Kaposi sarcoma
- Reviewed by Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
What is Kaposi sarcoma?
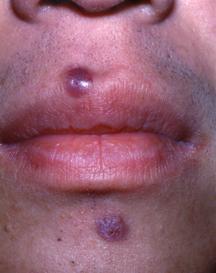
Kaposi sarcoma is a type of cancer caused by the virus human herpes virus 8. The tumors appear as red or purple patches on the skin, mouth, lungs, liver, or gastrointestinal tract.
First described in 1872, Kaposi sarcoma was considered rare until the HIV epidemic began. An aggressive form of the disease, HIV-related Kaposi sarcoma, occurs in people with severely weakened immune systems.
|
|
The four types of Kaposi's sarcoma are
- Classic Kaposi sarcoma. This is a rare, slow-growing skin tumor, usually affecting males of Italian, Middle Eastern, or Eastern European Jewish ancestry.
- African (endemic) Kaposi sarcoma. This form of the disease occurs more often in young males in certain African countries. Usually it is a slow-growing tumor, but in some cases, it can be aggressive, invading bone and tissue under the skin.
- Immunosuppressive treatment-related Kaposi sarcoma. People who are taking immunosuppressive medication after an organ transplant may develop this form of the disease. It sometimes improves if the medication is reduced or changed.
- HIV-related Kaposi sarcoma. HIV-related Kaposi sarcoma usually appears as a rapidly progressing tumor affecting the skin or mouth, although it can also affect the lymph nodes, gastrointestinal tract, lungs, liver, or spleen. The incidence of this type of Kaposi sarcoma has dramatically decreased due to highly active retroviral therapy (HAART) for people with HIV.
Symptoms of Kaposi sarcoma
The first symptoms of Kaposi sarcoma are usually red, purple, or brown patches, plaques, or nodules (bumps) on the skin. (The abnormal growth of small blood vessels just below the skin gives the lesions their purplish hue.) They may look like bruises. In the classic, African, and immunosuppressive forms of the disease, the lesions usually grow slowly and develop over years. As the disease worsens, the legs may swell. In some cases, it will spread to other organs.
In the HIV-related form, the cancer is much more aggressive, often growing to cover large areas and forming tumor-like masses. These lesions are usually soft and spongy at first, but they become hard and solid over time. The surface of the tumor may develop open ulcers that can become infected.
HIV-related Kaposi sarcoma is rarely confined to the skin. It often affects the mouth, lymph nodes, lungs, liver, spleen, and gastrointestinal tract. When the tumor involves the lungs, it often causes coughing, shortness of breath, and wheezing. The disease often progresses rapidly in the lungs. It may cause respiratory failure, which can be fatal.
When the disease involves the gastrointestinal tract, it rarely causes symptoms until it becomes very advanced. People may then develop symptoms of intestinal obstruction (nausea, vomiting, and abdominal pain) or bloody stools. If the lymph nodes become involved, severe swelling can occur, usually in the legs, arms, face, or scrotum (in men).
Diagnosing Kaposi sarcoma
If your doctor suspects Kaposi sarcoma, he or she will examine your body, looking for the following:
- lesions on your skin
- lesions inside your mouth
- enlarged lymph nodes.
Your doctor may also check the inside your rectum using a gloved, lubricated finger, as Kaposi sarcoma lesions can develop there.
Your doctor will ask if you have HIV or another condition that may be suppressing your immune system. If you do not know if you have HIV, your doctor will recommend an HIV test.
If you have HIV, your doctor will ask you several questions about your condition:
- When were you diagnosed?
- What medications are you currently taking? Have you taken other medications?
- What other HIV-related illnesses (opportunistic infections) have you had?
- What were the results of your most recent lab tests (such as CD4 count and viral load)?
Kaposi sarcoma can be confirmed with a biopsy. In this test, a small piece of tissue is removed and examined under a microscope.
If you have Kaposi sarcoma, your doctor will try to determine how far it has spread by examining you and asking you several questions:
- Do you have a cough, or are you short of breath? (This could indicate that the cancer has reached the lungs.)
- Do your legs swell up? (This suggests the cancer has reached lymph nodes.)
- Do you experience nausea, vomiting, or abdominal pain? Do you have blood in your stool? (This suggests the cancer is affecting the gastrointestinal tract.)
If your doctor suspects you may have Kaposi sarcoma in your lungs, she or he may order a chest x-ray, CT scan, MRI, and/or bronchoscopy. During a bronchoscopy, doctors thread a slender tube with a camera through the mouth into the lungs. Once in place, she or he can look directly at the tumor and remove tissue samples.
Other diagnostic tests, such as a gastrointestinal endoscopy and colonoscopy, may be ordered if your doctor suspects you may have Kaposi sarcoma in your gastrointestinal tract. Your gastrointestinal tract includes (but is not limited to) your esophagus, stomach, small intestine, and large intestine (colon and rectum).
Expected duration of Kaposi sarcoma
There is no cure for Kaposi sarcoma. It is a lifelong condition. However, the symptoms will improve with treatment (such as HAART for people with HIV.)
Preventing Kaposi sarcoma
There is no way to prevent the milder forms of Kaposi sarcoma (classic, African, and immunosuppression-related). The most effective way to avoid developing HIV-related Kaposi sarcoma is to prevent the spread of HIV. People who have HIV can decrease their risk of Kaposi sarcoma by taking HAART.
Treating Kaposi sarcoma
The goals of treatment are to ease symptoms, shrink the tumor(s), and prevent the disease from getting worse. The treatment depends on the type of Kaposi sarcoma, the size and location of the tumor(s), the extent of the disease, your CD4 count, and your overall health. Treatments include:
- topical therapy: applying a medicated gel directly to the skin lesion(s)
- surgery: removing the cancer cells
- cryotherapy: freezing the cancer cells to kill them
- chemotherapy: using drugs to kill the cancer cells
- radiation therapy: using radiation to kill the cancer cells
- biological therapy (immunotherapy): strengthening the body's immune system to better fight the cancer.
In people with HIV, the lesions will improve with treatment of that condition. Typically, this involves taking antiretroviral medications to strengthen the immune system.
In organ transplant patients with immunosuppressive treatment-related Kaposi sarcoma, the condition may improve with a change in immune-suppressing drugs. However, doing so can increase the risk of organ rejection.
When to call a professional
See a doctor if you have skin changes that fit the description of Kaposi sarcoma. If you have HIV and Kaposi sarcoma, you will need immediate treatment; your doctor may need to change or add medications to treat the HIV.
If you have not been tested for HIV and you think you may have Kaposi sarcoma, talk to your doctor right away. He or she will counsel you about risk factors for HIV and ask if you have symptoms suggestive of HIV. These include:
- swollen lymph nodes
- night sweats
- fevers
- fatigue
- weight loss.
If you are at risk of HIV, your doctor will recommend a blood test to check for this virus. Early diagnosis of HIV is important, because the prognosis for both HIV and Kaposi sarcoma improves dramatically with treatment.
Prognosis
The outlook for Kaposi sarcoma depends on the form of the disease you have. Milder forms are rare and develop slowly. People with classic Kaposi sarcoma usually die of other causes or develop a second type of cancer. (About one-third of people with classic Kaposi sarcoma develop another cancer.) Immunosuppression-related Kaposi sarcoma often improves by changing the drug or its dose.
The most important factor in the prognosis for HIV-related Kaposi sarcoma is how well the immune system functions. Developing Kaposi sarcoma suggests that the immune system is highly impaired. People with this disease usually die of a different HIV-related infection. People who take HAART have a better prognosis.
Additional info
American Cancer Society (ACS)
https://www.cancer.org/
Infectious Diseases Society of America
https://www.idsociety.org/
National Institute of Allergy and Infectious Diseases (NIAID)
https://www.niaid.nih.gov/
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.