On Veterans Day, don’t let the “invisible wounds” of PTSD remain hidden
Millions of American men and women have served in the Armed Forces, protecting and defending our nation. Although many died, most returned home to “pick up their lives.” That isn’t always easy. For some veterans, the trauma of war changes the brain in ways that can cause long-term problems.
War-related mental health problems have been with us for centuries. They probably afflicted Achilles, the Greek warrior at the center of Homer’s Iliad. During the Civil War, such problems were called “nostalgia” or “soldier’s heart.” In World War I, the term was “shell shock.” “Combat neurosis” and “battle fatigue” were the preferred descriptions during World War II and the Korean War. By the late 1970s, the condition had evolved into post-traumatic stress disorder (PTSD).
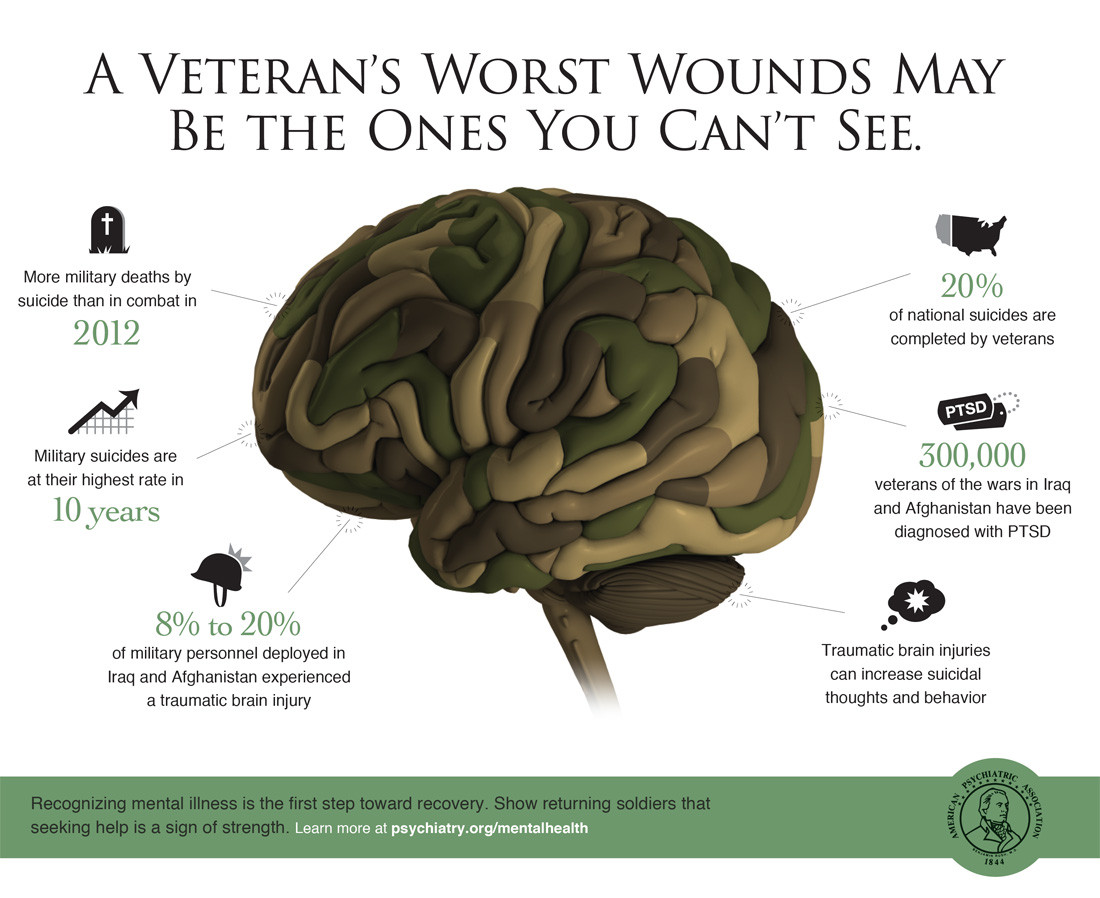
According to the American Psychiatric Association, more than 300,000 veterans of the wars in Iraq and Afghanistan have been diagnosed with PTSD. Countless others probably suffer from this condition but have never sought help for it. Even sadder, in 2012 more military deaths were caused by suicide than by combat. You can see other compelling statistics in the infographic below.
Many veterans don’t seek help because they feel there’s a stigma attached to these invisible wounds. That’s a shame, because help is available. “Seeking help for a mental health issue is a sign of strength, not weakness,” says former U.S. Rep. Patrick Kennedy, in a video encouraging the American family to “embrace our veterans so they stop suffering in silence.”
If you know a veteran, thank him or her for having served our nation. And if you think he or she is having trouble, bolster your courage and ask. Beginning the conversation may open the door to healing.
About the Author

Patrick J. Skerrett, Former Executive Editor, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.