daily routine and use a diary to jot down when you sleep, wake, eat, exercise, and take medications, and if you experience any periods of stress. Afterward, the blood pressure readings are downloaded into a computer and analyzed by your doctor.
But ambulatory blood pressure monitoring is generally offered only in specialized blood pressure clinics. The testing costs about $200 but isn't always fully reimbursed by insurance. Also, people sometimes find it hard to sleep when they're wearing the device.
The alternative—using a home blood pressure monitor—requires some diligence. But recent technological advances have made the process a lot simpler, says Dr. Antman. In the past, his patients would scribble their blood pressure readings on scraps of paper. "It was usually some piece of mail they were going to throw away that was nearby when they were checking their blood pressure," he says.
Easier home monitoring
These days, you can purchase a digital home blood pressure monitor with a cord that plugs into your smartphone. And two companies, Withings and iHealth, have FDA-approved blood pressure devices that send readings wirelessly to your phone. Either way, you don't have to worry about losing that piece of paper, and you can email the data directly to your doctor's office.
To get the most accurate blood pressure measurement, sit in a quiet room with your back and arm supported. Wait five minutes before starting the machine. After the first reading, relax for another minute. Then do it two more times, taking a minute to relax in between. Take your blood pressure on different days of the week, at different times of day, making note of your recent activities and what time you took any medication.
A patient-centric approach
Current guidelines suggest that most people aim for a reading of 140/90 millimeters of mercury (mm Hg) or lower. But recent findings suggest that an even lower target (a systolic reading of less than 120 mm Hg) may prevent more cardiovascular complications and deaths. By providing your doctor with real-world information from your home monitoring, you'll take a more active role in deciding what blood pressure goal makes sense for you and whether you need more (or less) medication, says Dr. Antman.
Top 3 tips to lower blood pressure
To estimate your health risks from high blood pressure, use the American Heart Association's risk calculator at /bp-risk, where you'll also find additional information about lifestyle changes to reduce blood pressure. |
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.















