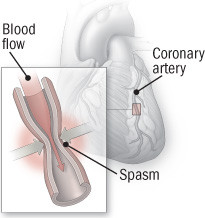
Coronary artery vasospasm
A sudden spasm of the coronary arteries can feel like a heart attack or even cause a small one.
Variant angina. Coronary syndrome X. Prinzmetal's angina. All have this in common: a sudden constriction of coronary arteries that reduces blood supply to part of the heart, causing chest pain and other symptoms similar to any heart attack.
Vasospasm is the sudden narrowing of an artery. It happens when the muscles within the vessel's wall quickly contract and stay that way. Vasospasm can occur anywhere in the body. It is part of the process can cause a minor stroke and is associated with some migraine symptoms. In the fingers and toes, it is responsible for Raynaud's phenomenon. In the coronary arteries, which supply the hardworking heart muscle with oxygen-rich blood, a sudden coronary vasospasm of one or more vessels can reduce blood flow to part of the heart.
Causes, consequences of a coronary vasospasm
A fast-paced chemical and nerve conversation continually fine-tunes blood flow to the heart muscle. This lets the heart instantly respond to changes in posture, exercise, emotions, temperature, and other stimuli.
This coronary yin and yang works flawlessly in most people. In some, though, a sudden imbalance in chemical messengers can set off vasospasm. It can occur during the transition from sleep to waking, during an episode of stress or anxiety, or as a result of hyperventilation. It can be triggered by various legal and illegal drugs, such as cocaine, amphetamines, anti-migraine drugs, and herbal supplements like Ephedra or bitter orange.
The sudden reduction in blood flow due to vasospasm sets off alarms in and around the heart. Oxygen-starved heart tissue sends warning signals that are felt as pain in the chest, left arm, jaw, and back.
In a relatively healthy individual, a single episode of coronary vasospasm doesn't usually have long-term consequences. In someone with clogged coronary arteries or a weakened heart, though, vasospasm can throw the heart into a potentially dangerous rhythm. A coronary vasospasm can also rupture a fragile cholesterol-filled plaque inside an artery, setting off a full=blown heart attack.
Coronary artery vasospasm
The sudden constriction of a coronary artery can reduce blood flow to part of the heart, and feel like a heart attack. |
Treating vasospasm
Coronary vasospasm deserves the same fast action. A big difference is how the coronary arteries appear on an angiogram, the special x-ray done by injecting dye directly into the coronary arteries. In someone with classic angina, an angiogram shows one or more cholesterol-clogged arteries; in those with a classic heart attack, it shows a completely blocked artery. In someone with vasospasm, though, the coronary arteries can look clear and healthy.
To stop coronary vasospasm, doctors usually rely on nitroglycerin or another fast-acting nitrate to relax constricted arteries. After that, prevention of future episodes is the key.
Calcium-channel blockers are effective for preventing coronary vasospasm. These include amlodipine (generic, Norvasc), diltiazem (generic, Cardizem, others), and long-acting nifedipine (generic, Adalat). Another option is a long-acting nitrate, such as isosorbide dinitrate (generic, Isordil) or sustained-release nitroglycerin. Calcium-channel blockers and nitrates work in different ways to relax blood vessels, and so make a good pair when one of them isn't enough to quell vasospasm.
Other therapies may include cholesterol-lowering statins, magnesium supplements, and sildenafil (Viagra), the widely used erectile dysfunction drug.
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.