Let's put the "public" in public defibrillation
Many people say they would shy away from using a defibrillator.
If you were in a public place and saw someone suddenly collapse, would you use a nearby defibrillator to revive him or her? In a survey of 1,000 adults, more than half answered "no."
Automated external defibrillators (AEDs) are the best — and often last — hope for people who collapse because their hearts have lapsed into a fast, irregular, and deadly heartbeat known as ventricular fibrillation. These shock-delivering devices are becoming a standard fixture in airports, malls, casinos, office buildings, and other public places. They are so easy to use, and the directions printed on them are so clear and straightforward, that even schoolchildren can learn to use them in a trice.
To gauge the readiness of the most likely rescuers — untrained bystanders — Dutch researchers surveyed passersby in Centraal Station, a busy rail station in downtown Amsterdam. Each interview was conducted within 10 feet of one of the five AEDs prominently displayed in the station.
More than half of those who took part in the survey could not identify the glass-fronted box on the wall as an emergency defibrillator. And only 47% said they would use the AED if needed. The most common reasons for declining to use the device were not knowing how it works (69%) and worries about hurting the victim (14%).
In order for someone to use an AED, he or she must (1) know that a defibrillator could help revive someone who suddenly collapses, (2) know that AEDs are available in some public places, (3) be able to identify an AED, and (4) be willing to use the device. In the Dutch study, less than 20% of those surveyed met these four requirements (Annals of Emergency Medicine, published online Feb. 4, 2011).
Delivering the shock of a lifetime
Automated external defibrillators use the same basic steps. Most also have a gentle but authoritative computerized voice that gives the user easy-to-follow instructions.
|
Sudden cardiac arrest
There are two types of heart attack. A myocardial infarction is the slower-moving type, caused by a clot blocking a coronary artery. This blockage usually causes chest pain or other warning signs that can last for hours. The second type, called a cardiac arrest, strikes so fast that there's little or no time to call for help. Unless two specific treatments — cardiopulmonary resuscitation (CPR) and an electric shock to the heart — are begun, the chances of surviving or of living without permanent brain damage dwindle with each passing minute.
Most cardiac arrests begin when something pushes the heart into ventricular tachycardia (tack-ee-KAR-dee-uh). In this rhythm, the heart's lower chambers beat very fast. It can give way to ventricular fibrillation (fib-rih-LAY-shun), which is fast and chaotic. In either case, the ventricles are contracting so fast that they don't have time to fill with blood between beats. Circulation ceases.
Several things can trigger ventricular tachycardia or ventricular fibrillation. A myocardial infarction can do it, as can a structural or electrical problem; dehydration; a serious imbalance of potassium, magnesium, or other minerals in the blood; an inherited condition; or a blow to the chest.
Cardiac arrest often comes out of the blue, with few warning signs. A person might feel dizzy, lightheaded, or out of breath, then suddenly collapse. Recognizing the signs in someone else is probably more important than recognizing them in yourself, since there isn't much you can do to help yourself. Knowing what is happening means you can respond quicker, and maybe save a life.
Someone having a cardiac arrest:
-
suddenly faints or collapses
-
stops breathing
-
has no pulse
-
may have twitching muscles.
Keep in mind that a person who has simply fainted keeps breathing and has a pulse. That's not the case with a sudden cardiac arrest.
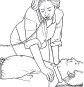
In case of cardiac arrestThese instructions apply if you are with a person who suddenly collapses — a witnessed cardiac arrest. The goal is to start chest compressions immediately, and have someone find an automated external defibrillator (AED). 1. Call 911.
Doing this summons health care professionals and a life-saving defibrillator. If you don't know how to do hands-only cardiopulmonary resuscitation (CPR), the emergency dispatcher may be able to coach you through it. 2. Start CPR.
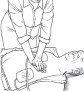
Place your hands on the breastbone in the middle of the person's chest. Press down hard enough to make the chest move inward 1 1/2–2 inches. Relax to let the chest rebound. Repeat this press-and-relax motion quickly, almost twice a second if you can. Each compression circulates blood to the brain and the rest of the body. 3. Restart the heart.
When a defibrillator arrives, ask the person who brought it to attach the pads to the victim's chest so you can keep doing CPR. When everything is ready, stop CPR and follow the directions on the defibrillator. 4. Go back to CPR.
Immediately after the shock, start pushing on the chest again. This helps the heart get back into a normal rhythm. After two minutes, if there doesn't seem to be any recovery, go through the defibrillation process again and get right back to CPR. |
Minutes matter
Someone who collapses with a cardiac arrest usually has enough oxygen in his or her bloodstream to nourish the brain for several minutes. That's why the American Heart Association now recommends doing "hands only" CPR if you witness someone collapse from what looks like a cardiac arrest — no mouth-to-mouth breathing required.
The chances of surviving a cardiac arrest fall about 10% for each minute the heart stays in ventricular fibrillation. Shock the heart back into a normal rhythm within two minutes, and the victim has an 80% chance of surviving. Deliver that shock after seven minutes — the average time it takes an emergency medical team to arrive in many cities — and the odds have slipped below 30%.
If you see someone suddenly collapse, and he or she has no pulse:
Call 911 right away. The sooner professional help arrives, the better.
Start "hands only" CPR. Push hard and fast (about 100 times a minute if you can) on the middle of the person's chest. This keeps blood flowing to the brain and the rest of the body. If you aren't in a public place with a defibrillator handy, keep doing CPR until emergency help arrives. Swap off with a partner if needed.
Use a defibrillator. If you are in a public place such as an airport, ask a bystander to find the nearest AED. Use it to shock the heart out of its deadly pace and back into a normal rhythm (see illustration).
Don't let lack of knowledge keep you from saving a life. Even if you have never done CPR or handled an AED before, trying is better than doing nothing. You can also be prepared — the American Heart Association, American Red Cross, and other organizations offer classes on CPR and using a public defibrillator.
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.