Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Scoliosis treatment: Can it help as you get older?

Physical therapy provides modest improvement for chronic low back pain
Heart Health Archive
Articles
How atrial fibrillation may affect your brain
This heart rhythm disorder is linked to thinking and memory problems. But anti-clotting drugs may lower the risk.
Bouts of atrial fibrillation, or afib — a rapid, chaotic heartbeat — make some people feel lightheaded and dizzy, while others don't notice any symptoms. But the most serious threat of this condition is the higher risk of stroke among people with afib compared with those without the disorder (see "Blood clot dangers, large and small"). Now, there's a growing recognition that people with afib also face an increased risk of thinking and memory problems — even if they do not experience a stroke.
Known as cognitive impairment, these problems include trouble remembering, learning new things, concentrating, or making routine decisions. The presumed underlying cause? Tiny blood clots that cause "silent" (that is, unrecognized) strokes and gradually injure parts of the brain involved with cognition.
Vegetable of the month: Peppers
Image: © Josef Mohyla/Getty Images
Peppers, which belong to the genus Capsicum, come in a variety of colors, shapes, sizes, and flavors. Bell peppers (available in green, yellow, orange, red, and even purple) make a nice addition to a salad or plate of crudités. Supermarkets carry bags of assorted mini bell peppers that are convenient both for snacking and using in recipes.
While sweet bell peppers are crunchy and mild, hot peppers — such as jalapeños, serranos, and habaneros — provide a tongue-tingling punch of heat. They contain varying amounts of the phytochemicals responsible for the spiciness in hot peppers.
Inherited high cholesterol often goes untreated
Research we're watching
About four in 1,000 adults in this country are born with a genetic condition marked by abnormally high cholesterol levels, known as familial hypercholesterolemia (FH). Their "bad" LDL cholesterol can be two to three times as high as the common target LDL value of 100 milligrams per deciliter (mg/dL) or lower for healthy people. But only about half of people with FH are getting proper treatment for the disease, according to a report in the May 22 issue of Circulation.
For the study, researchers analyzed health surveys done between 1999 and 2014 with nearly 42,500 adults in the United States. Although more than 80% of people with FH or severely high cholesterol were aware of their condition, only half were taking cholesterol-lowering statins. And among those who were, only one-third were taking optimal doses of the drugs.
Exercise may help outrun a family risk for heart disease
Research we're watching
Staying physically fit helps lower your risk of heart disease — even if the condition runs in your family, a new study finds.
Researchers relied on data from nearly half a million middle-aged and older adults in the United Kingdom. Over the six-year study, people with high levels of grip strength, self-reported physical activity, and cardiorespiratory fitness (as measured by a stationary bike test) were less likely than others to have a heart attack or stroke. That was true even among people with high genetic risk, based on whether they carried certain gene variants that have been linked to heart disease.
Tests your doctor may order to determine whether you have heart disease
Heart tests help show artery blockage and assess the risk of heart attack
If you are at high risk for heart disease or have a symptom such as shortness of breath or discomfort in your chest, your doctor may order certain heart tests. But there's more to testing than simply finding out if you have heart disease. Your doctor may also want to determine whether the fatty plaques inside your blood vessels pose a high, medium, or low risk for a heart attack. The answer will help determine whether you need treatment, and if so, which type of treatment will be best.
No single test is better than another, and no test is appropriate for everyone. "The best test for an individual is the one that provides the information needed to guide management," says Dr. Ron Blankstein, a cardiovascular imaging specialist at Harvard-affiliated Brigham and Women's Hospital.
Harnessing big data to help the heart
Machine learning may improve the way doctors detect heart disease.
Image: © exdez/Getty Images
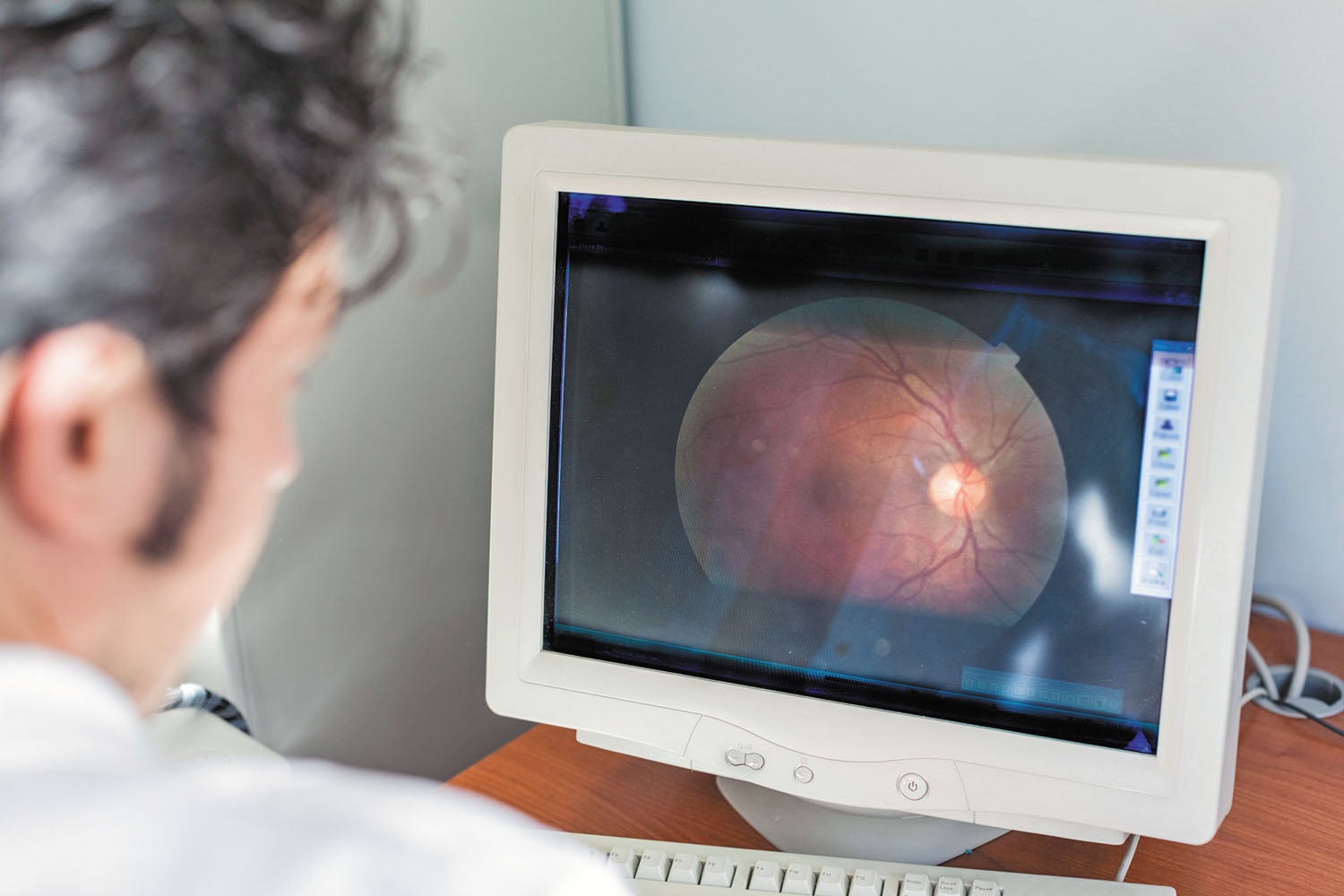
Imagine a world in which a photo of your eye — taken with your smartphone — could determine your risk of a heart attack, and your smartwatch could estimate your odds of experiencing a stroke. Sounds pretty futuristic, right?
In fact, preliminary studies showing the feasibility of both approaches have already been published. They're just two examples of the new wave of technology-based innovations (see "Transformative technologies") that are beginning to change health care as we know it.
Gene testing for antiplatelet drug response
Ask the doctor
Image: © wildpixel/Getty Images
Q. I understand there's a genetic test that can tell you how well you might respond to antiplatelet drugs. Do you recommend this test?
A. The short answer is no, not yet. For now, I think it is best to wait for the results from studies looking at personalized antiplatelet therapy. Also known as tailored medical therapy, personalized therapy refers to treatments that are based on your own information, including genetics. But first, I will address two other relevant questions: (1) what is antiplatelet therapy, and (2) who needs it?
Varicose veins: Clues to a deeper problem?
Leg veins that bulge just beneath the skin's surface are linked to a higher risk of deep-vein thrombosis.
Image: © gilaxia/Getty Images
Varicose veins are gnarled, bluish veins near the surface of the skin, usually on the legs and feet. Most people think of them as mainly a cosmetic problem, although varicose veins can cause a range of unpleasant symptoms, from a heavy, achy feeling in the legs to burning, throbbing, or itching sensations. Now, new research suggests that people with varicose veins may also have a higher risk of developing a clot in the deeper veins of the legs, known as deep-vein thrombosis or DVT.
"It's a good reminder for people with varicose veins to talk to their health care provider about their overall risk for vascular disease," says Dr. Gregory Piazza, assistant professor of medicine at Harvard Medical School. Most people with varicose veins won't experience a DVT. But it's still important to know the warning signs of this potentially dangerous condition (see "What is deep-vein thrombosis?") and to address any factors that might add to your risk, such as smoking, high blood pressure, and elevated cholesterol, he says.

Taming high blood pressure: How doctors find the right drug mix

Easy ways to add tofu to your diet

Red eyes, dry eyes, and more: Top questions for your eye doctor

The most effective types of exercise to lower blood pressure

Insufficient sleep linked to higher risk of atrial fibrillation

The best foods high in potassium — and why you need them

How to protect your health in a power outage

Can juicing help you get more fruits and vegetables?

Scoliosis treatment: Can it help as you get older?

Physical therapy provides modest improvement for chronic low back pain
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up