Study backs mammograms for women 50 to 69
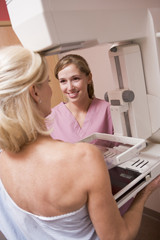
Women routinely subject their breasts to the often uncomfortable exam known as a mammogram because it can detect breast cancer at an early stage and save lives. But it also finds suspicious spots that turn out to be nothing—after more tests, possible some complications, and definitely a lot of worry.
For years researchers have been trying to weigh the benefits of finding early breast cancers against the risks related to false positives (the spots that turn out to be harmless). This work has sparked some bitter public debates and confusion for women over flip-flopping recommendations.
The latest salvo comes from a review of the results of mammograms among more than 12 million women in 18 European countries. From these data, the researchers calculated what they call a “balance sheet” of benefits and harms of routine mammograms. The results were published online in the Journal of Medical Screening.
In a group of 1,000 women who have their first mammogram at age 50, and repeat the test every other year until age 79:
- 800 will have negative mammograms
- 200 will need further testing: 170 will have a noninvasive test (a repeat mammogram, an ultrasound, and/or an MRI) and 30 will have a biopsy or surgery
- 7 to 9 will have their lives saved by detection and treatment of early breast cancer
- 4 will be “overdiagnosed,” meaning the cancers found would not have been detected otherwise or caused any problems during their lives.
The study supports the idea that routine mammograms can prevent deaths from breast cancer without causing undue harm. The findings probably apply to American women, Dr. Virginia Moyer, chair of the U.S. Preventive Services Task force told HealthDay.
Debate
Not all studies have found in favor of routine mammograms. This has led to different opinions about the pros and cons of mammograms to search for early breast cancer, and differing recommendations for when to start and how often to do it.
- The U.S. Preventive Services Task Force recommends that women between the ages of 50 and 74 have a mammogram every other year.
- The National Cancer Institute recommends that women age 40 or older have a mammogram every 1 to 2 years.
- The American Cancer Society recommends that women age 40 and older have a mammogram every year.
The findings from the European study suggest that the U.S. Preventive Services Task Force got it right—start at age 50 and have the test every other year.
Special cases
Women at higher risk of developing breast cancer may need mammograms earlier than age 50, or more often than every other year. Things that increase the risk include:
- Family history. Women who have two or more first-degree relatives (a mother, daughter or sister) with breast or ovarian cancer have a 50% higher risk of developing breast cancer.
- Genes. Some women with a strong family history of breast cancer also have mutations in the BRCA1 or BRCA2 genes. For these women, the lifetime risk of developing breast cancer is 50% to 85%.
- Exposure to radiation. Women who have had high-dose radiation to the chest have an increased risk of developing breast cancer. Radiation usually was done as part of treatment for another cancer (such as Hodgkin’s disease). The risk is especially high if a woman had radiation treatment as a teenager.
- Diethylstilbestrol (DES) exposure. DES was used from the 1940s through the 1960s to prevent miscarriage. It has since been banned. Women who took DES and those who were exposed to it in the uterus have a slightly higher risk of developing breast cancer.
- Other cancers. Breast cancer risk is higher in women who have been diagnosed with cancers of the ovary, colon, or endometrium.
Factors such as breast density, being overweight or obese, and drinking alcohol can increase the risk of breast cancer. They might not change when you start having mammograms or how often you need them, but they make it that much more important for you to have the test.
About the Author

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.















