Colonoscopy
- Reviewed by Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
What is it?
Colonoscopy is an examination of your complete colon, or large intestine. To perform colonoscopy, your doctor uses an instrument called a colonoscope, which is a flexible viewing tube with lenses, a small TV camera, and a light on one end. Through bundles of flexible glass fibers (fiber-optic technology) and a small video computer chip, the colonoscope scans the inside of your colon and transmits images to a video screen.

During colonoscopy, your doctor can check your colon for abnormal growths called polyps, sites of bleeding, and for other conditions such as colitis. The procedure may take up to an hour and is done in a special endoscopy suite or the outpatient area of a hospital. Although the colonoscope is lubricated and bends easily, you will be lightly sedated to minimize any discomfort.

What it's used for
Colonoscopy is used to look at the lining of your colon. This makes it useful in detecting colon cancer, polyps, inflammation, and other problems of the gastrointestinal tract. Periodic colonoscopy is still considered the best method to screen for polyps and early cancer. For people at average risk, colonoscopy or an alternative screening test should begin between the ages of 45 and 50.
Colonoscopy should begin earlier in people with a high risk of colorectal cancer due to a family history of colorectal cancer, chronic inflammatory bowel disease, or certain hereditary syndromes, including familial adenomatous polyposis. Regular colonoscopy at more frequent intervals also is recommended for anyone who has already had either a cancerous growth or precancerous polyp removed from the bowel.
Colonoscopy may be done as a follow-up exam after a positive fecal occult blood test. It also can be used to identify the source of rectal bleeding or to confirm that there are areas of colitis (inflammation of the colon) in someone who has symptoms.
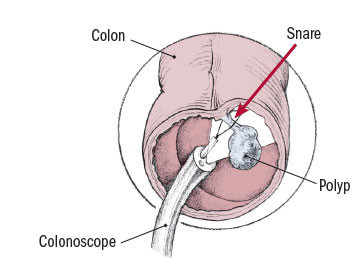
If your doctor sees a suspicious area during colonoscopy, he or she can use an attachment at the end of the colonoscope to take a biopsy (small tissue sample) to be examined in a laboratory. If a polyp is found during colonoscopy, your doctor may use a wire loop attachment to remove the entire polyp so that it can be sent for laboratory analysis.
Preparation
Your bowel needs to be empty during colonoscopy to give your doctor a clear view of your intestinal wall. To help empty your bowel, your doctor will give you specific directions about using laxatives the day before the procedure. Different doctors may recommend different laxative regimens, with or without enemas. In some cases, you will also need to follow a liquid diet for one to two days before the procedure with a full fast (nothing by mouth) after midnight the evening before the procedure. Your doctor will give you more exact details about diet when you schedule your colonoscopy exam. Because you will receive medication during colonoscopy that may make you feel drowsy, arrange for a friend or family member to help you get home from the doctor's office.
How it's done
You will put on a hospital gown, and the doctor's assistant will record your vital signs, including temperature, pulse, and blood pressure. A pulse oximeter (to measure the oxygen saturation level of your blood) may be placed on your finger, ear, or toe, and electrocardiograph (EKG) recording patches may be placed on your chest to monitor your heartbeat. You will be asked to lie on your side on an examination table, with the lower portion of your body covered by a sheet. As your doctor directs, you may be asked to raise one or both of your knees up to your chest.
You will be given medication that will lightly sedate you before the doctor inserts a lubricated, flexible colonoscope into your rectum. He or she will thread the colonoscope to the end of your colon and, as necessary, pump a small amount of air through the colonoscope to open up your intestinal passage for a clearer view. Your doctor may also take a stool sample or biopsy from inside your bowel.
Follow-up
After colonoscopy is done, you can get dressed. However, because you may still feel drowsy from the medication, a friend or family member should help you get home. You may pass gas that was pumped into your bowel during the examination.
You may return to your normal diet whenever you wish. If your doctor took a stool sample or biopsy during the exam, check back in a few days for the results.
Risks
In about one to three out of every 1,000 colonoscopies, a serious complication will occur. This can include heavy bleeding or a puncture or injury to the bowel wall.
When to call a professional
Call your doctor immediately if you see rectal bleeding after colonoscopy or if you feel faint, dizzy, or short of breath or have palpitations. Also call your doctor if you have abdominal pain with or without nausea and vomiting, or if you develop a fever, chills, severe headache, or muscle aches.
Additional info
American Cancer Society (ACS)
https://www.cancer.org/
National Cancer Institute (NCI)
https://www.cancer.gov
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.












