When your child ends up in the emergency room
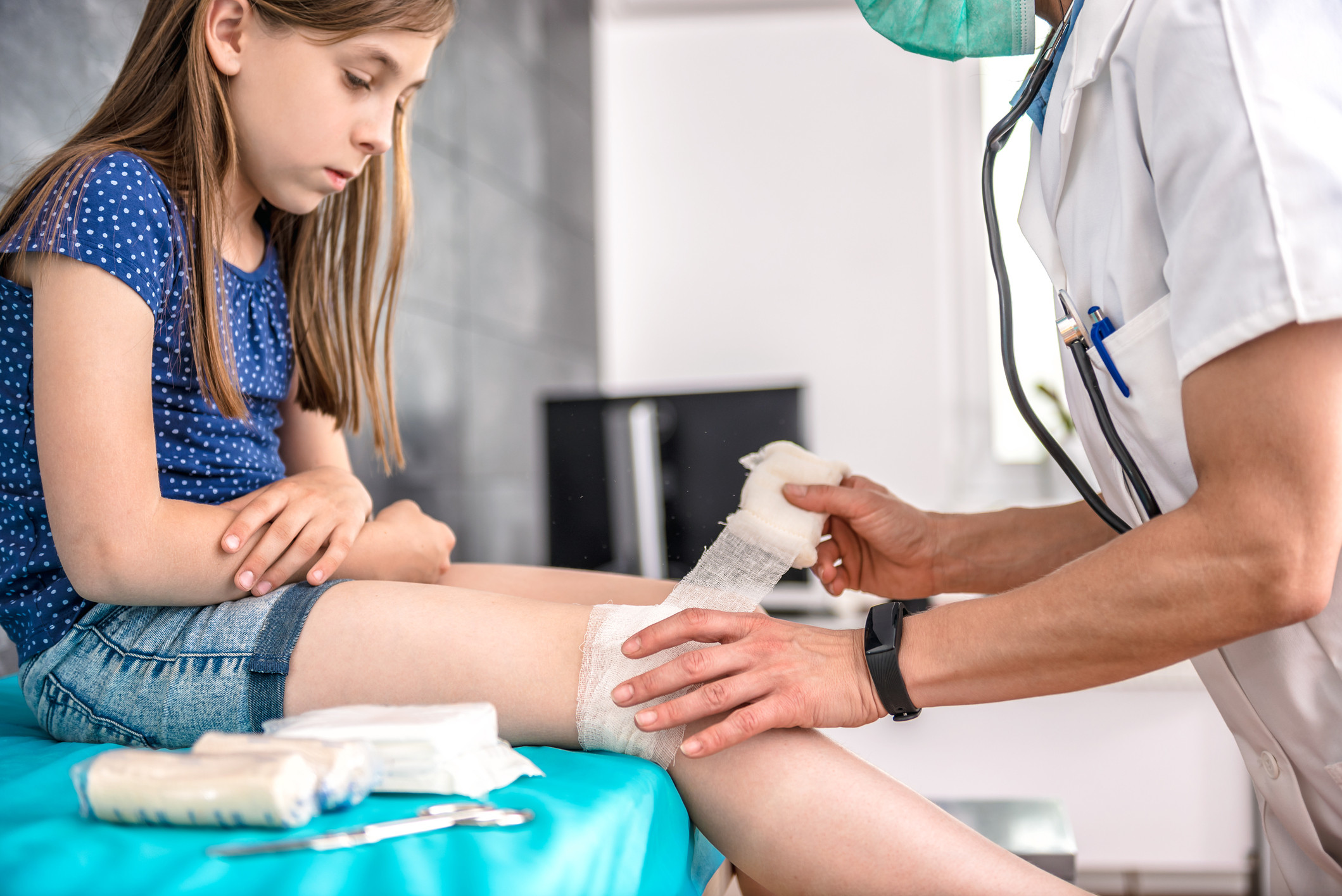
I recently wrote about a walk I took with my sons, where I slipped, falling onto my youngest who fell onto a rock, which cut his forehead and meant a trip to the emergency room for four stitches.
It wasn't our first visit, but thankfully, it's never been for anything dire. My kids have just run into and jumped off a variety of things, so there's been broken bones, forehead cuts (they have matching pairs), along with spiked temperatures that invariably happen when the pediatrician's office isn't open.
I'm pretty good at keeping my head, but I'm not at my best in an ED. I end up being too polite and defer="defer"ential. In essence, I say, "Stop this bleeding now, and in exchange, I won't bug you with more than two questions. Promise."
How to advocate for your child in the emergency room
It's not a winning formula. Doctors have skill, but they're just people. They're often rushed and can't know everything about my child. They will fail to cover everything that worries me and my wife. Bottom line: they need help, and that means, because I'm the biggest expert on my child — side note: remember that I'm the biggest expert on my child — I need to ask questions, share relevant information, and, occasionally, be a pain.
But before I resort to that last part, I want to work with you, doc, and to do that, I'll try to be clearheaded and give you useful information up top.
Help the emergency room doctor help your child
It's not close to an exhaustive list, but Dr. Vincent Chiang, Harvard Medical School associate professor of pediatrics and emergency medicine and emergency room physician at Boston Children's Hospital, has some suggestions of what to share:
- Your child's ability to cope with any part of a medical visit. Do not equivocate. "He does not like … shots, blood, being sick, pain, lying still, anything doctors" is all helpful. Some hospitals have child life specialists that can help reduce the stress. It would be stellar if the doctor mentions it and calls for one. If not, ask if someone's available.
- "This is our first time dealing with this." For the doctor, most stuff registers as routine, but it's not for parents, and saying this should be enough of a reminder to explain everything slowly, fully, and clearly. If it's not, repeat it.
- "She never complains" or "He complains about everything." It tells the doctor two things: something is different, and that worried you enough to come in. It can be hard to pinpoint, but try to verbalize your big concern ("My uncle had a headache and it turned out to be a tumor"). The doctor can possibly address it, so you're not unnecessarily sitting with it.
None of this guarantees quick answers, Chiang says. Some conditions only fully reveal themselves over time. Sometimes tests are needed. If so, ask if they're being done to rule out things or to look for something specific. More pointedly, ask the doctor if there's anything that's worrisome. And then ask when you two will have the next discussion, since all of this entails waiting, and that's often the most stressful part.
Four things to know when you leave the emergency room
It's understandable to forget questions and not mention every relevant detail. But before you leave the hospital, Chiang says to know these four things:
- The diagnosis. It's simple, but you want to be clear on what the doctor decided your child was being treated for.
- The treatment plan. It needs to address the medical problem and the comfort measures. Example: Sprained ankle. Rest, ice, compression, elevation. If there's pain or nausea or other discomfort, know your options for relief.
- The follow-up plan. It could be meeting with your pediatrician or a specialist, but it's rare that there would be nothing to do. At the least, let your pediatrician know what happened as soon as possible and make sure that the follow-up plan makes sense. You cannot assume that the hospital will provide the information.
- The reasons to return. Most often, when you leave the emergency room, follow-up happens outside of the hospital, but you want to know what signs and symptoms suggest urgent care is needed again. You also want to know when things should start to go back to normal.
Make sure you're clear on the treatment plan
Of the above four, Chiang says that the treatment plan causes the most confusion, because when you're hearing it, you're also hearing that your child is going home. You naturally become relaxed and the doctor might start moving on to a different patient. But there are still things to know, like if your kid can play sports or go to school/daycare, and, if not, when. There's also the medication. Be sure of the dosing and timing, and why your child is taking it. Ask if there are interactions with other medications or additional precautions (for example, avoiding the sun, a side effect we recently experienced with an antibiotic), and how soon the first dose has to be taken, double-checking if it was already given in the hospital.
One good move is to take the time read the discharge instructions before you leave, and if the doctor hasn't asked you to repeat back what you've heard about the treatment plan, then say, "This is what I understand. Am I correct?" It comes down to getting your questions answered, and that sometimes means pulling out the option of being a pain. It might feel unnatural or uncomfortable, but there's no benefit in keeping anything to yourself. As Chiang says, "I don't know about the question you don't ask me."
About the Author

Steve Calechman, Contributor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.
















