How to release a frozen shoulder: 5 stretches to use
Simple activities can be impossible when you have a frozen shoulder. But what is a frozen shoulder, exactly?
- Reviewed by Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Frozen shoulder (also called adhesive capsulitis) is a common disorder that causes pain, stiffness, and loss of normal range of motion in the shoulder. The resulting disability can be serious, and the condition tends to get worse with time if it's not treated. It affects mainly people ages 40 to 60 with women affected more often than men.
Frozen shoulder symptoms
With frozen shoulder, the shoulder feels stiff, painful, and has limited motion in all directions. Symptoms of a frozen shoulder include
- stiffness that worsens at first, but gradually begins to improve over time
- dull, aching pain that increases as the disease progresses, and may worsen when you move your arm.
A frozen shoulder may take two to nine months to develop. Although the pain may slowly improve, stiffness continues, and range of motion remains limited.
Anatomy of a frozen shoulder
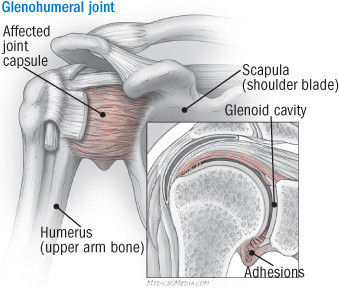
The shoulder has a wider and more varied range of motion than any other part of the body. It pivots mainly on a ball-and-socket arrangement called the glenohumeral joint, which joins the top of the humerus (upper arm bone) to a scooped-out part of the scapula (shoulder blade) called the glenoid cavity (see the illustration below).
The glenohumeral joint helps move the shoulder forward and backward and allows the arm to rotate and extend outward from the body. A flexible capsule filled with a lubricant called synovial fluid protects the joint and helps keep it moving smoothly. The capsule is surrounded by ligaments that connect bones to bones, tendons that fasten muscles to bones, and fluid-filled sacs called bursae that cushion tendons and bones during motion.
The band of muscles and tendons that stabilizes the shoulder and controls its movements is called the rotator cuff. This elaborate architecture of soft tissues accounts for the shoulder's marvelous flexibility, but also makes it vulnerable to trauma as well as chronic wear and tear.
|
Normally, the head of the humerus moves smoothly in the glenoid cavity, a depression in the scapula. A shoulder is "frozen" when the capsule protecting the glenohumeral joint contracts and stiffens. Scar tissue (adhesions) may also form between the joint capsule and the head of the humerus. |
Frozen shoulder causes
We don't fully understand what causes a frozen shoulder, but an inflammatory process is probably involved. Sometimes freezing occurs because the shoulder has been immobilized for a long time by injury, surgery, or illness. In many cases the cause is obscure. Fortunately, the shoulder can usually be unfrozen, though full recovery takes time — and lots of self-help.
The process usually begins with an injury (such as a fracture) or inflammation of the soft tissues, typically due to overuse injuries such as bursitis or tendinitis of the rotator cuff. Inflammation causes pain that is worse with movement and limits the shoulder's range of motion.
When the shoulder becomes immobilized in this way, the connective tissue surrounding the glenohumeral joint — the joint capsule — thickens and contracts, losing its normal capacity to stretch. Trying to avoid the pain caused by moving the shoulder leads to further contraction of the capsule. The humerus has less space to move in, and the joint may lose its lubricating synovial fluid. In advanced cases, bands of scar tissue (adhesions) form between the joint capsule and the head of the humerus.
Who gets frozen shoulder?
The frozen shoulder risk is increased by the following factors:
- lack of exercise therapy after tendinitis or an injury
- wearing a sling for more than a few days without intermittent stretching
- rotator cuff disorders (about 10% of people with these rotator cuff disorders develop frozen shoulder)
- enforced immobility resulting from a stroke, heart condition, or surgery
- other conditions such as thyroid disorders or Parkinson's disease
Frozen shoulder treatment
If you think you have a frozen shoulder or are already developing one, see your clinician or a shoulder expert for a physical exam. To assess your shoulder's range of motion, the clinician will ask you to perform various movements with your arm. These movements may include reaching across your chest to touch the opposite shoulder or down your back to touch the opposite shoulder blade (the Apley scratch test).
Your healthcare provider may take x-rays to make sure there's no other underlying problem, such as arthritic changes or a dislocation. An MRI may be ordered to check for a rotator cuff tear.
The treatment for a frozen shoulder is focused on relieving pain and restoring the shoulder's normal range of motion. Your clinical will develop your treatment plan. Treatment for frozen shoulder may include the following:
- anti-inflammatory medication such as aspirin, ibuprofen (Motrin, Advil), or naproxen (Aleve, Naprosyn, Anaprox)
- an ice pack or bag of frozen vegetables applied to the shoulder for 10 to 15 minutes several times a day can also help with pain
- corticosteroid injection into the shoulder joint or soft tissues
- physical therapy is the cornerstone of treatment, especially concentrating first on exercises that stretch the joint capsule, and later, on strengthening exercises. A physical therapist can show you how far to push yourself and can teach you the appropriate exercises. Once you've learned your limitations, you can practice most of your exercises on your own at home.
As you work to stretch the shoulder capsule, you should avoid any activities that require overhead reaching, lifting, or anything else that aggravates your pain. If you diligently follow your regimen of frozen shoulder exercises, it's likely that you'll be able to resume your usual level of activity (more than 90% of people improve with these nonsurgical measures).
But full recovery from a frozen shoulder takes time — from several months to two or three years. If you don't improve steadily or if you reach a plateau, go back to your clinician or consult a shoulder expert. Rarely, recalcitrant cases require surgery.
5 frozen shoulder exercises
Always warm up your shoulder before performing your exercises. The best way to do that is to take a warm shower or bath for 10 to 15 minutes. You can also use a moist heating pad or damp towel heated in the microwave, but it may not be as effective.
In performing the following exercises, stretch to the point of tension but not pain.
Pendulum stretch
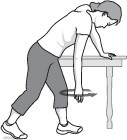
(Perform this exercise first.)
- Relax your shoulders.
- Stand and lean over slightly, allowing your affected arm to hang down.
- Swing the arm in a small circle — about a foot in diameter.
- Perform 10 revolutions in each direction, once a day.
- As your symptoms improve, increase the diameter of your swing, but never force it.
- When you're ready for more, increase the stretch by holding a light weight (three to five pounds) in the swinging arm.
Towel stretch
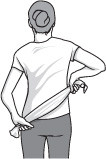
- Grasp a three-foot-long towel with both hands behind your back, and hold it in a horizontal position.
- Use your good arm to pull the affected arm upward to stretch it.
- You can also perform an advanced version of this exercise with the towel draped over your good shoulder.
- Grasp the bottom of the towel with the affected arm and pull it toward the lower back with the unaffected arm.
- Do this stretch 10 to 20 times a day.
Finger walk
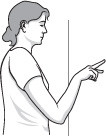
- Face a wall three-quarters of an arm's length away.
- Reach out and touch the wall at waist level with the fingertips of the affected arm.
- With your elbow slightly bent, slowly walk your fingers up the wall, spider-like, until you've raised your arm to shoulder level, or as far as you comfortably can. Your fingers should be doing the work, not your shoulder muscles.
- Slowly lower the arm (with the help of the good arm, if necessary) and repeat.
- Perform this exercise 10 to 20 times a day.
Cross-body reach
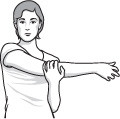
- Sit or stand.
- Use your good arm to lift your affected arm at the elbow, and bring it up and across your body, exerting gentle pressure to stretch the shoulder.
- Hold the stretch for 15 to 20 seconds.
- Do this stretch 10 to 20 times per day.
Armpit stretch
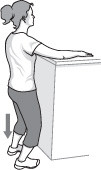
- Using your good arm, lift the affected arm onto a shelf about breast-high.
- Gently bend your knees, opening up the armpit.
- Deepen your knee bend slightly, gently stretching the armpit, and then straighten.
- With each knee bend, stretch a little further, but don't force it.
- Do this stretch 10 to 20 times each day.
Strengthening the rotator cuff
After your range of motion improves, you can add rotator cuff–strengthening exercises. Be sure to warm up your shoulder and do your stretching exercises before you perform strengthening
Outward rotation

- Hold a rubber exercise band between your hands with your elbows at a 90-degree angle close to your sides.
- Rotate the lower part of the affected arm outward two or three inches and hold for five seconds.
- Repeat 10 to 15 times, once a day.
Inward rotation
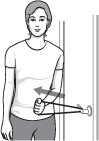
- Stand next to a closed door, and hook one end of a rubber exercise band around the doorknob.
- Grasp the other end with the hand of the affected arm, holding the elbow at a 90-degree angle.
- Pull the band toward your body two or three inches and hold for five seconds.
- Repeat 10 to 15 times, once a day.
About the Reviewer

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.