Help for hemorrhoids
One of the most embarrassing conditions also can be one of the easiest to treat and manage.
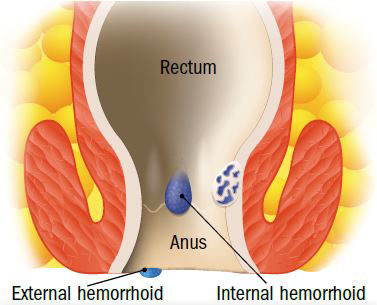
Image: © ttsz/Thinkstock
Hemorrhoids are without doubt among the most unpleasant of health topics. But if you have suffered from them, you may find comfort in knowing that you are not alone.
More than 75% of people ages 45 and older have had hemorrhoids, with symptoms like rectal pain, itching, and bleeding after a bowel movement.
"Hemorrhoids can be painful and embarrassing, but they often shrink on their own with simple self-help and over-the-counter remedies," says Dr. Howard LeWine, assistant professor of medicine at Harvard Medical School.
A look inside
Hemorrhoids are swollen veins near the anus. There are two types: internal and external. You can have either type by itself, or both at the same time.
Internal hemorrhoids form inside the anal canal and are often painless. However, they may cause intermittent bleeding, usually with bowel movements, and sometimes discharge mucus. Internal hemorrhoids may also protrude outside the anus, where they appear as small, grape-like masses.
External hemorrhoids form just outside the anal opening, where they primarily cause swelling, bothersome protrusions, and discomfort.
Cause and self-care
Sometimes hemorrhoids develop for no apparent reason, but often they are associated with chronic constipation or diarrhea, straining during bowel movements, and prolonged sitting on the toilet. This can interfere with blood flow to and from the rectum (the last six inches of the large intestine) and the anus, causing blood to pool in the veins around the anus, enlarging them.
The good news is that neither kind of hemorrhoid is dangerous, and severe complications are rare. Still, it's important to see your doctor if you experience rectal bleeding, feel a lump in the anus, or have ongoing rectal pain, as these might be signs of an unrelated and more serious condition, such as colorectal or rectal cancer.
Symptoms for either kind of hemorrhoid often can be relieved with self-care treatments. For example:
Sitz baths. A regular sitz bath can relieve itching and irritation. Fill a tub with three to four inches of warm (not hot) water and sit in it with your knees bent for about 10 to 15 minutes. Gently pat yourself dry with a towel.
Fiber supplements. These reduce hemorrhoid bleeding, inflammation, and enlargement by drawing water into your stool to make it easier to pass. A psyllium husk fiber supplement, such as Metamucil or a generic equivalent, is a good choice, although psyllium may cause gas or bloating. In that case, try a supplement containing wheat dextrin (Benefiber) or methylcellulose (Citrucel).
Topical therapies. Over-the-counter products are available for hemorrhoids, such as pads infused with witch hazel (Tucks), as well as soothing creams that contain lidocaine, hydrocortisone, or other ingredients like phenylephrine (Preparation H). These substances help shrink the inflamed tissue and provide relief from itching. External hemorrhoids rarely need more than self-care.
"The exception is a thrombosed hemorrhoid, the sudden formation of a hard, inflamed clot inside the hemorrhoid," says Dr. LeWine. "If this occurs, contact your doctor, since you may need a surgical procedure."
Nonsurgical options
When internal hemorrhoids continue to cause symptoms despite home treatment, your doctor may recommend an office-based nonsurgical procedure. Here are the most common options.
Rubber band ligation. This is the most widely used procedure for treating internal hemorrhoids. The doctor inserts a small elastic band into the anal canal and places it around the base of a hemorrhoid. The band cuts off the hemorrhoid's circulation, which causes the hemorrhoid to wither and die. The rubber band eventually falls off unnoticed. The procedure requires no anesthesia, although a numbing agent is sometimes used if you feel discomfort.
Sclerotherapy. The doctor inserts a proctoscope (a special metal or plastic scope used to view the hemorrhoids) into the anus. He or she then injects a chemical solution directly into the hemorrhoid or the area around it. This solution causes a local reaction that interferes with blood flow inside the hemorrhoid, causing it to shrink. Afterward, some people experience mild bleeding, pain, and pressure.
Coagulation therapy. This uses heat, laser, or electric current to cut off the hemorrhoid's blood supply. Once the hemorrhoid shrinks and dies, scar tissue forms on the anal canal wall to hold nearby veins in place so they don't bulge into the anal canal. One hemorrhoid is treated at a time, with a 10- to 14-day period between treatments.
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.