"Stress" cardiomyopathy: A different kind of heart attack

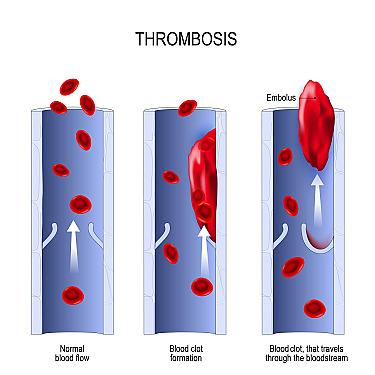
Most heart attacks are due to coronary arteries being blocked by blood clots that form when plaques of cholesterol rupture. The lack of blood flow through the blocked arteries results in heart muscle dying — hence the name "heart attack." However, there is another form of heart attack called takotsubo cardiomyopathy.
Over the past few years, physicians have come to recognize and better understand this form of heart attack. This unusual type of heart attack does not involve rupturing plaques or blocked blood vessels. It is called takotsubo cardiomyopathy, or stress cardiomyopathy. Japanese doctors, who were the first to describe this condition, named it "takotsubo" because during this disorder, the heart takes on a distinctive shape that resembles a Japanese pot used to trap an octopus. Takotsubo cardiomyopathy was commonly believed to be caused by sudden emotional stress, such as the death of a child, and to be far less harmful than a typical heart attack. For that reason, some had also labeled this condition "broken-heart syndrome."
A study in the September 3, 2015 issue of The New England Journal of Medicine reports on the work of an international collaboration of physicians from the United States and Europe that studied 1,750 patients with takotsubo cardiomyopathy. Interestingly, 90% of these cases occurred in women, and the women in this study were an average of 67 years old. The most common triggers of stress cardiomyopathy were physical (such as lung problems or infections), and the next most common cause was an emotional "shock." But in a substantial proportion of patients, there was no trigger that could be identified.
Compared with people who had experienced a "typical" heart attack, patients with takotsubo cardiomyopathy were almost twice as likely to have a neurological or psychiatric disorder. And in contrast to the commonly-held belief among doctors that takotsubo cardiomyopathy is less serious than other forms of heart attack, the rates of death in the hospital between takotsubo cardiomyopathy and more "traditional" heart attacks were similar.
As awareness of takotsubo cardiomyopathy increases among physicians and patients, I suspect we will be recognizing even more cases of takotsubo cardiomyopathy in the future. The condition certainly does not appear to be as rare as was suspected, nor as harmless as had been believed.
Future research will be needed to determine the best care for patients with takotsubo cardiomyopathy and lower their risk for future problems. Right now, we often use the same medications to treat weakened heart muscle in takotsubo cardiomyopathy as we do with other forms of heart attack, but there really are not many good studies yet regarding the optimal medication choices for people who have experienced takotsubo cardiomyopathy. The link with neurological or psychiatric disorders is intriguing, and suggests that an important heart–mind connection is relevant to some manifestations of takotsubo cardiomyopathy, and possibly to other cardiac conditions as well.
About the Author

Deepak L. Bhatt, M.D., M.P.H, Former Editor in Chief, Harvard Heart Letter
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.











.jpg)

