What to do about pelvic organ prolapse
Many women are living with uncomfortable pelvic organ prolapse. Here are your next steps if you're one of them.

One of the most uncomfortable—and awkward—conditions that afflicts women is pelvic organ prolapse. Normally, the pelvic organs—the bladder, uterus, vagina, and rectum—are supported and held in place by a group of muscles and tissues called the pelvic floor. When these muscles weaken over time, the pelvic organs can droop down and bulge out of the vagina.
In addition to the sensation of feeling an uncomfortable bulge in the vagina, you can experience symptoms such as
- pain or pressure in the pelvis, the lower back, or both
- urinary problems, like urine leaking or the feeling that you need to constantly urinate
- constipation
- painful sex.
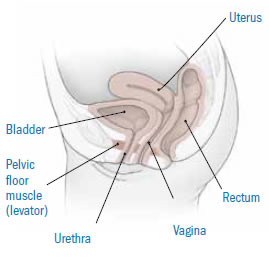
Normal positions of pelvic organs
Image: Thinkstock In pelvic organ prolapse, the pelvic floor |
What is pelvic organ prolapse?
How prolapse is named depends on which organ is affected:
- Cystocele is when the bladder protrudes into the vagina, creating a bulge. It's the most common form of prolapse.
- Rectocele is when the rectum bulges into the back wall of the vagina.
- Uterine prolapse involves the uterus dropping into the vagina.
Most of the time, pelvic organ prolapse is the result of carrying—and vaginally delivering—children, which weakens the pelvic floor. "The baby's head going through the vaginal canal stretches out the connective tissues," says Dr. May Wakamatsu, assistant professor at Harvard Medical School and division director of Female Pelvic Medicine and Reconstructive Surgery at Massachusetts General Hospital.
Getting older, being overweight, and having a condition that involves frequent coughing (which increases pressure in the abdomen and pelvis) also make a woman vulnerable to prolapse.
In pelvic organ prolapse, the pelvic floor muscles weaken, causing one or more of the pelvic organs to fall downward into or out of the vagina.
Pelvic prolapse symptoms
If you have pelvic organ prolapse, you'll notice a bulge at the opening of the vagina. The bulge isn't dangerous, but it can be very uncomfortable.
When the prolapse pulls the bladder downward, it bends the ureter (the tube through which urine exits the body). As a result, you might have trouble urinating fully. "It's like bending a garden hose," Dr. Wakamatsu says. Likewise, if the prolapse pulls the rectum downward, it can cause constipation.
As embarrassing as pelvic organ prolapse can be to talk about, it's something you need to discuss with your primary care physician or gynecologist. Letting it go can leave urine in your bladder, which can lead to urinary tract infections.
Treatment of pelvic organ prolapse
The first treatment your doctor might recommend is pelvic floor physical therapy, which may include Kegel exercises. You squeeze and release the muscles you use to hold in gas, which strengthens the muscles that help to support the pelvic organs.
It's important to do Kegels the right way, Dr. Wakamatsu says. A physical therapist can use techniques like biofeedback to help you find the right muscles to squeeze. Physical therapy with Kegels may be enough to relieve prolapse symptoms.
Your doctor might also recommend a device called a pessary. Pessaries are made from silicone and come in many different shapes. The pessary is inserted into the vagina to help support the prolapsed organs. It is usually fitted to you, and it's removable.
Surgery is an option for women who aren't comfortable with the idea of using a pessary, or who have tried it and found it didn't relieve their symptoms. There are several different types of surgery, based on the location and severity of the prolapse and other health issues. For women who have uterine prolapse, often a hysterectomy (removing the uterus) is recommended. Women who are at high risk for repeated prolapse may have a procedure called sacrocolpopexy, in which the surgeon works through small incisions in the abdomen to reposition the pelvic organs back where they should be.
How to prevent pelvic organ prolapse
"Women should lose weight if they're overweight. They should stop smoking because it can lead to repetitive coughing," Dr. Wakamatsu says. "And they should protect their pelvic floor by pulling in their lower abdominal muscles and tightening their pelvic floor muscles when they lift heavy objects."
Image: © FilippoBacci | GettyImages
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.