Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Scoliosis treatment: Can it help as you get older?

Physical therapy provides modest improvement for chronic low back pain
Ask Dr. Rob about piriformis syndrome
Common condition is the original pain in the buttocks.
What is it?
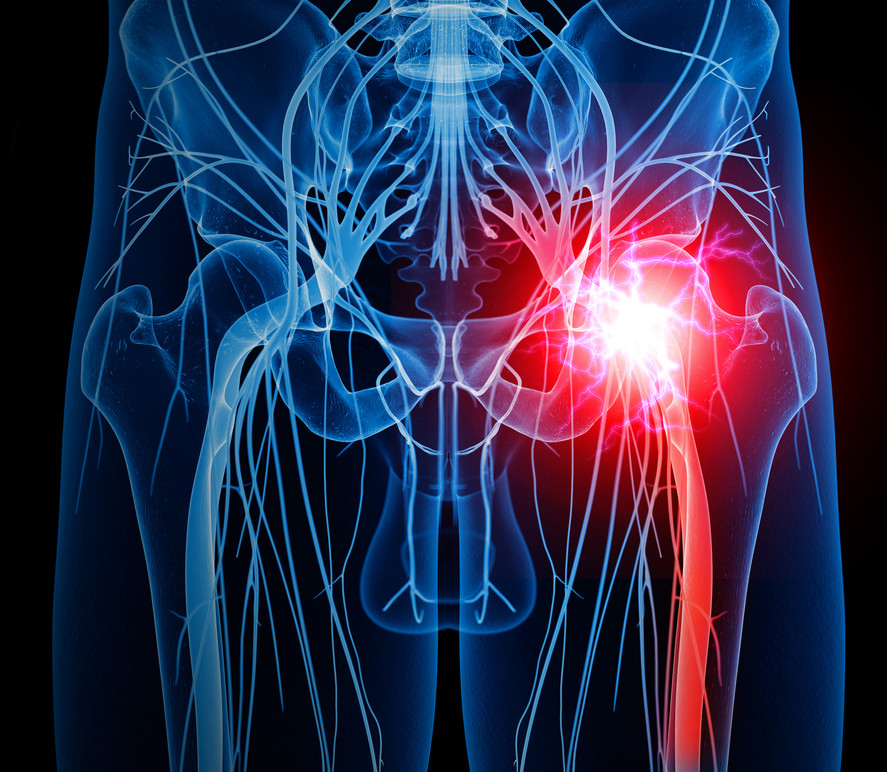
Piriformis syndrome is a painful condition that develops due to irritation or compression of the sciatic nerve near the piriformis muscle. The piriformis muscle connects the lowermost vertebrae with the upper part of the leg after traveling the "sciatic notch," the opening in the pelvic bone that allows the sciatic nerve to travel into the leg. Here, the muscle and nerve are adjacent and this proximity is why trouble can develop.
The condition is relatively common. Estimates suggest that about 5% of cases of sciatica (irritation of the sciatic nerve causing radiating pain from the back or buttock into the leg, calf and foot) are due to piriformis syndrome. It seems to be more common among women though the reason for this is not known.
Symptoms and signs
The typical patient with piriformis syndrome complains of "sciatica" — that is, sharp, severe, radiating pain from the lower back or buttock down the back of the leg and into the thigh, calf, and foot. Symptoms may seem to be due to hip bursitis or disc herniation ("slipped disc") but the doctor's examination helps sort out the true cause because with piriformis syndrome the person also has:
- difficulty sitting or putting weight on the buttock on one side
- muscle spasm of the piriformis muscle
- pain in the piriformis muscle during a rectal exam
- sciatica-type pain when the hip is moved and rotated outward against resistance.
Causes of piriformis syndrome
Recognized causes of piriformis syndrome include:
- injury
- abnormal development or location of the piriformis muscle or sciatic nerve
- abnormal spine alignment (such as scoliosis)
- leg-length discrepancy (when the legs are of different lengths)
- prolonged sitting, especially if carrying a thick wallet in a pocket directly behind the piriformis muscle
- prior hip surgery
- unusually vigorous exercise
- foot problems, including Morton's neuroma.
In many cases the cause cannot be identified.
Diagnosis
The diagnosis is "clinical" meaning that it is based on symptoms and physical examination. There is no specific blood test, biopsy, or imaging test to confirm the diagnosis. For this reason, it is difficult to know for sure that a person has the condition and there is some controversy about how common it is. This is especially true because spine and disc disease can cause similar symptoms and piriformis syndrome can be present along with these other conditions such as hip bursitis.
Expected duration
The duration of piriformis syndrome is variable. Often, it is brief in duration, especially if proper treatment begins soon after symptoms appear.
Prevention
There is no reliable way to prevent piriformis syndrome. For people who have had this or other back problems, standard recommendations include home exercises and stretching, a heel-lift (if the legs are of different lengths), not carrying a wallet in the back pocket, avoiding prolonged sitting, and getting treatment for other contributing conditions (such as spinal arthritis or foot problems). If triggered by vigorous exercise, reducing exercise intensity or changing activities (for example, from running to swimming) can prevent future episodes.
Treatment
While medications, such as pain relievers, muscle relaxants, and anti-inflammatory drugs may be recommended, the mainstay of treatment for piriformis syndrome is physical therapy, exercise, and stretching. Specific treatments may include:
- adjustments in gait
- improved mobility of sacroiliac joints
- stretching to relieve tight piriformis muscles and those surrounding the hip
- strengthening of the hip abductors (muscles that move the hips outward from the body)
- application of heat
- acupuncture.
If these measures are not effective, more invasive treatment can be considered such as:
- injections of a local anesthetic (similar to Novocain), botulinum toxin, and/or a corticosteroid agent — these injections are generally guided by ultrasound, x-ray, or electromyogram (which detects muscle and nerve activity) to make sure the needle is in the right place.
- surgery — Although an option of last resort, removing a portion of the piriformis muscle or its tendon has been reported to provide relief in refractory cases.
Prognosis
With prompt diagnosis and treatment, the prognosis is quite good. However, the condition may become recurrent or chronic; a poor outcome may be more likely if the diagnosis and treatment are delayed.
The bottom line
Piriformis syndrome may be the most common cause of sciatic-type back pain you've never heard of; or it may be rare, no one is really sure. If you have persistent, unexplained buttock pain that travels into the leg, stop carrying your wallet in your back pocket, try not to sit so much, and see your doctor. You might have a disc problem or some other common back trouble; but you could have piriformis syndrome and finding out sooner rather than later can make a difference.
To understand why back pain occurs and which treatments are most likely to help, get the Harvard Special Health Report Back Pain: Finding solutions for your aching back.
Image: Eraxion/Getty Images
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.

Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Scoliosis treatment: Can it help as you get older?

Physical therapy provides modest improvement for chronic low back pain
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up