
Driving with arthritis pain: Stay comfortable — and safe — behind the wheel

Daily cup of coffee may prevent afib recurrence
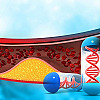
Gene-editing therapy lowers harmful blood fats in early study

What is EMDR therapy, and who can it help?
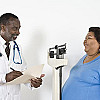
GLP-1 drugs versus bariatric surgery for treating obesity

Two dumbbells, three exercises, and 10 minutes

Easing the emotional burden of IBS

Modify your push-ups to meet your fitness level
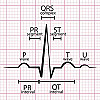
What is long QT syndrome?

Stroke survivors may benefit from very low LDL levels


Managing Shingles: Fending off a persistent threat from a childhood virus
This Harvard Medical School Guide takes a detailed look at shingles and the virus that causes its symptoms, how it's transmitted, how to reduce your chances of getting it, and how to manage the condition if you do get sick.
Other Product Information
If you’re like 95% of American adults, you had chickenpox in childhood. Before the United States started its widespread vaccination program in 1995, there were roughly four million cases of chickenpox every year. Contracting the highly contagious virus, with the itchy, whole-body rash that it causes, was virtually a rite of passage for American children.
Chickenpox, which is caused by the varicella-zoster virus, has no cure. But unlike viruses that your immune system clears from the body within a few days or weeks, the varicella-zoster virus doesn’t leave your body. After your symptoms go away, the virus hangs around, taking up residence and lying dormant in your nerves, with your immune system holding it in check. But later — often decades from the time it first made you sick — varicella-zoster can suddenly emerge and hit you again, this time appearing as a different condition known as shingles.
Like chickenpox, shingles also causes a blistering rash, but this time it generally appears as a painful band around one side of your ribcage, or it may appear on one side of your face. The first symptom for many people is pain or a burning sensation in the affected area. You may also have fever, a headache, and fatigue. Along with the rash and other temporary symptoms, shingles can also bring unpleasant, long-lasting, and sometimes permanent complications such as skin infections, nerve pain in the area where the rash appeared, or even vision loss. Some recent research even hints that people who get shingles also may be temporarily at higher risk for heart attack and stroke.
This Harvard Medical School Guide takes a detailed look at shingles and the virus that causes it: its symptoms, how it’s transmitted, how to reduce your chances of getting it, and how to manage the condition if you do get sick.
Prepared by the editors of Harvard Health Publishing in consultation with Michael Starnbach, Ph.D., Department of Microbiology and Immunobiology, Harvard Medical School; Professor of Nutrition, Harvard T.H. Chan School of Public Health. 16 pages. (2021)
About Harvard Medical School Guides
Harvard Medical School Guides delivers compact, practical information on important health concerns. These publications are smaller in scope than our Special Health Reports, but they are written in the same clear, easy-to-understand language, and they provide the authoritative health advice you expect from Harvard Health Publishing.
- Where does shingles come from?
- Who gets shingles?
- Protective mechanisms in action
- Causes of immune system suppression
- Symptoms of shingles
- Experiencing complications
- Treating shingles
- Preventing shingles
You might also be interested in…

Living Better, Living Longer: Taking steps now to ensure a happier, healthier future

Driving with arthritis pain: Stay comfortable — and safe — behind the wheel

Daily cup of coffee may prevent afib recurrence

Gene-editing therapy lowers harmful blood fats in early study

What is EMDR therapy, and who can it help?

GLP-1 drugs versus bariatric surgery for treating obesity

Two dumbbells, three exercises, and 10 minutes

Easing the emotional burden of IBS

Modify your push-ups to meet your fitness level

What is long QT syndrome?

Stroke survivors may benefit from very low LDL levels
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up