The smoldering epidemic
The number of new cases of hepatitis C is down, but millions are chronically infected and may not know it.
The identification of the virus that causes hepatitis C, a disease that affects the liver, has probably saved millions of lives. Before the discovery, two other hepatitis viruses — the hepatitis A and B viruses — had been identified, but neither was present in many cases of this disease. Patients were said to have "non-A, non-B hepatitis" — an awkward name that spoke of medicine's ignorance. In 1989, the mystery was solved. The viral culprit responsible for most cases of non-A, non-B hepatitis was found. Thereafter, those cases were called hepatitis C and their cause, the hepatitis C virus.
The hepatitis C virus is transmitted through blood, so before the virus was identified, the disease was spreading through blood transfusions, medical procedures such as kidney dialysis and organ transplantation, and needle sharing by intravenous drug users. The discovery of the virus meant that screening tests could be developed to find it in the blood supply. Diagnosis and treatment of the infection in people also became possible. Prior to the virus being discovered, about 200,000 Americans were newly infected with hepatitis C each year, according to federal government estimates. Today, it's estimated to be about a tenth of that number (and the number of confirmed cases is far fewer than that). Hepatitis C has also become a disease of middle age in the United States as people who were infected in the peak years in the 1980s have survived and gotten older. Hepatitis C is now more common among Americans in their 40s and 50s than in any other age group.
This isn't to say that hepatitis C is a conquered disease. Globally, as many as 170 million people are believed to be chronically infected with the virus. In the United States, it may be just over three million. Many infected people don't realize they have the disease because a lack of symptoms, or that they can unknowingly spread it to others. Hepatitis C can lead to liver cirrhosis and liver cancer, and about 10,000 American deaths each year are attributed to the disease. There's no vaccine, and the current treatments for chronic infection have bad side effects and aren't effective in many cases.
The A and the B of hepatitisThe hepatitis A virus is spread through the fecal-oral route. Fecal-oral transmission can occur if someone handles food after not washing his or her hands properly, or if the food (or water) came from tainted sources. The classic example is shellfish harvested from sewage-contaminated waters. Roughly 25,000 Americans are estimated to get hepatitis A each year, but the incidence — the number of new cases — is at record lows. Perhaps the single most important reason for the decline is the hepatitis A vaccine, which was introduced in 1995 and is now one of the vaccines that young children routinely receive. An increasing proportion of American hepatitis A cases are the result of infections acquired overseas in countries where the illness is more common, such as Mexico. The symptoms of hepatitis A include fever, nausea, abdominal pain, and the like. People can be sick for weeks, even months, but hepatitis A doesn't turn into a chronic infection like hepatitis B and C. Most people recover completely without treatment (except for symptom relief) and without liver damage. Like the hepatitis C virus, the hepatitis B virus is transmitted in blood, although semen and saliva can also be infectious. In the United States and other parts of the world where hepatitis B is relatively rare, the virus is spread primarily through unprotected sexual intercourse and the sharing of contaminated needles during intravenous drug use. Like the hepatitis C virus, the hepatitis B virus can survive outside the body for prolonged periods, so it's possible to get infected from sharing toothbrushes, razors, or other objects that might have blood on them. Federal health officials estimated that 43,000 new cases of hepatitis B occurred in the United States in 2007, the latest year for which such an estimate has been made. Hepatitis B incidence has been in steady decline in this country since 1991, when children began to be vaccinated against the disease. |
Symptoms and diagnosis
Frequently initial infection with the hepatitis C virus doesn't cause any notable symptoms. Some people (about 25%) may feel tired or feverish, lose their appetite, or have some pain in the upper right part of the abdomen, where the liver is located. When symptoms do occur, it's often one to three months after the exposure, so they may not prompt a visit to a doctor. Jaundice, the yellowing of the skin and whites of the eyes that's a classic sign of liver trouble, usually happens only when the disease gets more advanced.
Even when the infection persists and becomes a chronic condition, which happens about 80% of the time, hepatitis C often doesn't cause symptoms and can lurk undetected for decades. As a result, an infection is often discovered incidentally when a routine blood test shows a spike in certain liver-related enzymes. The doctor may follow up with more blood tests, like a special one that detects antibodies to the virus. Those tests aren't done routinely, but they are recommended for patients in the high-risk groups for hepatitis C, which in the United States includes, among others, those who received donated blood or organs before 1992 or blood clotting factors before 1987 and past or current users of intravenous drugs.
If the antibody test comes back positive, another test will probably be ordered to identify the genetic makeup of the virus. The hepatitis C virus has at least six different genotypes, which are referred to by numbers. In the United States, most people are infected with genotype 1, with most of the remaining infections being genotypes 2 and 3.
Avoiding cirrhosis
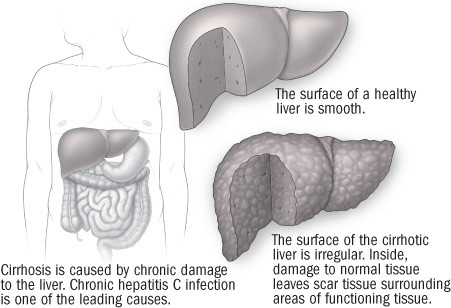
Even without symptoms, chronic hepatitis C can cause the liver to become inflamed as it fights the infection. Over time, the inflamed liver tissue can become scarred (this is called fibrosis) and replace healthy tissue. The liver is a resilient organ and can heal if the illness is caught and treated successfully. But if the scarring continues and becomes serious, the person is said to have cirrhosis (pronounced sir-ROW-sis). The most common causes of cirrhosis in the United States are alcohol abuse and chronic hepatitis B and C infections.
Once cirrhosis develops, a lot may go wrong and there's no shortage of symptoms. Fluids may accumulate in the legs (edema) or abdomen (ascites). Veins in other parts of the body may expand and bleed because blood doesn't flow properly through the liver. The blood itself can become laden with toxins that a healthy liver would normally filter out. Eventually the cirrhotic liver may fail altogether, which leaves a liver transplant as the only treatment option. Cirrhosis also greatly increases the risk for hepatocellular carcinoma, the most common type of liver cancer. A third of such cancers in the United States can be attributed to hepatitis C infections that led to cirrhosis.
Cirrhosis
|
The good news amid this gloom is that pretty much all of the serious consequences from chronic hepatitis C infection occur only after cirrhosis has developed, and that happens in a fraction of people with chronic hepatitis C infections. Studies have come up with different percentages, but 20% is a commonly cited figure. Why some people get cirrhosis while others live with chronic hepatitis C infections that cause little, if any, harm to their livers isn't completely understood, but several factors have been identified. People are more likely to develop cirrhosis if they drink alcohol, for example, or if they're also infected with HIV or hepatitis B. Age may matter: the risk of cirrhosis seems to go up if you were infected between the ages of 40 and 55. Some evidence suggests that African Americans are less likely than whites to develop cirrhosis. Results from a few studies suggest coffee might be protective.
The uncertainty of whether a chronic hepatitis C infection is going to lead to cirrhosis, along with the gradual nature of the process, often makes starting treatment a bit of a judgment call. Some people with chronic hepatitis C choose to delay treatment if tests show that their livers are healthy. Blood tests, ultrasound exams, and biopsies can be used to monitor how the liver is doing, so treatment can start later if the virus starts to cause liver damage.
Naturally, there's great interest in anything that might reduce the chances of that liver damage happening. The standard advice is pretty limited, though. People are told to avoid alcohol entirely because it both encourages replication of the hepatitis C virus and damages the liver on its own. Most medicines are safe for people with hepatitis C, although acetaminophen (Tylenol) use should be limited.
Some people with chronic hepatitis C infections take silymarin, an extract of the milk thistle plant. Milk thistle has long been thought to promote liver health, and some lab experiments have shown that it might protect liver cells, but solid proof is lacking. Trials are under way that may provide more evidence.
Treatment
The most effective current treatment for a chronic hepatitis C infection is a combination of pegylated interferon, taken as a weekly shot, and ribavirin (Copegus, Rebetol), taken as a pill. Eliminating the virus is the goal, so treatment is deemed successful if there's no evidence of the virus in the blood six months after therapy has stopped.
Interferon, a protein produced naturally by the body to fight viruses, is used to treat various cancers and other diseases. There are three major types of synthetic interferon, and the alfa variety has been used as a therapy for hepatitis C since the early 1990s. To help the interferon last longer in the body — and reduce the number of injections — it is "pegylated" by adding the chemical polyethylene glycol. Ribavirin, an antiviral medication, was approved as an add-on drug in 1998. The pairing of ribavirin with interferon has proved to be two or three times more effective than interferon alone.
The chances of successful treatment depend partly on the type of hepatitis C. About 80% of people in the United States infected with genotypes 2 and 3 respond well to pegylated interferon and ribavirin, but only about half of those infected with genotype 1 do.
Side effects are a problem: up to 80% of patients experience them. Generic "flu-like" symptoms, as well as fatigue, are common. But interferon-based therapy also has unusual effects on emotions and mood, and is associated with depression, emotional swings, or bouts of anger. Another drawback to the current regimen is that the medications need to be taken for a long time: six months for treatment of genotypes 2 and 3 and almost a year for genotype 1.
Doctors have tinkered with the interferon-based therapy with mixed results. One approach has been to combine it with novel compounds designed to interfere with replication of the hepatitis C virus, which mutates quickly inside cells. Two of the most promising drugs being tested in patients, telaprevir and boceprevir, inhibit protease enzymes, which is how many of the HIV drugs work.
Dr. Raymond Chung, a leading hepatitis C researcher at Massachusetts General Hospital, says scientists are looking at ways to attack the virus at different stages in its life cycle. One strategy is to prevent the hepatitis C virus from entering or exiting liver cells, so the virus can't assemble itself inside and then leave to infect other cells. Researchers are also looking for ways to boost the body's immune response to the hepatitis C virus. Dr. Chung heads a research consortium that received a $15 million federal grant to investigate how the virus manages to elude the immune system so well.
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.