Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Physical therapy provides modest improvement for chronic low back pain

Scoliosis treatment: Can it help as you get older?
How to boost your immune system
Helpful ways to strengthen your immune system and fight off disease.
How can you improve your immune system? On the whole, your immune system does a remarkable job of defending you against disease-causing microorganisms. But sometimes it fails: A germ invades successfully and makes you sick. Is it possible to intervene in this process and boost your immune system? What if you improve your diet? Take certain vitamins or herbal preparations? Make other lifestyle changes in the hope of producing a near-perfect immune response?
What can you do to boost your immune system?
The idea of boosting your immunity is enticing, but the ability to do so has proved elusive for several reasons. The immune system is precisely that — a system, not a single entity. To function well, it requires balance and harmony. There is still much that researchers don't know about the intricacies and interconnectedness of the immune response. For now, there are no scientifically proven direct links between lifestyle and enhanced immune function.
But that doesn't mean the effects of lifestyle on the immune system aren't intriguing and shouldn't be studied. Researchers are exploring the effects of diet, exercise, age, psychological stress, and other factors on the immune response, both in animals and in humans. In the meantime, general healthy-living strategies make sense since they likely help immune function and they come with other proven health benefits.
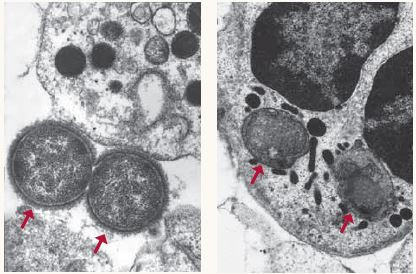
Immunity in action
A healthy immune system can defeat invading pathogens as shown above, where two bacteria are no match for the white blood cell that engulfs and kills them (see arrows). Photos courtesy of Michael N. Starnbach, Ph.D., Harvard Medical School |
Healthy ways to strengthen your immune system
Your first line of defense is to choose a healthy lifestyle. Following general good-health guidelines is the single best step you can take toward naturally keeping your immune system working properly. Every part of your body, including your immune system, functions better when protected from environmental assaults and bolstered by healthy-living strategies such as these:
- Don't smoke.
- Eat a diet high in fruits and vegetables.
- Exercise regularly.
- Maintain a healthy weight.
- If you drink alcohol, drink only in moderation.
- Get adequate sleep.
- Take steps to avoid infection, such as washing your hands frequently and cooking meats thoroughly.
- Try to minimize stress.
- Keep current with all recommended vaccines. Vaccines prime your immune system to fight off infections before they take hold in your body.
Increase immunity the healthy way
Many products on store shelves claim to boost or support immunity. But the concept of boosting immunity actually makes little sense scientifically. In fact, boosting the number of cells in your body — immune cells or others — is not necessarily a good thing. For example, athletes who engage in "blood doping" — pumping blood into their systems to boost their number of blood cells and enhance their performance — run the risk of strokes.
Attempting to boost the cells of your immune system is especially complicated because there are so many different kinds of cells in the immune system that respond to so many different microbes in so many ways. Which cells should you boost, and to what number? So far, scientists do not know the answer. What is known is that the body is continually generating immune cells. Certainly, it produces many more lymphocytes than it can possibly use. The extra cells remove themselves through a natural process of cell death called apoptosis — some before they see any action, some after the battle is won. No one knows how many cells or what the best mix of cells the immune system needs to function at its optimum level.
Immune system and age
As we age, our immune response capability becomes reduced, which in turn contributes to more infections and more cancer. As life expectancy in developed countries has increased, so too has the incidence of age-related conditions.
While some people age healthily, the conclusion of many studies is that, compared with younger people, the elderly are more likely to contract infectious diseases and, even more importantly, more likely to die from them. Respiratory infections, including, influenza, the COVID-19 virus, and particularly pneumonia are leading causes of death in people over 65 worldwide. No one knows for sure why this happens, but some scientists observe that this increased risk correlates with a decrease in T cells, possibly from the thymus atrophying with age and producing fewer T cells to fight off infection. Whether this decrease in thymus function explains the drop in T cells or whether other changes play a role is not fully understood. Others are interested in whether the bone marrow becomes less efficient at producing the stem cells that give rise to the cells of the immune system.
A reduction in immune response to infections has been demonstrated by older people's response to vaccines. For example, studies of influenza vaccines have shown that for people over age 65, the vaccine is less effective compared to healthy children (over age 2). But despite the reduction in efficacy, vaccinations for influenza, COVID-19 and S. pneumoniae have significantly lowered the rates of sickness and death in older people when compared with no vaccination.
There appears to be a connection between nutrition and immunity in the elderly. A form of malnutrition that is surprisingly common even in affluent countries is known as "micronutrient malnutrition." Micronutrient malnutrition, in which a person is deficient in some essential vitamins and trace minerals that are obtained from or supplemented by diet, can happen in the elderly. Older people tend to eat less and often have less variety in their diets. One important question is whether dietary supplements may help certain people maintain a healthier immune system.
Diet and your immune system
Like any fighting force, the immune system army marches on its stomach. Healthy immune system warriors need good, regular nourishment. Scientists have long recognized that people who are malnourished are more vulnerable to infectious diseases. For example, researchers don't know whether any particular dietary factors, such as processed foods or high simple sugar intake, adversely affects immune function.
There is some experimental evidence that various micronutrient deficiencies — for example, deficiencies of zinc, selenium, iron, copper, folic acid, and vitamins A, B6, C, and E — alter cellular immune responses. However, whether that translates to changes in the human immune system and impacts on health remain unknown.
So, what can you do? If you suspect your diet is not providing you with all your micronutrient needs — maybe, for instance, you don't like vegetables — taking a daily multivitamin and mineral supplement may bring other health benefits, beyond any possibly beneficial effects on the immune system. Taking megadoses of a single vitamin does not. More is not necessarily better.
Improve immunity with herbs and supplements?
Walk into a store, and you will find bottles of pills and herbal preparations that claim to "support immunity" or otherwise boost the health of your immune system. Although some preparations have been found to alter some components of immune function, thus far there is no evidence that they actually bolster immunity to the point where you are better protected against infection and disease. Demonstrating whether an herb — or any substance, for that matter — can enhance immunity is, as yet, a highly complicated matter. Scientists don't know, for example, whether an herb that seems to raise the levels of antibodies in the blood is actually doing anything beneficial for overall immunity.
Does being cold give you a weak immune system?
Almost every mother has said it: "Wear a jacket or you'll catch a cold!" Is she right? Probably not, exposure to moderate cold temperatures doesn't increase your susceptibility to infection. There are two reasons why winter is "cold and flu season." In the winter, people spend more time indoors, in closer contact with other people who can pass on their germs. Also the influenza virus stays airborne longer when air is cold and less humid.
A group of Canadian researchers that has reviewed hundreds of medical studies on the subject and conducted some of its own research concludes that there's no need to worry about moderate cold exposure — it appears to have no detrimental effect on the human immune system. Should you bundle up when it's cold outside? The answer is "yes" if you're uncomfortable, or if you're going to be outdoors for an extended period where such problems as frostbite and hypothermia are a risk. But don't worry about immunity.
Exercise: Good or bad for immunity?
Regular exercise is one of the pillars of healthy living. It improves cardiovascular health, lowers blood pressure, helps control body weight, and protects against a variety of diseases. But does it help to boost your immune system naturally and keep it healthy? Just like a healthy diet, exercise can contribute to general good health and therefore to a healthy immune system.
Image: lzf/Getty Images
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Physical therapy provides modest improvement for chronic low back pain

Scoliosis treatment: Can it help as you get older?
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up